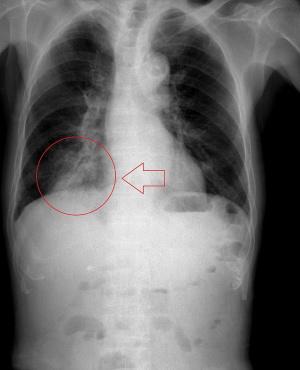
Aspirated foreign body
(Redirected from Foreign body aspiration)
Background
- Most common in young children (1-3 years old)
- Consider in any child with respiratory symptoms
- Object can be lodged in upper airway (20% of cases) or bronchus (80%)
Foreign Body Types
- Ear foreign body
- Nasal foreign body
- Ocular foreign body
- Aspirated foreign body
- GI
- Soft tissue foreign body
Clinical Features
- History of eating or handling a small object (or being unsupervised near one) followed by sudden onset coughing, dyspnea
- Onset of respiratory symptoms may sometimes be delayed >24 hours
- Dyspnea, tachypnea, respiratory distress, hypoxia
- Sudden collapse, cardiac arrest
- Cough, gagging
- Stridor, dysphonia (if stuck at level of larynx)
- Wheezing, decreased breath sounds (If lower airway)
- Wheezing not responsive to bronchodilators
- Fever, pneumonia symptoms if retained
Differential Diagnosis
Stridor
Trauma
- Larynx fracture
- Tracheobronchial tear/injury
- Thyroid gland injury/trauma
- Tracheal injury
- Electromagnetic or radiation exposure
- Burns, inhalation injury
Infectious Disorders
- Bacterial tracheitis
- Diphtheria
- Tetanus
- Tracheobronchial tuberculosis
- Poliomyelitis, paralytic, bulbar, or acute
- Fungal laryngitis
Abscesses
- Retropharyngeal abscess
- Epiglottitis, acute
- Peritonsillar abscess
- Laryngotracheobronchitis (croup)
- Retropharyngeal abscess
Neoplastic Disorders
- Neoplasms/tumors
Allergic and Auto-Immune Disorders
- Spasmodic/tracheobronchitis
- Angioedema/Angioneurotic edema
Metabolic, Storage Disorders
- Cerebral Gaucher's of infants (acute)
- Tracheobronchial amyloidosis
Biochemical Disorders
Congenital, Developmental Disorders
- Angioedema/Angioneurotic edema, hereditary
Psychiatric Disorders
- Somatization disorder
Anatomical or Mechanical
- Foreign body aspiration
- Acute gastric acid/aspiration syndrome
- Airway obstruction
- Neck compartment hemorrhage/hematoma
- Paradoxical vocal fold motion [1]
Vegetative, Autonomic, Endocrine Disorders
- Esophageal free reflux/GERD syndrome
- Laryngospasm, acute
- Bilateral vocal cord paralysis
- Hypoparathyroidism
Poisoning
Chronic Pediatric Conditions
- Laryngotracheomalacia[2]
- Subglottic stenosis or prior intubation
- Vascular ring (double aortic arch)
- Vocal cord dysfunction/paroxysmal vocal fold movement
Pediatric stridor
<6 Months Old
- Laryngotracheomalacia
- Accounts for 60%
- Usually exacerbated by viral URI
- Diagnosed with flexible fiberoptic laryngoscopy
- Vocal cord paralysis
- Stridor associated with feeding problems, hoarse voice, weak and/or changing cry
- May have cyanosis or apnea if bilateral (less common)
- Subglottic stenosis
- Congenital vs secondary to prolonged intubation in premies
- Airway hemangioma
- Usually regresses by age 5
- Associated with skin hemangiomas in beard distribution
- Vascular ring/sling
>6 Months Old
- Croup
- viral laryngotracheobronchitis
- 6 mo - 3 yr, peaks at 2 yrs
- Most severe on 3rd-4th day of illness
- Steeple sign not reliable- diagnose clinically
- Epiglottitis
- H flu type B
- Have higher suspicion in unvaccinated children
- Rapid onset sore throat, fever, drooling
- Difficult airway- call anesthesia/ ENT early
- H flu type B
- Bacterial tracheitis
- Rare but causes life-threatening obstruction
- Symptoms of croup + toxic-appearing = bacterial tracheitis
- Foreign body (sudden onset)
- Marked variation in quality or pattern of stridor
- Retropharyngeal abscess
- Fever, neck pain, dysphagia, muffled voice, drooling, neck stiffness/torticollis/extension
Evaluation
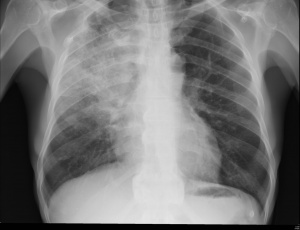
Chest x-ray of an adult with obstructive pneumonia in the right lung evidenced by hypodense area. This is from a blockage in the respiratory tract leading to an infection distal to the obstruction.
- CXR
- Useful to confirm diagnosis, does not rule out
- Negative in >50% of tracheal foreign bodies, 25% of bronchial foreign bodies[3], and may be missed if very small and/or radiopaque
- Inspiratory/expiratory films may show relative hyperinflation proximal to obstruction on end-expiration
- Consider lateral decubitus films on right and left side
Management
Complete Airway Obstruction
- If conscious: Heimlich maneuver, chest thrusts (obese or pregnant patients), back-blow/chest thrust (infants)
- If object visible, remove manually (don't push it further into airway!)
- Laryngoscopy, remove visualized object with Magill forceps
- If unsuccessful, bag-valve mask or intubate (may dislodge object and improve situation to partial or more distal obstruction)
- If unable to intubate, may need cricothyrotomy (though will not help if obstruction distal to cricothyroid)
Partial Obstruction
- Supplemental O2
- Allow patient to assume position of comfort
- Monitor closely
- May need rigid bronchoscopy to remove
- Consider consulting ENT, anesthesia (inhalational induction will decrease risk of pushing foreign body into harder-to-reach area)
- Post-removal: consider dexamethasone, bronchodilators and/or racemic epinephrine, and antibiotics for pneumonia
Disposition
See Also
- Respiratory distress
- Stridor, Stridor (Peds)
- PALS (Main), Newborn resuscitation
- Difficult airway algorithm, Airway sizes (peds)
- Aspiration pneumonia and pneumonitis
- Esophageal foreign body, Nasal foreign body
External Links
References
- ↑ Vocal Cord Dysfunction on Internet Book of Critical Care https://emcrit.org/ibcc/vcd/
- ↑ Ernst A, Feller-Kopman D, Becker HD, Mehta AC. Central airway obstruction. Am J Respir Crit Care Med 2004
- ↑ Zerella JT, Dimler M, McGill LC, Pippus KJ: Foreign body aspiration in children: value of radiography and complications of bronchoscopy. J Pediatr Surg 33: 1651, 1998.