Neonatal seborrhoeic dermatitis: Difference between revisions
No edit summary |
Neil.m.young (talk | contribs) (Text replacement - "==Diagnosis==" to "==Evaluation==") |
||
| Line 15: | Line 15: | ||
{{Neonatal rashes DDX}} | {{Neonatal rashes DDX}} | ||
== | ==Evaluation== | ||
*Clinical diagnosis | *Clinical diagnosis | ||
**Consider immunosuppression or [[HIV]] in severe or widespread lesions | **Consider immunosuppression or [[HIV]] in severe or widespread lesions | ||
Revision as of 13:12, 22 July 2016
Background
- Also known as cradle cap, infantile seborrhoeic dermatitis, crusta lactea, milk crust, and honeycomb disease
- Starts between 2-6wk of life; improves by 6 months
- Malassezia furfur, non-contagious fungus
Clinical Features
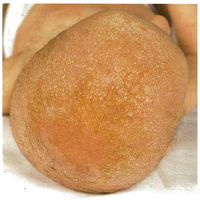
- Greasy yellow-red scales
- Proclivity for scalp (cradlecap), but may find around ears, cheeks, neck
- Not pruritic
- Also axilla and groin where there are significant sebaceous glands
Differential Diagnosis
Neonatal Rashes
- Atopic dermatitis
- Candidiasis
- Diaper dermatitis
- Erythema toxicum neonatorum
- Neonatal acne
- Psoriasis
- Seborrheic dermatitis
- Tinea capitis
- Impetigo
- Contact dermatitis
- Perianal streptococcal dermatitis
- Milia
- Miliaria
- Mongolian spots
- Omphalitis
- Pustular melanosis
- Sucking blisters
Evaluation
- Clinical diagnosis
- Consider immunosuppression or HIV in severe or widespread lesions
Management
- Salicylic acid shampoo (Sebulex) OR
- Application of mineral oil followed by washing and removal of scales with comb
- Avoid topical steroids
Disposition
- Outpatient