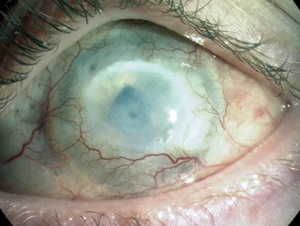
Caustic keratoconjunctivitis
(Redirected from Chemical Burns (Eye))
Background
- Chemical burn to eye
- Alkali injuries are more severe than acidic injuries, and are considered an ophthalmologic emergency
- Prognosis is determined by the extent of injury at the limbus and area/depth of injury to cornea
Caustics
- Substances that cause damage on contact with body surfaces
- Degree of injury determined by pH, concentration, volume, duration of contact
- Acidic agents cause coagulative necrosis
- Alkaline agents cause liquefactive necrosis (considered more damaging to most tissues)
- Corrosive agents have reducing, oxidising, denaturing or defatting potential
Alkalis
- Accepts protons → free hydroxide ion, which easily penetrates tissue → cellular destruction
- Liquefactive necrosis and protein disruption may allow for deep penetration into surrounding tissues
- Examples
- Sodium hydroxide (NaOH), potassium hydroxide (KOH)
- Lye present in drain cleaners, hair relaxers, grease remover
- Bleach (sodium hypochlorite) and Ammonia (NH3)
- Sodium hydroxide (NaOH), potassium hydroxide (KOH)
Acids
- Proton donor → free hydrogen ion → cell death via denatured protein → coagulation necrosis and eschar formation, which limits deeper involvement
- However, due to pylorospasm and pooling of acid, high-grade gastric injuries are common
- Mortality rate is higher compared to strong alkali ingestions
- However, due to pylorospasm and pooling of acid, high-grade gastric injuries are common
- Can be systemically absorbed and → metabolic acidosis, hemolysis, AKI
- Examples
- Hydrochloric acid (HCl), hydrofluoric acid (HF), Sulfuric acid (H2SO4), Phosphoric acid, Oxalic Acid, Acetic acid
- Found in: auto batteries, drain openers, toilet bowl, metal cleaners, swimming pool cleaners, rust remover, nail primer
- Hydrochloric acid (HCl), hydrofluoric acid (HF), Sulfuric acid (H2SO4), Phosphoric acid, Oxalic Acid, Acetic acid
Keratoconjunctivitis Types
- Atopic keratoconjunctivitis
- Caustic keratoconjunctivitis
- Secondary to chemical orbital exposure
- Epidemic keratoconjunctivitis
- Highly contagious viral (adenovirus) conjunctivitis, associated with watery discharge
- Ultraviolet keratitis
- Secondary to UV light exposure
- Keratoconjunctivitis sicca
- Associated with autoimmune disorders such as Sjögren syndrome, sarcoidosis, rheumatoid arthritis, and scleroderma
Conjunctivitis Types
Clinical Features
- Severe ocular pain, blepharospasm, reduced visual acuity
- Altered ocular pH (normal = 7.0-7.2)
- Appearance
- Conjunctival injection OR blnnching
- Chemosis, hemorrhage, epithelial defects
- Corneal loss OR edema
- Perilimbal ischemia (white ring around iris)
- Concerning due to co-location of corneal stem cell layer (re-epitheliazation relies on migration of limbal stem cells)
Alkali Burns
- Rapid penetration through cornea and anterior chamber
- Causes liquefaction necrosis from hydroxyl ions combining with fatty acids
- Elevated IOP may be seen in alkali injury[3]
- Acute injury liquefaction necrosis and ischemia which can be graded on degree of limbal and corneal involvement
- Early sequelae corneal edema and elevated IOP
- Later injury after one week - corneal breakdown, ulceration, perforation because of collagenase activity exceeds synthesis
Acid Exposure
- Injury related to length of exposure and concentration of chemical
- Causes coagulation necrosis and protein precipitation thus limits depth of penetration
- Delayed complications corneal and conjunctival scarring, vascularization, glaucoma, uveitis
Other Chemicals
- Most exposures produce only simple irritation
Roper-Hall classification[4]
| Grade | Cornea Appearance | Limbal Ischemia | Prognosis |
| I | Clear | None | Good |
| II | Hazy/iris details visible | <1/3 | Good |
| III | Opaque/iris details obscured | 1/3-1/2 | Guarded |
| IV | Opaque/iris details obscured | >1/2 | Poor |
Differential Diagnosis
Caustic Burns
- Caustic ingestion
- Caustic eye exposure (Caustic keratoconjunctivitis)
- Caustic dermal burn
- Airbag-related burns
- Hydrofluoric acid
- Tar burn
- Cement burn
Unilateral red eye
- Nontraumatic
- Acute angle-closure glaucoma^
- Anterior uveitis
- Conjunctivitis
- Corneal erosion
- Corneal ulcer^
- Endophthalmitis^
- Episcleritis
- Herpes zoster ophthalmicus
- Inflamed pinguecula
- Inflamed pterygium
- Keratoconjunctivitis
- Keratoconus
- Nontraumatic iritis
- Scleritis^
- Subconjunctival hemorrhage
- Orbital trauma
- Caustic keratoconjunctivitis^^
- Corneal abrasion, Corneal laceration
- Conjunctival hemorrhage
- Conjunctival laceration
- Globe rupture^
- Hemorrhagic chemosis
- Lens dislocation
- Ocular foreign body
- Posterior vitreous detachment
- Retinal detachment
- Retrobulbar hemorrhage
- Traumatic hyphema
- Traumatic iritis
- Traumatic mydriasis
- Traumatic optic neuropathy
- Vitreous detachment
- Vitreous hemorrhage
- Ultraviolet keratitis
^Emergent diagnoses
^^Critical diagnoses
Bilateral red eyes
- Painful
- Painless
Evaluation
- Generally a clinical diagnosis
Management
Caustic Ocular Exposure Management
- Eye irrigation
- Immediate irrigation is the most important treatment for caustic ocular injury, and should be started before comprehensive evaluation
- Irrigate affected eye(s) with copious amounts of fluid (no consensus on volume or length of time)[5]
- NS, LR, or BSS (Buffered Saline Solution) preferred in the hospital setting[6], but tap water is acceptable, especially in pre-hospital setting.
- Goal is to remove caustic agent and restore normal ocular pH (7.0-7.2)
- Do NOT attempt to neutralize pH by adding base to an acidic burn or acid to an alkali burn
- Use of morgan lens or eyelid speculum will assist with getting more fluid in contact with cornea
- Remove particulate matter
- Evert both lids, remove any visible particulate matter with cotton-tipped applicator
- Anesthesia
- Topical anesthetic (e.g. tetracaine) to help with discomfort.
- Other options include cycloplegics (e.g. atropine, cyclopentolate), IV/IM/PO analgesics
- Antibiotics
- Erythromycin ophthalmic ointment QID for minor burns
- Topical fluoroquinolone for more severe burns
- Control inflammation
- Topical steroids - prednisolone 1% ophthalmic QID for 1 week[7]
- Limit topical steroid use to 10 days to avoid corneal breakdown.[8]
- Ophthalmology consultation for all but minor burns (Severe exposures may require debridement or other surgical intervention)
Disposition
Admit
- Pediatric patient
- Corneal haziness, opacity, or limbal ischemia (paleness at limbus)
Discharge
With 24hr ophthalmology follow-up
- If only has corneal epithelial injury
- Encourage use of artificial tears and other lubricating eyedrops
See Also
References
- ↑ Wasserman RL, Ginsburg CM. Caustic substance injuries. J Pediatr. 1985;107(2):169-174. doi:10.1016/s0022-3476(85)80119-0
- ↑ Harley EH, Collins MD. Liquid household bleach ingestion in children: a retrospective review. Laryngoscope. 1997;107(1):122-125. doi:10.1097/00005537-199701000-00023
- ↑ Lin, M.P., et al., Glaucoma in patients with ocular chemical burns. American journal of ophthalmology, 2012. 154(3): p. 481-485 e1.
- ↑ Gupta N et al. Comparison of Prognostic Value of Roper Hall and Dua Classification Systems in Acute Ocular Burns. Br J Ophthalmol. 2011;95(2):194-198. http://www.medscape.com/viewarticle/739100.
- ↑ Chau JP, Lee DT, Lo SH. A systematic review of methods of eye irrigation for adults and children with ocular chemical burns. Worldviews Evid Based Nurs. 2012 Aug;9(3):129-38.
- ↑ Herr RD, White GL Jr, Bernhisel K, Mamalis N, Swanson E. Clinical comparison of ocular irrigation fluids following chemical injury. Am J Emerg Med. 1991 May;9(3):228-31.
- ↑ Dohlman, C.H., F. Cade, and R. Pfister, Chemical burns to the eye: paradigm shifts in treatment. Cornea, 2011. 30(6): p. 613-4.
- ↑ Donshik, P.C., et al., Effect of topical corticosteroids on ulceration in alkali-burned corneas. Archives of ophthalmology, 1978. 96(11): p. 2117-20.