Caustic ingestion
Background
Caustics
- Substances that cause damage on contact with body surfaces
- Degree of injury determined by pH, concentration, volume, duration of contact
- Acidic agents cause coagulative necrosis
- Alkaline agents cause liquefactive necrosis (considered more damaging to most tissues)
- Corrosive agents have reducing, oxidising, denaturing or defatting potential
Alkalis
- Accepts protons → free hydroxide ion, which easily penetrates tissue → cellular destruction
- Liquefactive necrosis and protein disruption may allow for deep penetration into surrounding tissues
- Examples
- Sodium hydroxide (NaOH), potassium hydroxide (KOH)
- Lye present in drain cleaners, hair relaxers, grease remover
- Bleach (sodium hypochlorite) and Ammonia (NH3)
- Sodium hydroxide (NaOH), potassium hydroxide (KOH)
Acids
- Proton donor → free hydrogen ion → cell death via denatured protein → coagulation necrosis and eschar formation, which limits deeper involvement
- However, due to pylorospasm and pooling of acid, high-grade gastric injuries are common
- Mortality rate is higher compared to strong alkali ingestions
- However, due to pylorospasm and pooling of acid, high-grade gastric injuries are common
- Can be systemically absorbed and → metabolic acidosis, hemolysis, AKI
- Examples
- Hydrochloric acid (HCl), hydrofluoric acid (HF), Sulfuric acid (H2SO4), Phosphoric acid, Oxalic Acid, Acetic acid
- Found in: auto batteries, drain openers, toilet bowl, metal cleaners, swimming pool cleaners, rust remover, nail primer
- Hydrochloric acid (HCl), hydrofluoric acid (HF), Sulfuric acid (H2SO4), Phosphoric acid, Oxalic Acid, Acetic acid
Clinical Features
- Signs and symptoms are inadequate to predict presence or severity of injury after caustic ingestion [3]
- Exam eyes and skin (splash and dribble injuries may easily be missed)
- GI tract injury
- Dysphagia, odynophagia, drooling, epigastric pain, vomiting
- Laryngotracheal injury
- Dysphonia, stridor, respiratory distress
- Occurs via aspiration of caustic or vomitus or inhalation of acidic fumes
Differential Diagnosis
Caustic Burns
- Caustic ingestion
- Caustic eye exposure (Caustic keratoconjunctivitis)
- Caustic dermal burn
- Airbag-related burns
- Hydrofluoric acid
- Tar burn
- Cement burn
Evaluation
Labs
Only necessary in patients with significant injury or volume of ingestion
- CBC
- Chemistry
- Lactic Acid
- In Alkali ingestion, presence of acidemia or hyperlactemia is likely indicative of clinically significant tissue injury[4]
- ECG
- Calcium and Magnesium level (if hydrofluoric acid exposure)
- Free Fluoride binds rapidly to calcium and magnesium leading to severe hypocalcemia and hypomagnesemia that can be life threatening
- Acetaminophen and Salicylate levels (in patients with concern for intentional ingestion)
Imaging
- 3-View CXR
- Look for free air under the diaphragm or signs of mediastinal air[5]
- Button battery XR - two rings, will likely need to remove it no matter where it is, whether post-pyloric or pre-pyloric
- CT with contrast
- Consider when perforated viscus is suspected but CXR is negative
Management
- Prevent provider and continued patient exposure to the caustic agent by removing all clothing and decontaminating the patient
- There is a possible benefit of water ingestion immediately after ingestion of a powdered caustic to irrigate adherent materials in oropharynx/esophagus if no airway concerns to prevent prolonged injury from the powder adhering to tissues[6]
Airway Management
- Monitor closely for stridor, airway edema, hoarseness, or other signs of airway injury
- Intubate early if signs of airway injury exist, first sign of voice changes, inability to tolerate secretions or stridor before airway becomes more difficult to manage.
- Consider awake fiberoptic or video laryngoscopy if concern for difficult airway
- Blind nasotracheal intubation is contraindicated due to the potential for perforations and false passages
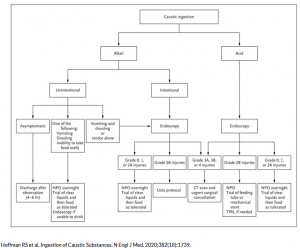
Endoscopy
Should be performed in the first 24 to 48 hours after ingestion (too early can underestimate extent of injury, too late increases risk of wound softening and perforation).
- Indications
- Intentional ingestion (higher likelihood of high volume ingestion)
- Unintentional ingestion with signs of:
Esophageal Stricture Mitigation[7]
- Discuss with GI or medical toxicologist
- For grade IIb or higher esophageal burns:
- Methylprednisolone (1 g/1.73 m2 per day for 3 days)
- Ranitidine
- Ceftriaxone
- Total parenteral nutrition
- Sucralfate, Mitomycin C
Surgical Intervention
- Indicated for:
- Perforation
- Peritoneal signs
Caustic Specific Treatment
- Can include chelation, dialysis, or specific antidotes
- Especially in caustics that cause systemic toxicity
Controversial or Contraindicated
- Antibiotics
- No evidence to support or reject the use of prophylactic antibiotics
- Only indicated if also giving steriods (see stricture mitigation above)
- Activated charcoal
- May infiltrate damaged mucosa & interfere with EGD
- Only consider when coingestants pose a risk for severe systemic toxicity
- Zinc chloride and mercuric chloride systemic absorptions may outweigh interference with endoscopy[8]
- Gastric lavage
- Contraindicated due to potential to cause reflux of caustic agent into esophagus, creating more damage
- Blind nasogastric-tube insertion for irrigation can cause thermal injury through neutralization
- Dilution with water or milk causes vomiting, elevating risk for perforation
- Possible benefit only for solid alkali ingestions
- Neutralization generates excess heat
- Milk or magnesium citrate only for hydrofluoric acid ingestion
Disposition
- All patients with symptoms from a caustic ingestion should be admitted for at least 24 hours of observation
- All patients with intentional ingestion should be evaluated by psych prior to discharge
Prognosis
- Depending on severity may have full return of mobility and function or can progress to perforation followed by stricture formation
- Days 2-14 post-injury are associated with highest tissue friability / risk of perforation
- Strictures typically develop in the first 2 months, higher risk in those with circumferential esophageal erosions (Grade 2B burns and above)
- High-grade caustic burns associated with 1000x increase in esophageal adenocarcinoma or squamous-cell carcinoma
See Also
References
- ↑ Wasserman RL, Ginsburg CM. Caustic substance injuries. J Pediatr. 1985;107(2):169-174. doi:10.1016/s0022-3476(85)80119-0
- ↑ Harley EH, Collins MD. Liquid household bleach ingestion in children: a retrospective review. Laryngoscope. 1997;107(1):122-125. doi:10.1097/00005537-199701000-00023
- ↑ Gaudreault, P. et al. Predictability of esophageal injury from signs and symptoms: a study of caustic ingestion in 378 children. Pediatrics. 1983;71(5):767-770.
- ↑ Hoffman et al. Ingestion of Caustic Substances. N Engl J Med. 2020. Apr;382(18):1739-1748
- ↑ Muhletaler C. et al. Acid corrosive esophagitis: radiographic findings. AJR Am J Roentgenol. 1980. Jun;134(6):1137-40. PMID: 6770621
- ↑ Hoffman et al. Ingestion of Caustic Substances. N Engl J Med. 2020. Apr;382(18):1739-1748
- ↑ High Doses of Methylprednisolone in the Management of Caustic Esophageal Burns. Pediatrics 2014;133:e1518–e1524
- ↑ Contini S, Scarpignato C. Caustic injury of the upper gastrointestinal tract: a comprehensive review. World J Gastroenterol. 2013;19(25):3918-3930. PMID 23840136