Diabetic ketoacidosis (peds)
(Redirected from DKA (peds))
This page is for pediatric patients. For adult patients, see: diabetic ketoacidosis
Background
- DKA + altered mental status = cerebral edema until proven otherwise
Clinical Features
- May be the initial presenting of an unrecognized Type-1 diabetes mellitus patient
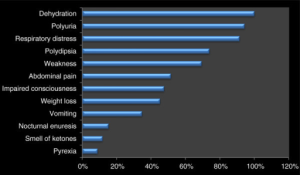
- Signs/symptoms may include:
- Tachypnea, Kussmaul's breathing
- Polyuria, polydipsia, polyphagia, poor weight gain/weight loss
- Signs of dehydration
- Abdominal pain, nausea/vomiting
- Altered mental status, drowsiness, lethargy
- Breath fruity odor (acetone)
- Perform a thorough neurologic exam as cerebral edema increases mortality significantly, especially in children
- +/- signs/symptoms of precipitating trigger for decompensation (e.g. pneumonia, cellulitis)
- Keep in mind that the initial presentation of sepsis with dehydration can look very similar to DKA
Differential Diagnosis
Hyperglycemia
Diabetic Emergencies
- Diabetic ketoacidosis (DKA)
- Diabetic ketoacidosis (peds)
- Hyperosmolar hyperglycemic state (HHS)
- Nonketotic hyperglycemia
- Euglycemic DKA (SGLT-2 inhibitors, pregnancy, fasting)
Diabetes Mellitus (New or Known)
- Type 1 diabetes mellitus (new-onset or uncontrolled)
- Type 2 diabetes mellitus (new-onset or uncontrolled)
- Medication noncompliance or insulin pump malfunction
- Gestational diabetes
- Latent autoimmune diabetes of adults (LADA)
Medication/Drug-Induced
- Corticosteroids (most common drug-induced cause)
- Thiazide diuretics
- Atypical antipsychotics (olanzapine, clozapine, quetiapine)
- Beta-blockers (especially non-selective)
- Phenytoin
- Tacrolimus, cyclosporine (transplant patients)
- Protease inhibitors (HIV antiretrovirals)
- Catecholamines (epinephrine, norepinephrine infusions)
- SGLT-2 inhibitors (paradoxical DKA with euglycemia)
- Total parenteral nutrition (TPN)
- Dextrose-containing IV fluids (iatrogenic)
- Niacin
- Pentamidine (initially hyperglycemia, then hypoglycemia from beta-cell destruction)
Physiologic Stress Response
- Sepsis / critical illness (stress hyperglycemia — very common in the ED)
- Trauma / major surgery / burns
- Acute coronary syndrome / myocardial infarction
- Stroke (especially hemorrhagic)
- Pancreatitis (both a cause and consequence)
- Shock (any etiology)
- Pain (catecholamine surge)
- Seizure (postictal)
- Physiologic stress alone rarely causes glucose >200 mg/dL in non-diabetics; glucose >200 in a "stress response" should prompt evaluation for undiagnosed diabetes or prediabetes
Endocrine
- Cushing syndrome / Cushing disease (cortisol excess)
- Pheochromocytoma (catecholamine excess)
- Hyperthyroidism / thyroid storm
- Acromegaly (growth hormone excess)
- Glucagonoma (rare)
- Somatostatinoma (rare)
Pancreatic
- Pancreatitis (acute or chronic — destruction of islet cells)
- Pancreatic malignancy (adenocarcinoma, neuroendocrine tumors)
- Post-pancreatectomy
- Cystic fibrosis-related diabetes
- Hemochromatosis (iron deposition in pancreas — "bronze diabetes")
Toxic/Overdose
- Iron toxicity (hepatic injury → impaired glucose regulation)
- Salicylate toxicity (can cause both hyper- and hypoglycemia)
- Sympathomimetic toxicity (cocaine, methamphetamine)
- Calcium channel blocker toxicity (impairs insulin secretion)
- Carbon monoxide toxicity (stress response)
Other
- Renal failure (chronic kidney disease, acute kidney injury — impaired insulin clearance AND insulin resistance)
- Cirrhosis / hepatic failure (impaired glycogenolysis regulation)
- Pregnancy (gestational diabetes, steroid administration for fetal lung maturity)
- Parenteral nutrition (TPN, dextrose-containing fluids)
- Post-transplant diabetes (immunosuppressants)
Complications of Diabetes (Not Causes of Hyperglycemia)
These are associated conditions that may be present alongside hyperglycemia but do not themselves cause elevated glucose:
- Diabetic foot infection
- Diabetic peripheral neuropathy
- Cerebral edema in DKA
- Diabetic retinopathy
- Diabetic nephropathy
Evaluation
Workup
- Point of care glucose (and potassium, if available)
- VBG
- Chem 7
- Magnesium
- Phosphorus
- Serum ketones (or beta-OH and acetone)
- Urinalysis
- CBC
- Urine pregnancy (if appropriate)
- Consider infectious workup to identify trigger
Diagnosis
- Hyperglycemia (>200)
- Acidosis
- pH <=7.30 or bicarb <=15
- +ketonemia (>1:2 serum dilution)
General Treatment
- Initial bolus 20ml/kg NS x 1 (repeat boluses only for shock or poor perfusion)[1]
Manage Hydration[2]
- If K+<5.5
- 0.45% NS (or NS) + 20 KPhosat 1.5 x maintenance rate
- When BS <300, change to D5/0.45%NS (or NS) +20 KPhos at 1.5 x maintenance rate (maintain BS 150-250)
- 0.45% NS (or NS) + 20 KPhosat 1.5 x maintenance rate
- In a retrospective study, lactated ringers when compared with normal saline was associated with lower total cost and rate of development of cerebral edema.[3]
Manage Acidosis[4]
- Insulin 0.1 units/kg/hr IV drip IV drip — Do not start if K+ <4.0; decrease to 0.05 units/kg/hr when transitioning to SC
- Do not start if K+ <4.0 (replete K+ first)
- Continue until HCO3 >15 and pH >7.3, then transition to SC insulin
- Decrease infusion to 0.05 units/kg/hr until 1hr after SC insulin initiated
Potassium
- if <2.5, hold insulin and give 1 meq/kg potassium KCL in IV over 1hr
- No insulin until K >2.5
- if >2.5 but <3.5 give 40-60 meq/L in IV until K >3.5
- if >3.5 but <5.5 give 30-40 meq/L in IV for K = 3.5 - 5
- if >5.5, then check K q1hr
Bicarbonate[5]
- No evidence supports the use of sodium bicarb in DKA, with a pH >6.9
- However, no studies have been performed for patients with pH <6.9 and the most recent ADA guidelines recommend it for patients with pH <7.1
- Only consider for:
- Critically ill (hemodynamic compromise from decreased contractility) AND
- pH <7.0
- Sodium bicarbonate 0.5-2 mEq/kg over 1-2 hr IV — Correction should never exceed pH >7.1 or bicarb >10
- Correction should never exceed pH > 7.1 or bicarb >10
Monitor for Complications[6]
- Cerebral edema (1% of DKA)
- Acute change in mental status
- Signs of herniation
- If present, see Cerebral Edema in DKA
Disposition
- Admit all (usually to PICU, if on insulin drip) unless
- Known diabetes
- pH >7.35 and bicarb >20
- Known and resolving precipitant for DKA
Complications
See Also
- Diabetes mellitus (main)
- Diabetic ketoacidosis (main)
- EBQ:Sodium Bicarbonate use in DKA
- Clinical Trial of Fluid Infusion Rates for Pediatric Diabetic Ketoacidosis
External Links
References
- ↑ Cooke & Plotnick. Management of diabetic ketoacidosis in children and adolescents. Pediatr Rev. 2008 Dec;29(12):431-5
- ↑ Cooke & Plotnick. Management of diabetic ketoacidosis in children and adolescents. Pediatr Rev. 2008 Dec;29(12):431-5
- ↑ Bergmann, K. R., Jennifer Abuzzahab, M., Nowak, J., Arms, J., Cutler, G., Christensen, E., … Kharbanda, A. (2018). Resuscitation With Ringerʼs Lactate Compared With Normal Saline for Pediatric Diabetic Ketoacidosis. Pediatric Emergency Care, 1.
- ↑ Cooke & Plotnick. Management of diabetic ketoacidosis in children and adolescents. Pediatr Rev. 2008 Dec;29(12):431-5
- ↑ EBQ:Sodium Bicarbonate use in DKA
- ↑ Cooke & Plotnick. Management of diabetic ketoacidosis in children and adolescents. Pediatr Rev. 2008 Dec;29(12):431-5