Otic barotrauma
Background
- Also known as "ear squeeze" - generally seen during scuba diving or air travel
Barotrauma Types
- Otic barotrauma
- Pulmonary barotrauma
- Sinus barotrauma
- Mask squeeze
- Barodentalgia (trapped dental air causing squeeze)
Diving Physiology
- Pascals Law applies to the diving body (without air filled areas such as lungs) states that the pressure applied to any part of the enclosed liquid will be transmitted equally in all directions through the liquid.
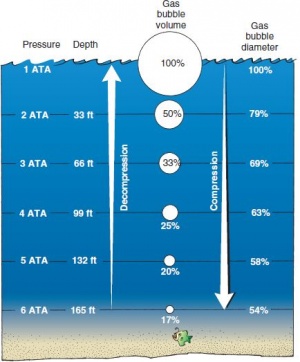
- Boyles Law applies to the diving body's air filled areas such as lungs, sinuses, middle ear, and states that the volume and pressure of a gas at a given temperature are inversely related.
- At 2 ATA (10m/33ft) a given gas would be 1/2 it's volume, at 3 ATA (20m/66ft) it would be 1/3 it's volume and so on.
- Dalton's Law applies to the total pressure of an ideal gas mixture being the sum of the partial pressures of each individual gas.
- Divers may used Enriched Air NITROX mixtures to proportionally increase partial pressures of oxygen and reduce partial pressures of nitrogen while diving.
- At extremes of depth, additional inert gasses such as helium in TRIMIX are used to further reduce partial pressures of both oxygen and nitrogen below toxic levels.
- Henry's Law applies to the dissolvability of gasses into fluids, including body tissues, being proportional to the partial pressure of the gas.
- The increased pressure at depth causes divers to breath their gas mix at increased pressure to defeat the external water pressure.
- Increased inhaled partial pressures of nitrogen increase risk of nitrogen narcosis, and dissolved nitrogen in tissues re-expanding in micro-bubbles on ascent is the essential cause of decompression sickness. This can affect divers at any depth, including commonly-seen recreational diving depths of 20m/60ft or less.
- Increased inhaled partial pressures of oxygen, generally beyond 1.4-1.6atm, increases risk of oxygen toxicity. This is typically not a substantial risk in common depths of recreational divers at 20m/60ft of depth or less, but can be for more advanced divers at deeper depths.
- The increased pressure at depth causes divers to breath their gas mix at increased pressure to defeat the external water pressure.
Clinical Features
Middle Ear
- Results from inability to equalize middle ear pressure
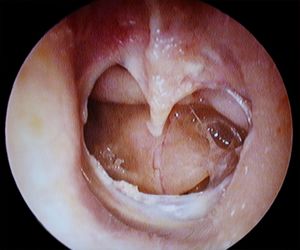
- Pain, fullness, vertigo, conductive hearing loss, TM rupture
Inner Ear
- Results from forceful valsalva against an occluded eustachian tube, or rapid descent in diving or aviation
- Pressure difference between middle ear and inner ear can rupture oval or round window
- Sudden onset of sensorineural hearing loss, tinnitus, severe vertigo
- Must be lacking in any other neurologic signs (otherwise consider infarction)
Differential Diagnosis
Diving Emergencies
- Barotrauma of descent
- Otic barotrauma
- Pulmonary barotrauma
- Sinus barotrauma
- Mask squeeze
- Barodentalgia (trapped dental air causing squeeze)
- Barotrauma of ascent
- Pulmonary barotrauma (pulmonary overpressurization syndrome)
- Decompression sickness (DCS)
- Arterial gas embolism
- Alternobaric vertigo
- Facial baroparesis (Bells Palsy)
- At depth injuries
- Oxygen toxicity
- Nitrogen narcosis
- Hypothermia
- Contaminated gas mixture (e.g. CO toxicity)
- Caustic cocktail from rebreathing circuit
Ear Diagnoses
External
- Auricular hematoma
- Auricular perichondritis
- Cholesteatoma
- Contact dermatitis
- Ear foreign body
- Herpes zoster oticus (Ramsay Hunt syndrome)
- Malignant otitis externa
- Otitis externa
- Otomycosis
- Tympanic membrane rupture
Internal
- Acute otitis media
- Chronic otitis media
- Mastoiditis
Inner/vestibular
Barotrauma Types
- Otic barotrauma
- Pulmonary barotrauma
- Sinus barotrauma
- Mask squeeze
- Barodentalgia (trapped dental air causing squeeze)
Evaluation
- Generally clinical
- Webber and Rinne for middle ear barotrauma
- Conductive hearing loss expected
- TEED grading system for middle ear barotrauma
| Grade | Description |
|---|---|
| 0 | Symptoms without otologic findings |
| 1 | Erythema and mild retraction of the tympanic membrane |
| 2 | Erythema of the tympanic membrane with mild or spotty hemorrhage within the membrane |
| 3 | Gross hemorrhage throughout the tympanic membrane |
| 4 | Grade 3 changes pluse hemorrhage within the middle ear (hemotympanum) |
| 5 | Free blood in the middle ear plus perforation of the tympanic membrane |
Management
Middle Ear
- Decongestants and topical nasal vasoconstrictors
- Consider antibiotics if tympanic membrane rupture
- Remember to use medications such as ofloxacin suspension that will be safe in the middle ear
- Urgent audiology required if sensorineural hearing loss, rather than conductive hearing loss
Inner Ear
- Elevate head of bed
- Advise patient to not blow nose
- Antivertigo medications (e.g. meclizine)
- ENT consult
Disposition
- Generally may be discharged with ENT follow up
- Resolution usually in 5-7 days, but can take up to 2 weeks