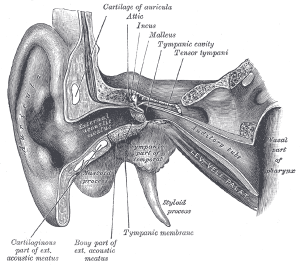
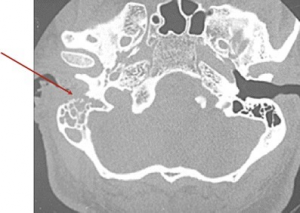
Malignant otitis externa
Background
- Life-threatening infection of external ear/canal, soft tissue, +/- spread to skull base
- Diabetes and immunosuppression are main risk factors
- Pseudomonas causes >90% of cases
- Begins as simple otitis externa
Clinical Features
Adults
- Otitis externa that has not resolved despite 2-3wks of topical antibiotics
- Otalgia often out of proportion for routine otitis externa
- Edema of external auditory canal
- Granulation tissue often seen in the ear canal floor
- Facial nerve often first CN involved[1]
- CN IX, X, or XI involvement
- Trismus
Pediatrics
- More rapidly progressive than in adults
- Fever, leukocytosis, bacteremia/sepsis
- TM, middle ear, and facial nerve more likely to be affected
Differential Diagnosis
Ear Diagnoses
External
- Auricular hematoma
- Auricular perichondritis
- Cholesteatoma
- Contact dermatitis
- Ear foreign body
- Herpes zoster oticus (Ramsay Hunt syndrome)
- Malignant otitis externa
- Otitis externa
- Otomycosis
- Tympanic membrane rupture
Internal
- Acute otitis media
- Chronic otitis media
- Mastoiditis
Inner/vestibular
Evaluation
- Imaging[2]
- Most authors support CT initially, but CT fails to diagnose early osteomyelitis since 30% bone destruction needed for detection
- MRI more sensitive for intracranial complications
- Labs
- WBC usually normal or slightly elevated
- Left shift uncommon
- Elevated ESR and CRP
- Differentiates from MOE from acute external otitis or malignancy
- However, not required for diagnosis[3]
Management
Adults
Peds
Disposition
- Contact ENT for disposition decision; early infection may be managed as outpatient
Complications
- Lateral or sigmoid sinus thrombosis
- Meningitis
See Also
References
- ↑ Pfaff JA, Moore GP: Otolaryngology, in Marx JA, Hockberger RS, Walls RM, et al (eds): Rosen’s Emergency Medicine: Concepts and Clinical Practice, ed 8. St. Louis, Mosby, Inc., 2014, Ch 72.
- ↑ Nussenbaum B et Al. Malignant Otitis Externa Workup. Medscape, Jul 14 2015. http://emedicine.medscape.com/article/845525-workup#c4
- ↑ Hosmer, K: Ear Disorders, in Tintinalli JE, Stapczynski JS, Ma OJ, Yealy DM, Meckler GD, Cline DM (eds): Emergency Medicine, A Comprehensive Study Guide, ed 8. New York, McGraw-Hill, 2016, Ch 242:p 1581-2.