Lightning injuries
(Redirected from Lightning)
Background
- Second most common storm-related injury
- Approximately 30 million ground strikes per year
Injury Mechanisms[1]
- Direct effect of electrical current on body
- Electrical to thermal conversion of energy causing superficial and deep burns
- Direct strike = patient is hit directly by lightning current
- Often fatal and may cause penetrating injuries[2]
- Splash Injury = current "splashes" to the patient from another object which is struck first
- Conduction = patient is in contact with an object (e.g. metal fence, tree) that is struck by lightning
- Ground current = Also known as step voltage. Occurs when the current spreads out from the initial strike point and then travels through the patient's body
- Most common mechanism of injury
- Blunt Trauma = Secondary injury pattern that results when the lightning causes a wave of force to propagate through the air to the patient or as a secondary object strikes the patient.
Prehospital Care
- Reverse triage = in lightning-related MCI cases, care should be delivered to patients in cardiac and respiratory arrest first
- Patients struck by lightning who are alive on EMS arrival will likely survive[1]
- All patients should be transported, preferably to a burn center
- Consider spinal precautions in all patients
Clinical Features
Injuries often involve multiple organ systems[3]
Cardiopulmonary
- Both cardiac and respiratory arrest may be present without evidence of external injury
- Ventricular dysrhythmias, asystole, and QT prolongation most common
- Although cardiac automaticity may spontaneously return, apnea may persist
- Duration of apnea rather than cardiac arrest is the critical prognostic factor
- Myocardial infarction after lightning injury is unusual
Neuro
- Symptoms are usually immediate and transient or delayed and permanent
- Seizure, LOC, confusion, amnesia, extremity paralysis
- Pupillary dilation or anisocoria may occur that is unrelated to brain injury
- Neuroprognostication should not be based on dilated pupils alone in setting of lightning strike[4]
- Keraunoparalysis - neuromuscular "stunning" that usually resolves spontaneously within hours
- Thought of as a neurologic phenomenon but actually result of arterial vasospasm from catecholamine release
Vascular
- Vasomotor spasm may cause loss of distal pulses, coolness of extremities, loss of sensation
- Keraunoparalysis - see above
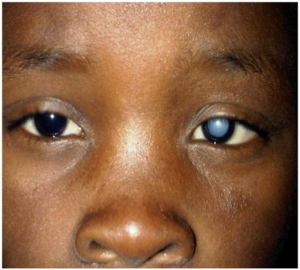
Ocular
- Cataracts may occur weeks to years after injury (must document careful eye exam in all patients)
- Other injuries include vitreous hemorrhage, corneal abrasion, retinal detachment
Auditory
- Blast effect producing Tympanic Membrane Rupture is relatively common
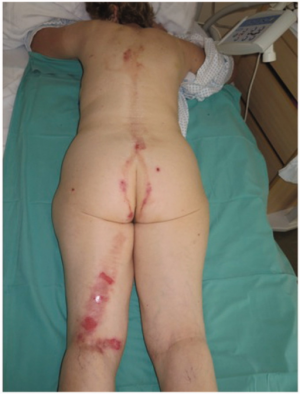
Derm
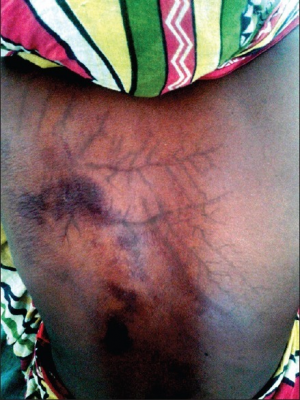
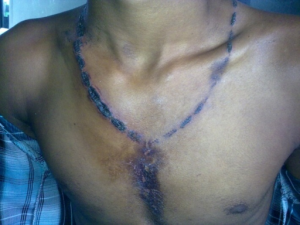
- Lichtenberg figures (ferning pattern) - pathognomonic for lightning strike
- Occur due to electron showering over the skin leading to extravasation of RBC's, not a true burn; disappear within 24hr
- Flash burns
- Similar to those found in arc welders; appear as mild erythema, may involve cornea
- Punctate burns
- Look similar to cigarette burns; are full-thickness
- Contact burns
- Occur when metal close to the skin is heated from the lightning current
Ortho
- Compartment Syndrome and rhabdomyolysis are unlikely due to short duration of lightning current
- Associated with posterior shoulder dislocation
Special Populations
- 50% of pregnancies have fetal demise, though literature is sparse[5]
- Third trimester appears to carry the greatest risk of adverse outcomes
- Most surviving fetuses have no long term morbidity when carried to term
- Any lightning strikes in pregnancy requires fetal monitoring, comprehensive testing in-hospital performed by Ob/Gyn
Differential Diagnosis
Burns
- Smoke inhalation injury (airway compromise)
- Chemical injury
- Acrolein
- Hydrochloric acid
- Tuolene diisocyanate
- Nitrogen dioxide
- Systemic chemical injury
- Specific types of burns
- Associated toxicities
Evaluation
Work-Up
- Exposure: complete and thorough physical exam head to toe
- ECG
- CBC
- Chem
- Total CK
- UA - to evaluate for myoglobinuria
- CT brain (for patients with coma, altered mental status, confusion)
- Other imaging and workup is directed toward visible or suspected injuries
Diagnosis
- Clinical diagnosis
Burn Thickness Chart[6]
| Thickness | Deepest Skin Structure Involved | Pain & Sensation | Appearance | Expected Course | Image |
|---|---|---|---|---|---|
| Superficial (first-degree) |
|
|
|
|
|
| Superficial Partial (second-degree) |
|
|
|
|
|
| Deep Partial (second-degree) |
|
|
|
|
|
| Full (third-degree) |
|
|
|
|
|
| Fourth-degree |
|
|
|
|
Management
- Reverse triage - prolonged on-scene CPR and ACLS protocol is indicated even if there are no initial signs of life
- Aggressive resuscitation
- Lightning-induced Cardiac Arrest has better prognosis than CAD-induced Cardiac Arrest
- Hypotension is not an expected finding (i.e. suggests traumatic blood loss)
- Maintain cervical spine precautions
- Targeted Temperature Management between 32 and 36 degrees Celsius shown to be neuroprotective in setting of hypoxic ischemic encephalopathy after cardiac arrest
Disposition
- Admit patients with persistent muscle pain or neuro, cardiac rhythm, or vascular abnormalities
- Discharged patients require follow up to assess for delayed effects of lightning injury
See Also
References
- ↑ 1.0 1.1 Gatewood M, Zane R. Lightning injuries. Emery Med Clin N Am. 2004; 22: 369-403
- ↑ Waes. O et al. "Thunderstruck": Penetrating Thoracic Injury From Lightning Strike. Annals of Emergency Medicine. 63(4). 2014. 457-458
- ↑ Cooper M. et al. Blumenthal R: Lightning Injuries. Auerbach PS ed: Wilderness Medicine, 6th ed. Philadelphia: Elsevier/Mosby; 2012
- ↑ https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3361158/
- ↑ Galster K et al. Lightning Strike in Pregnancy With Fetal Injury. Wilderness and Environmental Medicine. June 2016. Volume 27, Issue 2, Pages 287–290.
- ↑ Haines E, et al. Optimizing emergency management to reduce morbidity and mortality in pediatric burn patients. Pediatric Emergency Medicine Practice. 12(5):1-23. EB Medicine.