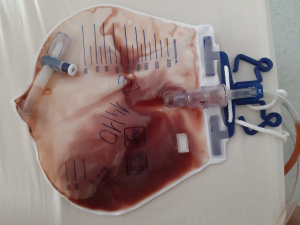
Hematuria
This page is for adult patients; for pediatric patients see hematuria (peds)
Background
- Hematuria can be macroscopic/gross or microscopic
- Microscopic hematuria generally defined as >3 RBCs per high-power field of an uncontaminated sample
- Hematuria can also be divided into glomerular and nonglomerular causes
- Make sure hematuria is not myoglobin (due to rhabdo), hemoglobinuria (due to hemolysis), or bleeding from non-urinary source (ex. menstruation)
- Hematuria + pain suggests UTI or nephrolithiasis
- Hematuria + no pain suggests malignancy, hyperplasia, or vascular cause
Common Causes
- Younger adults
- Older adults
- Any age
- Schistosomiasis (most common cause worldwide)
Clinical Features
Types of hematuria
- Initial hematuria
- Blood at beginning of micturition with subsequent clearing
- Suggests urethral disease
- Intervoid hematuria
- Blood between voiding only (voided urine is clear)
- Suggests lesions at distal urethra or meatus
- Total hematuria
- Blood visible throughout micturition
- Suggests disease of kidneys, ureters, or bladder
- Terminal hematuria
- Blood seen at end of micturition after initial voiding of clear urine
- Suggests disease at bladder neck or prostatic urethra
- Gross hematuria
- Indicates lower tract cause
- Microscopic hematuria
- Tends to occur with kidney disease
- Brown urine with RBC casts and proteinuria
- Suggests glomerular source
- Clotted blood
- Indicates source below kidneys
Blunt Trauma[1]
Renal injuries are associated with:
- Sudden deceleration injury without hematuria
- Gross Hematuria
- Microscopic Hematuria with Shock (SBP<90 mm Hg)
- The degree of hematuria does not correlate with significance of renal injury
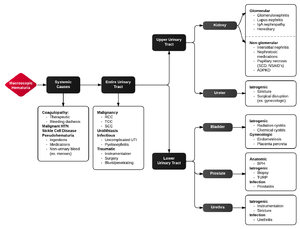
Differential Diagnosis
Hematuria
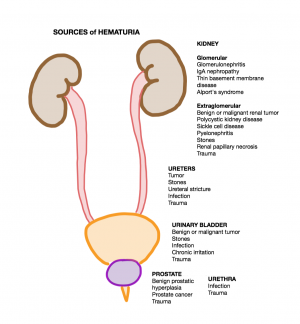
Sources of hematuria.
- Urologic (lower tract)
- Any location
- Iatrogenic/postprocedure
- GU trauma
- Infection
- Kidney stone
- Erosion or mechanical obstruction by tumor
- Ureter(s)
- Dilatation of stricture
- Bladder
- Transitional cell carcinoma
- Vascular lesions or malformations
- Chemical or radiation cystitis
- Prostate
- Benign prostatic hypertrophy
- Prostatitis
- Urethra
- Stricture
- Diverticulosis
- Foreign body
- Endometriosis (cyclic hematuria with menstrual pain)
- Any location
- Renal (upper tract)
- Glomerular
- Glomerulonephritis
- IgA nephropathy (Berger disease)
- Lupus nephritis
- Hereditary nephritis (Alport syndrome)
- Toxemia of pregnancy
- Serum sickness
- Erythema multiforme
- Nonglomerular
- Interstitial nephritis
- Pyelonephritis
- Papillary necrosis: sickle cell disease, diabetes, NSAID use
- Vascular: arteriovenous malformations, emboli, aortocaval fistula
- Malignancy
- Polycystic kidney disease
- Medullary sponge disease
- Tuberculosis
- Renal trauma
- Glomerular
- Hematologic
- Primary coagulopathy (e.g., hemophilia)
- Pharmacologic anticoagulation
- Sickle cell disease
- Myoglobinuria - positive blood, no RBCs: rhabdomyolysis
- Hemoglobinuria - positive blood, no RBCs
- Miscellaneous
- Eroding abdominal aortic aneurysm
- Malignant hypertension
- Loin pain–hematuria syndrome
- Renal vein thrombosis
- Exercise-induced hematuria
- Cantharidin (Spanish fly) poisoning
- Stings/bites by insects/reptiles having venom with anticoagulant properties
- Schistosomiasis
- Sickle Cell Trait
Red or Purple Urine
- Hematuria
- Hemoglobinuria
- Porphyria
- Myoglobinuria (rhabdomyolysis)
- Foods
- Blackberries
- Beets
- Blackberries
- Rhubarb
- Food coloring
- Fava beans
- Drugs
- Purple urine bag syndrome
- Uric acid crystalluria (neonates)
Evaluation
Workup
Labs
- Urinalysis
- Urine microscopy can show abnormal RBC morphologies suggesting glomerular source of hematuria
- Microscopic hematuria associated with proteinuria suggests glomerular disease and requires further investigation (as an outpatient)
- Urine dipstick may be performed quickly in some centers but has high false-positive rate[2]
- CBC - for anemia and thrombocytopenia
- BMP - for renal function
- Coags
Imaging
- Utilize multiphasic CT urography ("hematuria protocol") to assess for pathology in the kidney and urinary collecting system[3]
- A noncontrast phase is useful for visualizing stones or hydronephrosis
- A nephrographic phase has contrast enhancing renal parenchyma, useful for pyelonephritis and renal tumors
- A delayed excretory phase visualizes urothelial and bladder tumors
- Ultrasound useful to assess for hydronephrosis or a Abdominal Aortic Aneurysm
- Ultimately, cystoscopy and/or kidney biopsies may be necessary as follow-up procedures after the final disposition
Diagnosis
- Based on UA
- Isolated hematuria with dysmorphic red cells or red cells with a decreased mean corpuscular volume (MCV), should prompt an evaluation for glomerulopathy (e.g., IgA nephropathy & Alport's syndrome)[4]
- Isolated hematuria may be elusive. In some series, more than half of the patients have microhematuria with no definable cause.[5]
Management
- Treat underlying cause
- Gross hematuria
- Often associated with intravesicular clot formation and bladder outlet obstruction
- Use triple-lumen urinary drainage catheter with intermittent or continuous bladder irrigation
- Adequate urinary drainage must be ensured; otherwise consult urology
- Use triple-lumen urinary drainage catheter with intermittent or continuous bladder irrigation
- Often associated with intravesicular clot formation and bladder outlet obstruction
Disposition
Outpaient
- Outpatient management appropriate if:
- Hemodynamically stable without life-threatening cause of hematuria
- Able to tolerate oral fluids, antibiotics, and analgesics as indicated
- Able to void
- No significant anemia or acute renal insufficiency
Referral Considerations
- Patients <40 yr: refer to primary care provider for repeat UA within 2wk
- Patients >40 yr with risk factor for urologic cancer: refer to urologist within 2wk
- Risk factors:
- Smoking history
- Occupational exposure to chemicals or dyes
- History of gross hematuria
- Previous urologic history
- History of recurrent UTI
- Analgesic abuse
- History of pelvic irradiation
- Cyclophosphamide use
- Pregnancy
- Known malignancy
- Sickle cell disease
- Proteinuria
- Renal insufficiency
- Risk factors:
- Consider nephrology referral for signs of glomerular hematuria such as concommittant AKI, proteinuria, dysmorphic RBCs, RBC casts
Admission
If:
- Intractable pain
- Intolerance of oral fluids and medications
- Bladder outlet obstruction
- Suspected or newly diagnosed glomerulonephritis
- High risk of developing complications (pulmonary edema, volume overload, hypertensive emergency)
- Pregnant women (hematuria can accompany preeclampsia, pyelonephritis or obstructing nephrolithiasis)
See Also
References
- ↑ Mee S. et al. Radiographic assessment of renal trauma: A 10-year prospective study of patient selection. J Urology. 1989 May;141(5):1095-8
- ↑ Saleem MO, Hamawy K. Hematuria. [Updated 2022 Aug 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK534213/
- ↑ Sharp VJ, Barnes KT, Erickson BA. Assessment of asymptomatic microscopic hematuria in adults. Am Fam Physician. 2013 Dec 1;88(11):747-54. PMID: 24364522.
- ↑ Ingelfinger, J. (2021). Hematuria in Adults. The New England Journal of Medicine, 385(2), 153–161.
- ↑ Ingelfinger, J. (2021). Hematuria in Adults. The New England Journal of Medicine, 385(2), 153–161