Immune thrombocytopenic purpura (peds)
This page is for pediatric patients. For adult patients, see: Immune thrombocytopenic purpura and ITP in Pregnancy
Background
- Also known as immune thrombocytopenia (ITP), an acquired immune-mediated thrombocytopenia
- Hallmark is isolated thrombocytopenia
- Pathophysiology: Autoantibodies to platelet membrane antigens (ex. GpIIb//IIIa) lead to splenic clearance of platelets and limit production
- Can be primary or secondary (medications, systemic illness, infection, autoimmune disorder)
- Primary peak is in early childhood (2-5 years) with a smaller peak in adolescence
- ITP is a diagnosis of exclusion; first consider all serious causes of petechiae/purpura including meningococcemia, DIC, HUS, TTP, Leukemia, etc
Acute vs Chronic ITP
| Charateristic | Acute ITP | Chronic ITP |
| Common age group | Younger children | Adults |
| Sex | Affects men/women equally | Usually women |
| Duration | Resolves in 1-2 months | Lasts > 3 months |
| Cause | Typically follows viral illness | More likely to have an underlying disease or autoimmune disorder (e.g. SLE) |
| Prognosis | Rarely remits spontaneously or with treatment |
Clinical Features
- Usually well-appearing without constitutional symptoms
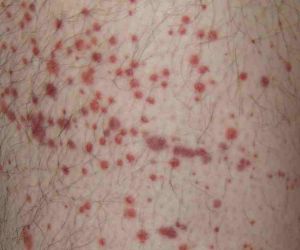
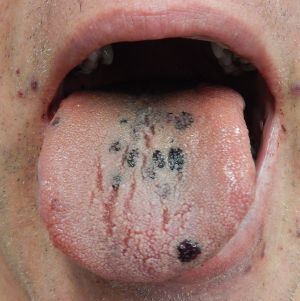
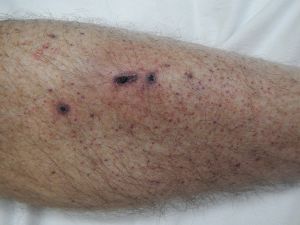
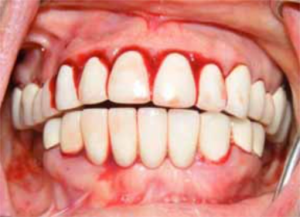
- Isolated petechial rash or bruising is often the first clinical feature
- May have a preceding systemic illness
- >70% of pediatric cases occur after viral infections[1]
- May have exposure to recent vaccinations (particularly MMR) or drugs known to cause thrombocytopenia: Heparin, Quinidine, Phenytoin, Sulfa drugs, Valproate and Vancomycin
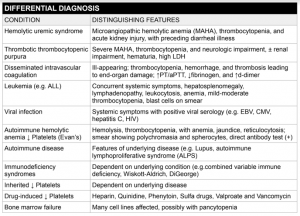
Differential Diagnosis
Thrombocytopenia
Decreased production
- Marrow infiltration (tumor or infection)
- Viral infections (rubella, HIV)
- Marrow suppression (commonly chemotherapy or radiation)
- Congenital thrombocytopenia
- Fanconi anemia
- Alport syndrome
- Bernand Soulier
- Vitamin B12 and/or folate deficiency
Increased platelet destruction or use
- Idiopathic thrombocytopenic purpura
- Thrombotic Thrombocytopenic Purpura (TTP)
- Hemolytic Uremic Syndrome (HUS)
- Disseminated Intravascular Coagulation (DIC)
- Viral infections (HIV, mumps, varicella, EBV)
- Drugs (heparin, protamine)
- Postransfusion or Posttransplantation
- Autoimmune destruction (SLE or Sarcoidosis)
- Mechanical destruction
- Artificial valves
- ECMO
- HELLP syndrome
- Excessive hemorrhage
- Hemodialysis, extracorporeal circulation
- Splenic Sequestration
- Occurs in Sickle cell disease and Cirrhosis
Drug Induced
- sulfa antibiotics, ETOH, ASA, thiazide diuretics/furosemide
Comparison by Etiology
| ITP | TTP | HUS | HIT | DIC | |
|---|---|---|---|---|---|
| ↓ PLT | Yes | Yes | Yes | Yes | Yes |
| ↑PT/INR | No | No | No | +/- | Yes |
| MAHA | No | Yes | Yes | No | Yes |
| ↓ Fibrinogen | No | No | No | No | Yes |
| Ok to give PLT | Yes | No | No | No | Yes |
Evaluation
Workup
- CBC
- Peripheral blood smear to assess for atypical cell lines, hemolytic anemia, and platelet quantity/quality
- Coags if heavy bleeding
- Results are typically normal in ITP
- Type and Screen
- Blood typing can determine Rh status; only Rh+ patients should be treated with RhoGAM
- RhoGAM coats RBCs to later bind Fc gamma receptor in the reticuloendothelial system (spleen), which interferes with the removal of antibody-coated platelets
- There is no role for antiplatelet antibody testing due to lack of sensitivity/specificiy[2]
Diagnosis
- Platelet count of < 100,000/microL is usually the only finding on a CBC
- Consider alternate diagnoses, including leukemia/lymphoma, when other cell lines are abnormal
- Usually < 30,000/microL.
- Remainder of the CBC is typically normal, unless there is significant bleeding (Hgb could be low)
- Peripheral blood smear shows fewer than normal platelets and increased mean platelet volume (due to younger, larger platelets/megakaryocytes)
- Leukocytes and RBCs should be morphologically normal
Management
- Consult pediatric hematologist
- Avoid activity that could increase risk of trauma, especially head trauma
- Avoid NSAIDs and anticoagulants
- Therapy is based on degree of bleeding; first-line therapy includes different combinations of corticosteroids and IVIG or RhoGAM (use only for Rh+ patients)
- Most children (85%) have a self-resolving course and do not require treatment.[3]
- Low-risk bleeding: Watchful waiting
- Moderate to high-risk bleeding: IVIG or RhoGAM if significant bleeding or if preparing for procedure
- Severe bleeding, non-life threatening: Platelet transfusion if needed. Methylprednisolone, IVIG and/or RhoGAM for up to 4 days. Possibly Romiplostim (thrombopoietin receptor agonist) or TXA.
- Life threatening bleeding: Platelet transfusion, methylprednisolone x 3-4 days, IVIG x 1-3 days.
Disposition
- Low-risk patients may be discharged with short-term follow up
- Moderate to high-risk patients or those with severe bleeding should be admitted
See Also
- ITP (adult)
- ITP in Pregnancy
- TTP
References
- Duncan, Ellen. Immune Thrombocytopenia. PEM GUIDES. 7th edition. NYU Langone Health; 2020: 459-462.
- ↑ Deepak M. Kamat; Immune Thrombocytopenia Purpura. Quick References 2020; 10.1542/aap.ppcqr.396184
- ↑ Provan D, Stasi R, Newland AC, Blanchette VS, Bolton-Maggs P, Bussel JB, Chong BH, Cines DB, Gernsheimer TB, Godeau B, Grainger J, Greer I, Hunt BJ, Imbach PA, Lyons G, McMillan R, Rodeghiero F, Sanz MA, Tarantino M, Watson S, Young J, Kuter DJ. International consensus report on the investigation and management of primary immune thrombocytopenia. Blood. 2010 Jan 14;115(2):168-86. doi: 10.1182/blood-2009-06-225565. Epub 2009 Oct 21. PMID: 19846889.
- ↑ Justiz Vaillant AA, Gupta N. ITP-Immune Thrombocytopenic Purpura. [Updated 2023 May 6]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-.