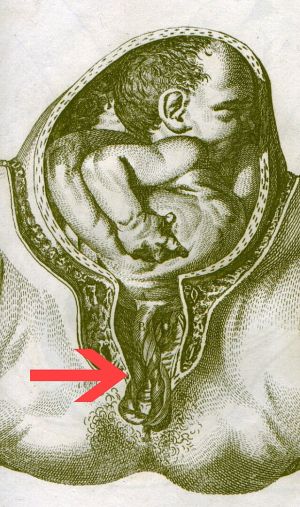
Umbilical cord prolapse
Background
- Occurs in 0.5% of pregnancies
- Likely secondary to the presenting fetal part not filling enough of the lower uterus and allowing cord to present first during labor.[1]
Risk factors
Clinical Features
- Presentation of umbilical cord before fetal delivery (can be felt as pulsatile structure on exam)
Differential Diagnosis
- Emergent delivery
- Umbilical cord prolapse
- Breech delivery
- Shoulder dystocia
- Perimortem cesarean delivery
Evaluation
- Clinical diagnosis
Management
- Emergent OB/Gyn consult
- Do NOT attempt to reduce cord
- Elevate presenting fetal part to reduce compression and transport to OR for emergent C-section[2]
- Examiner who diagnosed umbilical cord prolapse must maintain umbilical decompression until patient is in OR
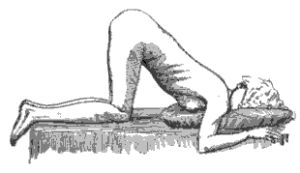
- Place patient in knee-chest position and encourage not to push or cough[1]
- May also consider Trendelenburg position (if patient can tolerate) to let gravity assist in moving fetus off pelvic floor
Disposition
- Admit to L&D