Ovarian torsion
(Redirected from Ovarian Torsion)
Background
- Rotation of the ovary around its vascular pedicle (infundibulopelvic and utero-ovarian ligaments)
- Compromises venous/lymphatic drainage first → edema → eventual arterial compromise → ischemia and necrosis
- 5th most common gynecologic emergency
- Accounts for ~3% of all gynecologic emergencies
- Most common in reproductive-age women (20-40 years)
- Risk factors:
- Ovarian mass >5 cm (most common risk factor; dermoid cysts particularly prone)
- Ovarian hyperstimulation syndrome (fertility treatment)
- Pregnancy (especially first trimester; corpus luteum cysts)
- Prior tubal ligation (increases ovarian mobility)
- Long utero-ovarian ligament
- Right side more common than left (sigmoid colon may limit left ovarian mobility)
- Can occur in prepubertal girls (often without predisposing mass — normal ovary)
Clinical Features
- Sudden onset, severe, unilateral lower abdominal/pelvic pain (most common presentation)
- Pain may be intermittent (intermittent torsion/detorsion)
- Nausea and vomiting (present in 70% — may be prominent)
- Low-grade fever (late finding suggesting necrosis)
- Adnexal tenderness on bimanual exam; palpable adnexal mass in ~50%
- May mimic appendicitis, renal colic, or ectopic pregnancy
- Peritoneal signs are late and suggest necrosis
- In children: may present with non-specific abdominal pain
Differential Diagnosis
- Ectopic pregnancy (always obtain pregnancy test first)
- Ruptured ovarian cyst
- Appendicitis
- Renal colic / nephrolithiasis
- Pelvic inflammatory disease / tubo-ovarian abscess
- Endometriosis
- Testicular torsion (analogous condition)
- Hemorrhagic corpus luteum
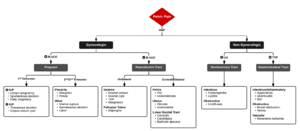
Acute Pelvic Pain
Gynecologic/Obstetric
- Normal variants may be noted on exam but generally do not cause pain or other symptoms
- Nabothian cysts: Epithelial cells within mucous glans that appear as yellow inclusions on the cervix
- Cervical Ectropion: Edothelial cells on the exterior of the cervix
- Parous cervix: The is no longer round but may have multiple shapes after birth
- Pregnancy-related
- Ectopic pregnancy
- Spontaneous abortion, threatened or incomplete
- Septic abortion
- Pelvic organ prolapse
- Acute Infections
- Vulvovaginitis
- Adnexal Disorders
- Hemorrhage/rupture of ovarian cyst
- Ovarian torsion
- Twisted paraovarian cyst
- Other
- Myoma (degenerating)
- Genitourinary trauma
- Ovarian hyperstimulation syndrome
- Sexual assault
- Recurrent
- Mittelschmerz
- Primary/Secondary Dysmenorrhea
- Pelvic Congestion Syndrome
- Endometriosis
Genitourinary
Gastrointestinal
- Gastroenteritis
- Appendicitis
- Bowel obstruction
- Perirectal abscess
- Diverticulitis
- Inflammatory bowel disease
- Irritable bowel syndrome
- Mesenteric adenitis
Musculoskeletal
- Abdominal wall hematoma
- Psoas hematoma, psoas abscess
- Hernia
Vascular
- Pelvic thrombophlebitis
- Abdominal aortic aneurysm
- Ischemic bowel (Mesenteric Ischemia)
Evaluation
- Urine pregnancy test (rule out ectopic pregnancy)
- CBC: leukocytosis may be present (nonspecific)
- Urinalysis: rule out UTI, nephrolithiasis
- Lactate: may be elevated in late presentations
Transvaginal Ultrasound (Test of Choice)
- Enlarged ovary (>4 cm) compared to contralateral side
- Ovarian edema (heterogeneous appearance)
- Peripherally displaced follicles ("string of pearls" sign)
- Whirlpool sign on Doppler: twisted vascular pedicle (most specific finding)
- Free fluid in cul-de-sac
Doppler Findings
- Absent or decreased ovarian arterial/venous flow supports diagnosis
- HOWEVER: presence of Doppler flow does NOT exclude torsion[2]
- Sensitivity of absent flow is only ~50% — dual blood supply (ovarian and uterine arteries)
- Intermittent torsion may show normal flow between episodes
- If high clinical suspicion, proceed to OR despite normal Doppler
CT Abdomen/Pelvis
- May show enlarged ovary, fat stranding, deviation of uterus toward affected side
- Less sensitive than US for torsion but may identify alternative diagnoses
- "Ovarian mass with surrounding fat stranding" on CT should raise concern
Management
- Emergent gynecology consultation for operative intervention
- Time-sensitive — ovarian salvage rates decrease with prolonged ischemia
- Detorsion within 6 hours: high salvage rate
- Detorsion at 24-36 hours: viable ovary still possible
- Do not assume a black/dusky ovary is nonviable — most recover after detorsion
- Laparoscopic detorsion is procedure of choice (preserves fertility)
- Oophoropexy (fixation) may be performed to prevent recurrence
- Oophorectomy reserved for clearly necrotic tissue or suspected malignancy
- Supportive care in ED:
- IV fluids, antiemetics (ondansetron 4 mg IV)
- Pain control: ketorolac 15-30 mg IV and/or opioids
- NPO for OR preparation
Disposition
- Admit for emergent surgical intervention
- Do NOT delay surgery for additional imaging if clinical suspicion is high
- Consult gynecology early — even if US is equivocal, operative evaluation may be warranted
See Also
References
- Huchon C, Fauconnier A. Adnexal torsion: a literature review. Eur J Obstet Gynecol Reprod Biol. 2010;150(1):8-12. PMID 20189289
- Chang HC, et al. Pearls and pitfalls in diagnosis of ovarian torsion. Radiographics. 2008;28(5):1355-1368. PMID 18794312
- Houry D, Abbott JT. Ovarian torsion: a fifteen-year review. Ann Emerg Med. 2001;38(2):156-159. PMID 11468611
- Oelsner G, Shashar D. Adnexal torsion. Clin Obstet Gynecol. 2006;49(3):459-463. PMID 16885652