Lymphedema: Difference between revisions
| Line 61: | Line 61: | ||
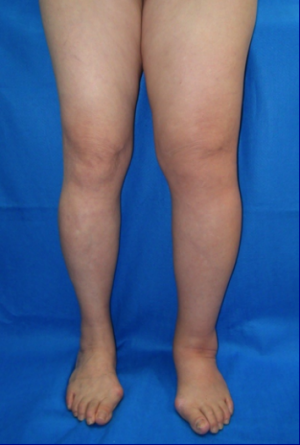
*Generally asymptomatic, although may have feeling of heaviness in limb | *Generally asymptomatic, although may have feeling of heaviness in limb | ||
*Swelling not evident on exam | *Swelling not evident on exam | ||
|| | |[[File:1lymphedema.png|thumb]] | ||
| | |||
|- | |- | ||
| Stage I (mild)|| | | Stage I (mild)|| | ||
Revision as of 20:30, 26 March 2019
Background
- Lymphedema is swelling due to abnormal accumulation of interstitial protein rich fluid and fibroadipose tissue.
- Occurs when lymphatic load exceeds capacity in the lymphatic system
Etiology
Primary[1]
- Congenital Lymphedema (6-12%) - before age 2
- Lymphedema Precox (77-94%) - at onset of puberty
- Lymphedema Tarda (11%) - after age 35
Secondary
- Cancer and cancer treatment (Lymphadenectomy, Radiotherapy) [2]
- Breast Cancer - most common
- Sarcoma
- Lower Extremity Melanoma
- Gynecologic Cancer
- Genitourinary Cancer
- Head and neck cancer
- Infection
- Lymphatic filariasis
- Tuberculosis
- Recurrent Skin Infections (eg. cellulitis, erysipelas)
- Lymphadenitis
- Obesity
- Inflammatory disorders
- Dermatitis
- Sarcoidosis
- Arthritis
- Rheumatoid arthritis
- Psoriatic arthritis
- Juvenile Idiopathic Arthritis
Clinical Features
- Slowly progressive swelling, may be pitting at onset
- Feeling of heaviness, tightness, or discomfort
- Severe cases have dermal thickening with skin becoming dry, firm, and hyperkeratotic
- Occurs due to cutaneous fibrosis and adipose deposition.
- Stemmer Sign - positive if unable to pinch and lift skin at the base of second toe or finger.
Differential Diagnosis
Unilateral leg swelling
- Gravitational
- Venous stasis
- Thrombophlebitis
- Lymphedema
- Medications
- Deep venous thrombosis (uncomplicated)
- Leg or foot infection
- Fracture
- Compartment syndrome
- Limb hypertrophy
- Hypertrophy of soft tissue or bone (Klippel-Trenaunay syndrome)
- Overgrowth of body part (Proteus Syndrome)
- Lipedema
- Tumor
- Post-thrombotic Syndrome
- Causes of bilateral pedal edema
Evaluation
- Diagnosis is primarily made clinically. See clinical features above.
- Rule out alternative diagnoses (e.g. duplexes to rule out DVT if indicated)
- Additional non-ED studies may include:
- Duplex Ultrasound
- Lymphoscintigraphy
- Computed Tomography
- Magnetic Resonance Imaging/Lymphography
- Indocyanine Green (ICG) Lymphangiography
- Genetic Testing
Clinical Staging (by International Society of Lymphology) [3]
| Stage | Signs & Symptoms | Image | |
| Stage 0 (asymptmatic) |
|
||
| Stage I (mild) |
|
||
| Stage II (moderate) |
|
||
| Stage III (severe) |
|
Management[4][3]
- General Measures
- Self-monitoring - for size, sensation, color, temperature, skin condition
- Limb elevation
- Diet and exercise - maintain ideal body weight. Recommended to use compression garments during exercise.
- Avoid skin infection/injury
- Compression Therapy - bandaging, garments, intermittent pneumatic compression
- Physiotherapy - manual lymphatic drainage
- Contraindicated in presence of cellulitis, neoplasm, DVT, moderate-severe heart failure
- Surgical Referral
Disposition
- Discharge if uncomplicated
See Also
External Links
References
- ↑ Szuba A, Rockson SG. Lymphedema: classification, diagnosis and therapy. Vasc Med 1998; 3:145-56
- ↑ Cormier JN, Askew RL, Mungovan KS, et al. Lymphedema beyond breast cancer: a systematic review and meta-analysis of cancer-related secondary lymphedema. Cancer 2010; 116:5138-49
- ↑ 3.0 3.1 International Society of Lymphology. The diagnosis and treatment of peripheral lymphedema: 2013 Consensus Document of the International Society of Lymphology. Lymphology 2013; 46:1-11
- ↑ Rockson SG. Lymphedema. Am J Med 2001; 110:288-95