Dysphagia
Background
- Most patients with dysphagia have an identifiable, organic cause
- Assume malignancy in patients >40yo with new-onset dysphagia
- Medications can cause dysphagia from esophageal mucosal injury or reduced lower esophageal sphincter tone.
- CVA is most common cause of oropharyngeal dysphagia
Clinical Features
- Difficulty swallowing
- Sensation of food stuck
- Chest pain
- Dysphagia categories[1]
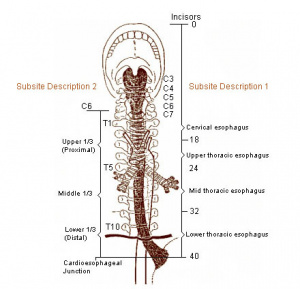
- Oropharyngeal dysphagia - difficulty initiating swallowing (coughing, chocking, nasal regurgitation)
- Esophageal dysphagia
- Mechanical obstruction - usually solid food only
- Neuromuscular disorder - solid or liquid food
Transfer dysphagia (oropharyngeal)
- Discoordination in transferring bolus from pharynx to esophagus
- Etiology
- Neuromuscular disease (80% of cases)
- Localized disease
- Pharyngitis, aphthous ulcers, PTA, Zenker diverticulum
- Symptoms
- Gagging, coughing, inability to initiate swallow, need for repeated swallows
Transport dysphagia (esophageal)
- Improper transfer of bolus from upper esophagus into stomach
- Etiology
- Obstructive disease (85% of cases)
- Foreign body, carcinoma, webs, strictures, thyroid enlargement
- Motor disorder
- Achalasia, peristaltic dysfunction (nutcracker esophagus), scleroderma
- Obstructive disease (85% of cases)
- Symptoms
- Food "sticking," retrosternal fullness with solids (and eventually liquids), odynophagia
Differential Diagnosis
Dysphagia
- Oropharyngeal dysphagia
- CVA
- Parkinson's disease
- Brain stem tumors
- Degenerative disease - ALS, MS, Huntington's
- Postinfectious - polio, syphilis
- Peripheral neuropathy
- Myasthenia gravis
- Polymyositis, dermatomyositis
- Muscular dystrophy
- Esophageal dysphagia
- Achalasia
- Diffuse esophageal spasm
- Ingested foreign body
- Esophageal web
- Malignancy, mediastinal masses
- Schatzki Ring
- Scleroderma
- Strictures - peptic, radiation, chemical, medication-induced
- Vascular compression
- Zenker's diverticulum
Evaluation
- Evaluate for underlying etiology (e.g. rule out new neuro dysfunction)
- Neck x-ray (AP and lateral)
- Helpful in presumed transfer dysphagia and proximal transport dysphagia
- CXR
- Helpful in presumed transport dysphagia
Management
- Referral to GI or ENT for direct laryngoscopy or video-esophagography
Disposition
See Also
References
- ↑ Spieker MR. Evaluating Dysphagia. Am Fam Physician. 2000 Jun 15;61(12):3639-3648.