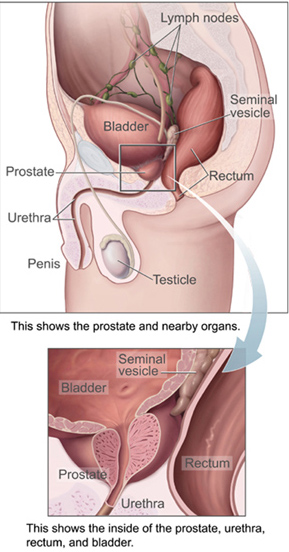
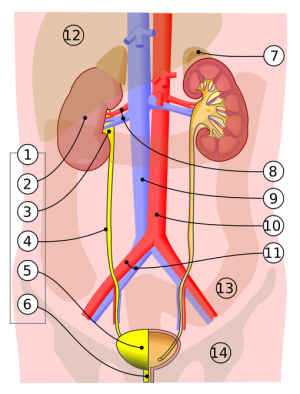
Prostatitis
Background
- E. coli involved in 80% of cases
- Other: Pseudomonas, Klebsiella, Enterobacter, Serratia, Staph
Risk Factors
- Urinary Tract Obstruction
- Epididymitis
- Urethritis
- Unprotected rectal intercourse
- Phimosis
- Indwelling urethral catheter
Genitourinary infection
"UTI" frequently refers specifically to acute cystitis, but may also be used as a general term for all urinary infections; use location-specific diagnosis.
- Renal/perirenal
- Ureteral
- Infected urolithiasis
- Bladder
- Acute cystitis ("UTI")
- Chronic cystitis
- Urethra/periurethra
Clinical Features
Acute
- Dysuria/urgency/frequency, perineal pain/low back pain, pain with ejaculation, fever
- Rectal exam: Exquisitely tender and boggy prostate
Chronic
- Similar to acute prostatitis with exception of fever/chills
- Rectal exam is often unremarkable
Differential Diagnosis
Dysuria
- Genitourinary infection
- Acute cystitis ("UTI")
- Pyelonephritis
- Urethritis
- Chronic cystitis
- Infected nephrolithiasis
- Prostatitis
- Epididymitis
- Renal abscess/perinephric abscess
- Emphysematous pyelonephritis
- Nephrolithiasis
- Urethral issue
- Urethritis
- Urolithiasis
- Urethral foreign body
- Urethral diverticulum
- Allergic reaction (contact dermatitis)
- Chemical irritation
- Urethral stricture or obstruction
- Trauma to vagina, urethra, or bladder
- Gynecologic
- Vaginitis/cervicitis
- PID
- Genital herpes
- Pelvic organ prolapse
- Fistula
- Cystocele
- Other
- Diverticulitis
- Interstitial cystitis
- Behavioral symptom without detectable pathology
Evaluation
Work-Up
- Urinalysis, urine culture
Diagnosis
- Clinical diagnosis (UA and Urine culture may be normal)
Management
Antibiotics
Associated with STD
Target organisms are E. coli, and STDs (GC)
- Doxycycline 100mg PO q12 hrs x14 days + 500mg IM x1
- Ciprofloxacin no longer recommended to treat gonorrhea in US
No Associated STD and Chronic Bacterial Prostatitis
Aimed at Enterobacteriaceae, enterococci, Pseudomonas
- Ciprofloxacin 500mg PO q12hrs x 28 days OR
- Levofloxacin 500mg PO daily x 28 days OR
- TMP/SMX 1 DS tablet PO q12hrs x 28 days
- Consider extension to 6 wks of empiric therapy
Septic
- Gentamicin 7mg/kg IV daily + 1g IV q12hrs
Supportive Measures[1]
- If severe obstruction suspected, may pass a Foley gently
- If Foley does not pass easily, insert punch suprapubic catheter, to be removed 24-36 hrs later
- Consider α-blocker for outflow obstruction and urinary reflux
- Terazosin 5mg/d PO for 4 weeks or long-term
- OR tamsulosin
- Prostatic abscesses frequently require surgical aspiration
Disposition
- Admit toxic patients or patients with Urinary Retention
- Urology follow up
- Should obtain repeat Urinalysis and urine culture in 7 days
- Ensure follow up to tailor therapy to urine culture and sensitivities
- Counsel patients on importance of adhering to full course of prolonged therapy
References
- ↑ Deem SG et al. Acute Bacterial Prostatitis. eMedicine. Dec 9, 2015. http://emedicine.medscape.com/article/2002872-treatment