Endocarditis
(Redirected from Splinter hemorrhage)
Background
- Defined as an infection of the endocardial surface of the heart, affecting native (or prosthetic) heart valves as well as in-dwelling cardiac devices
- Consider in patients with known risk factors and unexplained fever
- Mitral valve most commonly affected overall; tricuspid valve most common in IVDA
- Noninfectious vegetations can arise in patients with malignancy/SLE/Hypercoagulable state ("Marantic" endocarditis)
- S. aureus is single most common cause (accounts for 1/3 of all cases)[1]
- Strep viridans is the most common cause of native valve endocarditis, excluding risk factors below
- Blood cultures are falsely negative ~5% (think HACEK organisms)
- Only 20% have an increase in a known murmur and only 48% have a new murmur[2]
Prophylaxis
- No longer recommended at all in the United Kingdom[3]
- In United States, only recommended for invasive dental procedures (not routine cleanings) and invasive respiratory procedures in setting of: [4][5]
- Prosthetic valves
- Prior endocarditis
- Un-repaired congenital cyanotic heart disease
- Repaired congenital heart disease/valvulopathy with prosthetic material
Risk Factors
- IVDA
- Tricuspid valve most commonly affected
- Prosthetic heart valve
- Coagulase negative staphylcocci are substantial etiologies in this patient population[6]
- Structural heart disease
- Rheumatic heart disease (biggest risk factor in low-income countries)
- Mitral valve prolapse
- Bicuspid aortic valve
- Hemodialysis
- HIV infection
- Fungal endocarditis risk factors, with Candida most common
- Prolonged antibiotics
- TPN through central line
Clinical Features
- Fever
- Present in 80% of cases
- Heart murmur
- Preexisting murmur found in 85% of cases; new murmur found in 48%
- CHF
- Acute or progressive (70%)
- Derm
- Osler nodes
- Tender red/purple nodules on distal finger and toes
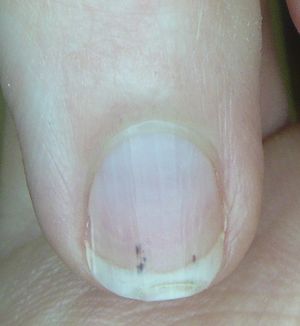
- Splinter hemorrhages
- Nail bed hemorrhages not extending the length of the nail
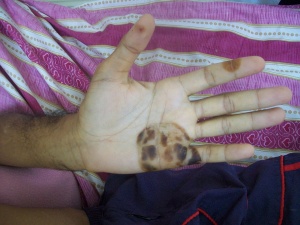
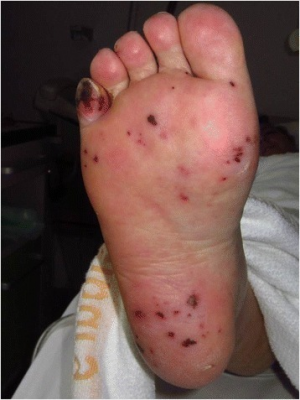
- Janeway lesions
- Non-tender, small erythematous or hemorrhagic macular, papular or nodular lesions on the palms or soles only a few millimeters in diameter
- Osler nodes
- CNS
- 65% of emboli involve the CNS[7]
- Central retinal artery occlusion
- Pulmonary
- Cardiac
- Abdominal
- Bowel, renal, splenic infarcts
- Ophtho
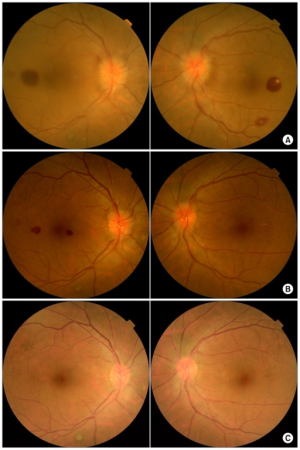
- Roth spots
- White centered retinal hemorrhage
- Associated with multiple systemic illnesses, most commonly bacterial endocarditis
- Roth spots
Differential Diagnosis
<translate>
Fever
Infectious
- Critical
- Sepsis
- PNA with respiratory failure
- Peritonitis
- Meningitis
- Cavernous Sinus Thrombosis
- Necrotizing Fasciitis
- Emergent
- PNA
- Peritonsillar Abscess
- Retropharyngeal Abscess
- Epiglottitis
- Endocarditis
- Pericarditis
- Appendicitis
- Cholecystitis
- Diverticulitis
- Intra-abdominal abscess
- Pyelonephritis
- Tubo-ovarian abscess
- Encephalitis
- Brain abscess
- Cellulitis
- Abscess
- Malaria
- Non-emergent
Non-infectious
- Critical
- Emergent
- CHF
- Dehydration
- Recent Seizure
- Sickle Cell Dz
- Transplant rejection
- Pancreatitis
- DVT
- Serotonin Syndrome
- Non-emergent
- Drug fever (except as in NMS and Serotonin Syndrome)
- Malignancy
- Gout
- Sarcoidosis
- Crohn's Disease
- Postmyocardiotomy syndrome
- Sweet's syndrome
</translate>
- Endocarditis
- Infected DVT
- Lemierre's syndrome
- Central line, pacemaker wire infection
- Peri-odontal disease
Evaluation
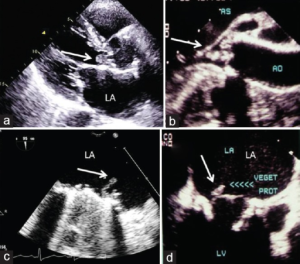
Vegetations in infective endocarditis (arrows). (a) Transthoracic echocardiogram parasternal long-axis view showing vegetation on native aortic valve; (b) transesophageal echocardiography long axis of endocarditis of native aortic valve; (c) transesophageal echocardiography visualization of vegetation on the atrial side of mechanical mitral valve; (d) transesophageal echocardiography showing endocarditis of bioprosthetic mitral valve. LA: Left atrium; LV: Left ventricle.
Work-Up
- Blood culture (from 3 separate sites)[8]
- CBC
- Staphylococcal endocarditis: Leukocytosis +/- thrombocytopenia
- Subacute endocarditis: WBC may be normal or elevated
- Urinalysis
- ESR
- Elevated in >90% of cases
- ECG
- Ischemia, heart block
- CXR
- Pulmonary emboli, CHF
- Ultrasound
- Obtain as soon as possible
- TEE may be required for:
- Prosthetic valves
- Difficulty obtaining clear TTE images (obesity, COPD)
- High clinical probability of endocarditis
Diagnosis
- Inpatient diagnosis is based on the Duke's Criteria although many of the criteria are not filled in the ED
- Heightened clinical suspicion is necessary even if diagnosis does not meet the official criteria.[9]
Modified Duke Criteria[10]
- 2 major criteria OR
- 1 major and 3 minor criteria OR
- 5 minor criteria
Major Criteria
- Positive blood culture with typical IE microorganism, defined as one of the following:
- Typical microorganism consistent with IE from 2 separate blood cultures, as noted below:
- Viridans-group streptococci, or
- Streptococcus bovis including nutritional variant strains, or
- HACEK group, or
- Staphylococcus aureus, or
- Community-acquired Enterococci, in the absence of a primary focus
- Microorganisms consistent with IE from persistently positive blood cultures defined as:
- Two positive cultures of blood samples drawn >12 hours apart, or
- All of 3 or a majority of 4 separate cultures of blood (with first and last sample drawn 1 hour apart)
- Coxiella burnetii detected by one positive blood culture or IgG
- Staphylococus lugdunensis should raise concerns for endocarditis with a single positive blood culture[11]
- Typical microorganism consistent with IE from 2 separate blood cultures, as noted below:
- Evidence of endocardial involvement with positive echocardiogram defined as:
- Valvular mass or supporting structures or
- Abscess, or
- New disruption of a prosthetic valve or new valvular regurgitation
Minor Criteria
- Predisposing factor: known cardiac lesion, recreational drug injection
- Fever >38°C
- Evidence of emboli: arterial emboli,pulmonary infarcts, Janeway lesions, conjunctival hemorrhage
- Glomerulonephritis, Osler's nodes
- Positive blood culture (that does not meet a major criterion) or serologic evidence of infection
Management
- Initial management should focus on early blood cultures and antibiotics
CHF/Cardiogenic Shock
- Often due to valve failure, rupture, or a new defect.
Pulmonary edema
- Often due to mitral or aortic valve rupture causing severe regurgitation
- Focus on after-load reduction
Respiratory failure (emboli)
- Often requires intubation with failure either due to CHF or Pneumonia
- Multi-lobar pneumonia suggests a tricuspid or pulmonary valve lesion with emboli to lungs
Antibiotics
Start after 3 sets of blood cultures are obtained (if possible)[8]
Therapy should be based on:
- Whether the patient has received prior antibiotic therapy
- Prosthetic valves
- Local antibiotic resistance patterns or knowledge of prior endocarditis cultures
- Prior hospitalizations and risk of MRSA
Native Valves
Options:[12]
- Ampicillin/Sulbactam 12g/day IV in 4 doses + Gentamicin 3mg/kg/day IV in 2 or 3 doses
- Amoxicillin/Clavulanate 12g/day in 4 doses + Gentamicin 3mg/kg/day IV in 2 or 3 doses
- Oxacillin 2g IV six times daily or Nafcillin 2g IV six times daily + Gentamicin 1mg/kg IV three times daily AND Ampicillin 2g IV six times daily
- Daptomycin 6mg/kg IV once daily
Suspected MRSA:[12]
- Vancomycin 30mg/kg/day IV in 2 doses PLUS
- Gentamicin 3mg/kg/day IV in 2 or 3 doses PLUS
- Ciprofloxacin 1000mg/day PO in 2 doses or 800 mg/day IV in 2 doses
Prosthetic Valves (Early)
- Early prosthetic valve endocarditis defined as < 12 months post surgery[12]
- Vancomycin 30mg/kg/day IV in 2 doses PLUS
- Gentamicin 3mg/kg/day IV in 2 or 3 doses PLUS
- Rifampin 1200 mg/day PO in 2 doses
IV Drug User without Prosthetic Valve
- Vancomycin 15-20 mg/kg IV BID daily
- Daptomycin 6mg/kg IV once daily
Prosthetic Valve (Late)
- Late prosthetic valve endocarditis defined as ≥ 12 months post surgery[12]
- Same as native valve endocarditis empiric therapy
Dental Procedure Prophylaxis
All antibiotics options are given as a single dose 1 hour prior to the dental procedure
Options:[13]
- Amoxicillin 2g or 50mg/kg
- Ampicillin 2g (50mg/kg) IV or IM
- Cefazolin 1g (50mg/kg) IM or IV or Ceftriaxone 1g (50mg/kg) IM or IV
- Clindamycin 600mg (20mg/kg) PO or IV
- Azithromycin 500mg (15mg/kg) PO or Clarithromycin 500mg (15mg/kg) PO
Pediatric Dosing:
- Amoxicillin 50mg/kg PO (max 2g) 1hr before procedure
- Ampicillin 50mg/kg IV/IM (max 2g) 30min before procedure if unable to take PO
- PCN allergy: Clindamycin 20mg/kg PO or IV (max 600mg) OR
- Azithromycin 15mg/kg PO (max 500mg) OR
- Cephalexin 50mg/kg PO (max 2g)
Pediatric Empiric
- Vancomycin 15mg/kg IV q6hrs (max 2g/dose) + Gentamicin 1mg/kg IV q8hrs
- Nafcillin 50mg/kg IV q6hrs (max 2g/dose) if MSSA confirmed
- Ceftriaxone 100mg/kg/day IV divided q12h (max 4g/day) as alternative
Disposition
Admit all suspected cases and consult Cardiothoracic surgery for endocarditis complicated by:[2]
- New Heart failure suspected due to severe regurgitation
- Cardiogenic Shock
- Echocardiography demonstrating a new fistula
- Surgery indicated for[14]:
- Acute heart failure
- Periannular extension
- Recurrent emboli
- Large mobile vegetations
- Persistent bacteremia
- Fungal endocarditis (penetration of antifungals into vegetation walls poor)[15]
- IV amphotericin B
- Lifelong PO antifungal
Miscellaneous
- No therapeutic anticoagulation necessary
- Anticoagulation carries higher risk of bleeding without delivering mortality benefit or reducing embolic complication[16]
- Septic pulmonary embolism
- Most common culture growths are MSSA, MRSA, and candida[17]
- Furthermore, therapeutic anticoagulation not indicated for septic pulmonary embolism
Complications
Cardiac
- Heart Failure
- Most common cause of death due to IE
- Perivalvular Abscess
Embolic
- CVA
- Blindness
- Painful, ischemic extremities
- Unusual pain syndromes (due to splenic or renal infarction)
- Mycotic aneurysm
- Hypoxia
- MI
Neurologic
- Embolic stroke
- Acute encephalopathy
- Meningoencephalitis
- Purulent or aseptic meningitis
- Cerebral hemorrhage
- Seizure
- Spinal abscess
Renal
Musculoskeletal
See Also
External Links
References
- ↑ Selton-Suty C, Célard M, Le Moing V, et al. Preeminence of Staphylococcus aureus in infective endocarditis: a 1-year population-based survey. Clin Infect Dis. 2012;54(9):1230-1239. doi:10.1093/cid/cis199
- ↑ 2.0 2.1 Hoen, B. et al. Infective Endocarditis. NEJM. 2013. 368;15. 1425-1433 PDF
- ↑ Wilson W. et al. Prevention of infective endocarditis: guidelines from the American Heart Association: a guideline from the American Heart Association Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee, Council on Cardiovascular Disease in the Young, and the Council on Clinical Cardiology, Council on Cardiovascular Surgery and Anesthesia, and the Quality of Care and Outcomes Research Interdisciplinary Working Group. Circulation 2007;116(15):e376-e377.
- ↑ Richey R, Wray D, Stokes T. Prophylaxis against infective endocarditis: summary of NICE guidance. BMJ 2008;336: 770-1.
- ↑ Wilson W, et al. Prevention of Infective Endocarditis: Guidelines from the American Heart Association. Circulation. 2007;116:1736-1754
- ↑ Lalani T et al. Prosthetic valve endocarditis due to coagulase-negative staphylococci: findings from the International Collaboration on Endocarditis Merged Database. Eur J Clin Microbiol Infect Dis. 2006 Jun;25(6):365-8.
- ↑ Mylonakis. E, Calderwood S. Infective endocardidits in adults. NEJM. 2001;345(18):138-1330
- ↑ 8.0 8.1 Lee A, Mirrett S, Reller LB, Weinstein MP. Detection of bloodstream infections in adults: how many blood cultures are needed? J Clin Microbiol 2007;45: 3546 – 3548
- ↑ Durack D, Lukes A, Bright D "New criteria for diagnosis of infective endocarditis: utilization of specific echocardiographic findings. Duke Endocarditis Service". Am J Med. 1994. 96 (3): 200–9
- ↑ Li, JS et al. "Proposed Modifications to the Duke Criteria for the Diagnosis of Infective Endocarditis". Clinical Infectious Diseases. 2000. 30(4). 633.
- ↑ Liu Po-Yen et al. Staphylococcus lugdunensis Infective Endocarditis: A Literature Review and Analysis of Risk Factors. Journal of Microbiology, Immunology and Infection Volume 43, Issue 6, December 2010, Pages 478-484.
- ↑ 12.0 12.1 12.2 12.3 ESC Task Force Guidelines on the prevention, diagnosis, and treatment of infective endocarditis. European Heart Journal (2009) 30, 2369–2413 doi:10.1093/eurheartj/ehp285 PDF
- ↑ AHA Pocket Card Dental Prophylaxis Endocarditis
- ↑ Kosowsky JM, Takhar SS: Infective Endocarditis and Valvular Heart Disease in Marx JA, Hockberger RS, Walls RM, et al (eds): Rosen’s Emergency Medicine: Concepts and Clinical Practice, ed 8. St. Louis, Mosby, Inc., 2013, (Ch) 84: pp 1113-1123.
- ↑ British Society for Antimicrobial Chemotherapy. Guidelines for the antibiotic treatment of endocarditis in adults: report of the Working Party of the British Society for Antimicrobial Chemotherapy. J. Antimicrob. Chemother. (December 2004) 54 (6): 971-981.
- ↑ Elkaryoni A et al. ANTICOAGULATION IN INFECTIVE ENDOCARDITIS: INSIGHTS FROM NATIONWIDE INPATIENT SAMPLE. Journal of the American College of Cardiology. Volume 73, Issue 9 Supplement 1, March 2019.
- ↑ Li Zhao RY et al. Clinical characteristics of septic pulmonary embolism in adults: A systematic review. Respiratory Medicine. Volume 108, Issue 1, January 2014, Pages 1-8.