Laryngomalacia
Background
- Common cause of inspiratory stridor in infants and children
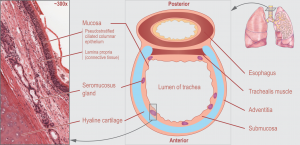
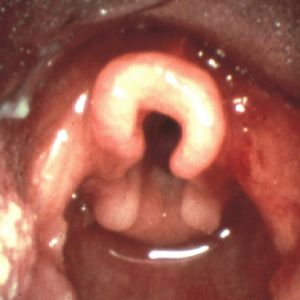
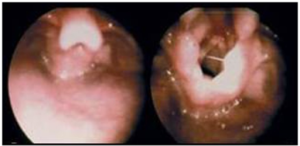
- Characterized by collapse of supraglottic tissue during inspiration
- Differs from tracheomalacia in that this pathology involves soft tissue rather than tracheal cartilage
- Etiology not well-known, possible mechanisms include redundant neck tissue, neurologic causes
- Typically presents as early as 2 years of life, resolves by 2 years of age[1]
Clinical Features
- Inspiratory stridor (peds), especially during sleep
- Snoring
- Dysphagia
- Gastroesophageal reflux disease
Differential Diagnosis
Pediatric stridor
<6 Months Old
- Laryngotracheomalacia
- Accounts for 60%
- Usually exacerbated by viral URI
- Diagnosed with flexible fiberoptic laryngoscopy
- Vocal cord paralysis
- Stridor associated with feeding problems, hoarse voice, weak and/or changing cry
- May have cyanosis or apnea if bilateral (less common)
- Subglottic stenosis
- Congenital vs secondary to prolonged intubation in premies
- Airway hemangioma
- Usually regresses by age 5
- Associated with skin hemangiomas in beard distribution
- Vascular ring/sling
>6 Months Old
- Croup
- viral laryngotracheobronchitis
- 6 mo - 3 yr, peaks at 2 yrs
- Most severe on 3rd-4th day of illness
- Steeple sign not reliable- diagnose clinically
- Epiglottitis
- H flu type B
- Have higher suspicion in unvaccinated children
- Rapid onset sore throat, fever, drooling
- Difficult airway- call anesthesia/ ENT early
- H flu type B
- Bacterial tracheitis
- Rare but causes life-threatening obstruction
- Symptoms of croup + toxic-appearing = bacterial tracheitis
- Foreign body (sudden onset)
- Marked variation in quality or pattern of stridor
- Retropharyngeal abscess
- Fever, neck pain, dysphagia, muffled voice, drooling, neck stiffness/torticollis/extension
Evaluation
Diagnosis
- Confirmed with fiberoptic laryngoscopy by pediatric ENT
- Should also evaluate for other associated anomalies (e.g., esophageal atresia)
Management
- Mild (mild stridor with no other symptoms):
- Frequent monitoring with PCP to ensure adequate weight gain
- Moderate/severe:
- Referral to ENT
Disposition
See Also
External Links
References
- ↑ Shah UK, Wetmore RF. Laryngomalacia: a proposed classification form. Int J Pediatr Otorhinolaryngol. 1998 Nov 15;46(1-2):21-6. doi: 10.1016/s0165-5876(98)00111-6. PMID: 10190701.