Herpes simplex keratitis
Background
- Most common cause of corneal blindness in US
- Avoid topical steroids to prevent necrotizing stromal keratitis
Conjunctivitis Types
Clinical Features
- Blurred vision
- Eye pain, photophobia
- More pain than with typical conjunctivitis
- Tearing
- Perilimbic injection
- Normal pupil size and intraocular pressure
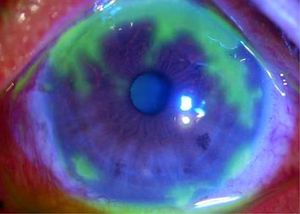
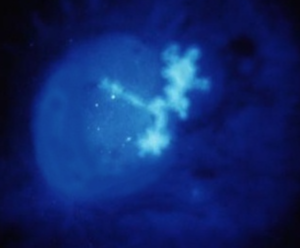
- Dendritic ulcers with fluorescein
- May also see "geographic ulcers" - amoeba-like ulceration with dendrites at the edges[1]
- Severe cases may cause uveitis, iritis
Slit lamp/Fluorescein
- Epithelial disease
- Infectious epithelial keratitis
- Corneal vesicles rarely seen; dendritic ulcers form from coalesced corneal vesicles
- Enlarge into geographic ulcers, with scalloped borders
- Neurotrophic keratopathy
- Ulcers more oval, with smooth borders as opposed to geographic ulcers
- Irregular corneal surface from immune response
- Decreased corneal sensitivity due to scarring, necrosis
- Infectious epithelial keratitis
- Stromal keratitis - develops secondarily to in 25% of patients with epithelial disease
- Necrotizing stromal keratitis - leads to thinning and perforation
- Immune stromal keratitis - recurrent ocular HSV
- Endotheliitis (disease extending from epithelium to stroma to endothelium)
- Keratic precipitates
- Accompanying iritis
Differential Diagnosis
- Iritis
- Conjunctivitis
- Glaucoma
- UV keratitis
- Herpes zoster
- Contact lens complication
- Fungal keratitis
- Bacterial keratitis
- Interstitial keratitis
Herpes Simplex Virus-1
- Eczema herpeticum
- Herpes gingivostomatitis
- Herpes keratitis
- Herpes labialis (cold sore)
- Herpes simplex encephalitis
- Herpetic whitlow
Evaluation
Clinical diagnosis with staining and slit lamp exam
Management
- Topical options
- Acyclovir 3% ophthalmic ointment 5x daily
- Continued for three days after clearing of corneal lesions
- If unavailable, Ganciclovir ophthalmic gel 0.15% 5x daily
- Cycloplegic for symptoms - Cyclopentolate 1% x1 drop 3x daily, lasts for a day
- Acyclovir 3% ophthalmic ointment 5x daily
- Oral acyclovir (400mg 5x daily) or valacyclovir (500mg 3x daily) may be used alone or in combo with topical
- Treatment can be stopped one week after healing of the lesions
- Avoid topical steroids unless in consult with ophtho (steroids can be started when infectious treatment adequately underway)
Disposition
- Usually self-limiting with most experiencing resolution within 3 wks
- Outpatient consult to ophtho for refractory cases, ulcers needing debridement, and multiple recurrences
See Also
External Links
References
- ↑ Go S. Eye Emergencies. In: Cydulka RK, Fitch MT, Joing SA, Wang VJ, Cline DM, Ma O. eds. Tintinalli's Emergency Medicine Manual, 8e. McGraw-Hill; Accessed March 12, 2021. https://accessemergencymedicine.mhmedical.com/content.aspx?bookid=2158§ionid=162273694
- Wang, J et al. Herpes Simplex Keratitis. Dec 7 2015. http://emedicine.medscape.com/article/1194268-overview#showall