Amebiasis
(Redirected from Entamoeba histolytica)
==Background==
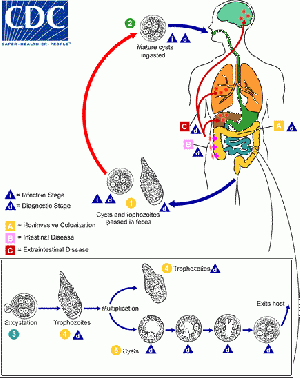
- Fecal oral transmission of Entamoeba histolytica cyst
- Most infection asymptomatic
- Excystation in intestinal lumen
- Trophozoites adhere and colonizes large intestine forming new cysts or invade the intestinal mucosa to cause colitis or abscesses
- Liver abscess - 10x more common in men
- Incubation period usually 2-4 weeks, but may range from a few days to years
==Clinical Features== *Asymptomatic vs. dysentery vs. extraintestinal abscesses
- Intestinal- several weeks of crampy abdominal pain, weight loss, watery or bloody diarrhea
- Liver abscess-fever, cough, RUQ or epigastric pain, right-sided pleural pain or referred shoulder pain +/- GI upset
- Hepatomegaly with tenderness over the liver a typical finding
- Abscess rupture can involve associated peritoneum, pericardium, or pleural cavity
- Extrahepatic amebic abscesses in the lung, brain, and skin are rare
==Differential Diagnosis== ===Dysentery=== *Infectious- shigella, salmonella, campylobacter, E. Coli.
- Noninfectious- Inflammatory bowel disease, ischemic colitis, diverticulitis, AV malformation.
Hepatic abscess
- Pyogenic abscess
- Aerobic: Escherichia coli, Klebsiella, Pseudomonas
- Anaerobic: Enterococcus, bacteroides, anaerobic streptococci
- Echinococcosis
- Amebiasis
- Benign cysts/malignancy
- Tuberculosis
- Mycosis
Fever in traveler
- Normal causes of acute fever!
- Malaria
- Dengue
- Leptospirosis
- Typhoid fever
- Typhus
- Viral hemorrhagic fevers
- Chikungunya
- Yellow fever
- Rift valley fever
- Q fever
- Amebiasis
- Zika virus
Acute diarrhea
Infectious
- Viral (e.g. rotavirus)
- Bacterial
- Campylobacter
- Shigella
- Salmonella (non-typhi)
- Escherichia coli
- E. coli 0157:H7
- Yersinia enterocolitica
- Vibrio cholerae
- Clostridium difficile
- Parasitic
- Toxin
Noninfectious
- GI Bleed
- Appendicitis
- Mesenteric Ischemia
- Diverticulitis
- Adrenal Crisis
- Thyroid Storm
- Toxicologic exposures
- Antibiotic or drug-associated
- Inflammatory bowel disease
Watery Diarrhea
- Enterotoxigenic E. coli (most common cause of watery diarrhea)[1]
- Norovirus (often has prominent vomiting)
- Campylobacter
- Non-typhoidal Salmonella
- Enteroaggregative E. coli (EAEC)
- Enterotoxigenic Bacteroides fragilis
Traveler's Diarrhea
- Giardia lamblia
- Cryptosporidiosis
- Entamoeba histolytica
- Cyclospora
- Clostridium perfringens
- Listeriosis
- Helminth infections
- Marine toxins
- Ciguatera
- Scombroid poisoning
- Paralytic shellfish poisoning
- Neurotoxic shellfish poisoning
- Diarrheal shellfish poisoning
==Evaluation== ===Labs=== *CBC
- Chem
- LFTs
- Stool PCR
- Diagnostic gold standard
- 100% sensitive and specific
- Stool or abscess microscopy
- <60% SN; unreliable diagnostic test[2]
- Stool, serum, or abscess fluid antigen
- Indirect hemagglutination (antibody)
===Imaging=== *Abdominal Ultrasound
- 58-98% SN for liver abscess (depending on size/location)
- Abdominal CT
- Alternative to ultrasound; equally effective in identifying abscess
==Management== ===Asymptomatic colonization=== *Paromomycin or diloxanide
Colitis
- Metronidazole 750mg PO q8h x 5-10 days
===Liver abscess=== *Metronidazole, tinidazole, paromomycin, or diloxanide
- Consider drainage of abscess by IR if no response to antibiotics in 5 days, abscess > 5cm, or left lobe involvement
==Disposition== *Admission
- Admit if signs of shock, sepsis, or peritonitis
- Patients with toxic megacolon should be admitted for surgical intervention.
- Discharge
- Patients who are non-toxic and able to tolerate oral hydration/PO meds can be discharged with outpatient follow-up
==External Links== *Merk Manual - Amebiasis
==References==