Noninvasive ventilation
(Redirected from CPAP)
Background
Mechanism of Action
- Augments inspiratory/expiratory pressures throughout a spontaneous respiratory cycle.
- Recruits compressed alveoli to reduce atelectasis.
- Prevents small airway collapse during inspiration.
- Counteracts intrinsic PEEP (Positive End Expiratory Pressure).
- Decreased both preload and afterload in heart failure exacerbations.
- Improves lung compliance and V/Q matching.
- Decreases the work of breathing.
- Reduces need for intubation and mortality in acute cardiogenic pulmonary edema[1] and acute COPD exacerbation[2]
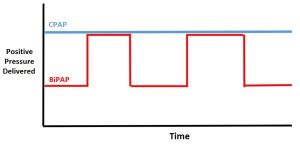
CPAP vs. BPAP
- CPAP = PEEP = EPAP
- Use for isolated hypoxia
- Increasing CPAP increases oxygenation
- BPAP = PEEP + (IPAP = Inspiratory Pressure Support)
- Use for hypoxia and hypoventilation (decreases work of breathing)
- Increasing IPAP (specifically IPAP-CPAP) increases ventilation
- Note: BiPAP is a brand name of one of the BPAP machines. Both names are often used interchangeably.
Indications
Contraindications
- Obtunded patients
- Uncooperative patients
- Vomiting or inability to protect the airway (aspiration risk)
- Facial trauma or burns
- Facial, esophageal, or gastric surgery
- Poor mask fit
Procedure
- Prepare intubation equipment in case of BPAP/CPAP failure.
- Position the patient in a 30-90° upright position.
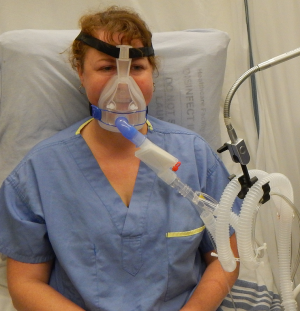
- Apply the mask.
- Select the appropriately-sized mask.
- Secure it in place by fastening the Velcro straps.
- Note: Some experts recommend allowing the patient to get used to the mask first, PRIOR TO starting the positive airway pressures.
- Prepare the patient.
- Patients will often require frequent coaching throughout this process.
- In moderately anxious patients, consider low-dose fentanyl, a benzodiazepine or ketamine to assist with patient-ventilator synchrony.
- Adjust the settings.
- For BPAP, begin with an IPAP of 8-10 cm H2O and an EPAP of 2-4 cm H2O.
- Gradually titrate upward IPAP and EPAP 1-2 cm every 5-15 minutes with a goal IPAP 10-16 cm H2O and EPAP of 8-10 cm H2O depending upon patient response.
- Continue close monitoring.
- A doctor, nurse, or respiratory therapist should be with the patient at all times during BPAP/CPAP use.
Complications
- Skin irritation
- Nasal bridge pain
- Mucosal dryness
- Eye irritation
- Gastric distention
- Decreased cardiac output
- Barotrauma (rarely)
See Also
Mechanical Ventilation Pages
- Noninvasive ventilation
- Intubation
- Mechanical ventilation (main)
- Miscellaneous
External Links
- Merk Manual - How To Do Noninvasive Positive Pressure Ventilation
- NUEM - Non-Invasive Positive Pressure Ventilation in the ED
References
- ↑ Peter JV, Moran JL, Phillips-Hughes J, Graham P, Bersten AD. Effect of non-invasive positive pressure ventilation (NIPPV) on mortality in patients with acute cardiogenic pulmonary oedema: a meta-analysis. Lancet. 2006;367(9517):1155-1163. doi:10.1016/S0140-6736(06)68506-1
- ↑ Ambrosino N, Vagheggini G. Non-invasive ventilation in exacerbations of COPD. Int J Chron Obstruct Pulmon Dis. 2007;2(4):471-476.