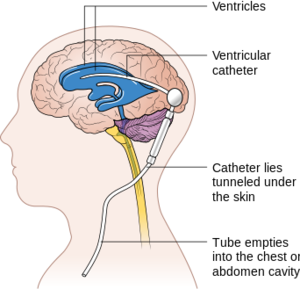
Ventriculoperitoneal shunt complications
(Redirected from VP shunt)
Background
- Also called a cerebral sinus fluid (CSF), VP, or cerebral shunt
- Highest incidence of postoperative complications of any neurosurgical procedure
- Majority in the first 2 years (40% in the first year[1])
- May drain into peritoneal cavity or less commonly the right atrium, pleural cavity, ureter, gallbladder
Clinical Features
- Typically develop over several days
Adults
- Cephalgia, nausea and vomiting, lethargy, ataxia, altered mental status
- Paralysis of upward gaze ("sunset eyes"), dilated pupils, cranial nerve palsies
Infants
- Vomiting, irritability, bulging fontanelle
- Often very subtle: a caregiver-reported change in behavior predicts malfunction
Physical Exam
- Neither sensitive nor specific
- Decreased level of consciousness, erythema along shunt tract, bulging fontanelle, nausea/vomiting, irritability should raise suspicion
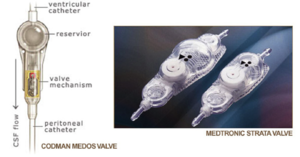
- Valve chamber abnormality
- Gently compress chamber and observe for refill
- Difficulty compressing chamber indicates distal flow obstruction
- Slow refill (>3s) indicates proximal obstruction
Differential Diagnosis
Ventriculoperitoneal shunt problems
- Ventriculoperitoneal shunt obstruction
- Ventriculoperitoneal shunt overdrainage (Slit Ventricle Syndrome)
- Ventriculoperitoneal shunt infection
- Ventriculoperitoneal shunt mechanical failure
Loculation of Ventricles
- Separate, noncommunicating CSF accumulations may develop within a ventricle
- Shunt device unable to drain entire ventricular system leading to increased ICP
Abdominal Complications
- Pseudocyst may form around the peritoneal catheter
- Can lead to occlusion and/or abdominal pain (depending on size)
Evaluation
- CBC, Chem7, coags
- Blood cultures
- Shunt tap if concerned for infection (this is usually done by or in consultation with neurosurgery)
- A normal lumbar puncture does not rule out ventriculitis (shunt infection)
- Imaging
- Shunt series
- AP and lateral skull, AP chest and abdomen
- Identifies kinking, migration, or disconnection
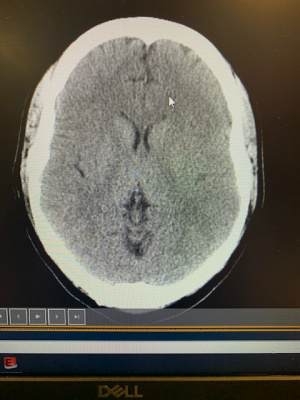
- CT
- Needed to evaluate ventricular size (if larger, concerning for elevated ICP)
- Very helpful to compare to previous study (many patients with shunts have abnormal baseline)
- One-third of patients with shunt malfunction will have normal head CT[citation needed]
- Ultrasound
- If the baby has an open fontanelle, you may use US
- Some literature for ultrasound of optic nerve diameter (if normal (3.3cm), lower chance of elevated ICP)[citation needed]
- Shunt series
Management
- Assume shunt malfunction in patients with suggestive features regardless of findings on imaging
- Revisions are extremely common, low threshold to contact Neurosurgery
- Ventriculoperitoneal shunt drainage
Disposition
See Also
References
- ↑ Drake JM, Kestle JRW, Tuli S. CSF shunts 50 years on past, present and future. Child’s Nerv Syst. 2000; 16:800–804.