Iatrogenic pneumothorax
Background
Causes[1]
- Transthoracic needle aspiration (24%)
- Subclavian vessel puncture (22%)
- Thoracentesis (22%)
- Pleural biopsy (8%)
- Mechanical ventilation (7%)
Clinical Features
Consider in all patients with sudden deterioration after intubation
- Sudden onset pleuritic chest pain
- Tachypnea, hypoxemia, increased work of breathing
- Reduced ipsilateral lung excursion
- Hypotension→ tension pneumothorax
Differential Diagnosis
Pneumothorax Types
Evaluation
Clinically Stable
Defined as having all of the following:
- Resp rate < 24
- Heart rate 60-120 beats per minute
- Normal BP
- SaO2 >90% on room air and patient can speak in whole sentences
Workup
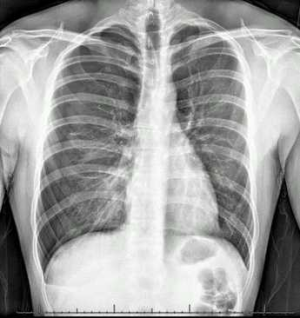
- CXR
- Displaced visceral pleural line without lung markings between pleural line and chest wall
- Upright is best
- Expiratory films DO NOT improve accuracy[2]
- Lateral decubitus films with suspected side up do increase sensitivity. Good approach in pediatrics to avoid CT
- Supine CXR = deep sulcus sign
- CT Chest
- Very sensitive and specific
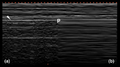
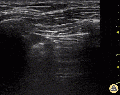
Lung ultrasound of pneumothorax
- No lung sliding seen (not specific for pneumothorax)
- May also identify "lung point": distinct point where you no longer see lung sliding (pathognomonic)
- Absence of lung sliding WITHOUT lung point could represent apnea or right mainstem intubation
- Evaluate other intercostal spaces because pneumothorax may only be seen in least dependent area of thorax
- NO comet tail artifact
- Bar Code appearance/"Stratosphere" sign on M-mode (absence of "seashore" waves)
- Ultrasound has greater sensitivity than chest x-ray for pneumothorax in trauma patients [3]
Management
Supplemental oxygen (non-rebreather mask) initially for all
Unstable
- Needle decompression followed by chest tube insertion
Stable[1]
Not on Positive Pressure
- Observation (majority) vs. aspiration
- Chest tube if become symptomatic
On Positive Pressure Ventilation
- Needle decompression followed by chest tube insertion
Needle Aspiration of Pneumothorax
- Use thoracentesis or "pig-tail" kit, if available
- Place in 2nd IC space in midclavicular line or 4th/5th IC space in anterior axillary line
- Withdraw air with syringe until no more can be aspirated
- Assume a persistent air leak (failure) if no resistance after 4 liters of air has been aspirated AND the lung has not expanded
- Once no further air can be aspirated:
- Option 1
- Place closed stopcock and secure catheter to the chest wall
- Obtain CXR four hours later
- If adequate lung expansion has occurred, remove catheter
- Following another two hours of observation, obtain another CXR
- If the lung remains expanded, may discharge patient
- Option 2
- Leave catheter in place
- Attached a Heimlich (one-way) valve
- May discharge with follow-up within two days
- Option 1
- If 2.5 L of air has been aspirated, and a significant PTX remains, tube thoracostomy is indicated
- NEJM video on needle aspiration of pneumothorax.
Adult Chest Tube Sizes
| Chest Tube Size | Type of Patient | Underlying Causes |
| Small (8-14 Fr) |
|
|
| Medium (20-28 Fr) |
|
|
| Large (36-40 Fr) |
|
Disposition
- See Management section
See Also
External Links
References
- ↑ 1.0 1.1 "Management of spontaneous pneumothorax: British Thoracic Society pleural disease guideline 2010." Thorax 2010;65:ii18-ii31 doi:10.1136/thx.2010.136986 PDF
- ↑ Eur Respir J. 1996 Mar;9(3):406-9
- ↑ Nagarsheth K, Kurek S. Ultrasound detection of pneumothorax compared with chest X-ray and computed tomography scan. Am Surg. 2011 Apr;77(4):480-4. PMID: 21679560.
- ↑ Inaba Et. al J Trauma Acute Care Surg. 2012 Feb;72(2):422-7.
- ↑ Advanced Trauma Life Support® Update 2019: Management and Applications for Adults and Special Populations.