Vaginal bleeding in pregnancy (less than 20wks)
Background
- Occurs in 20-40% of 1st trimester pregnancies
- Once IUP is confirmed by ultrasound no utility in obtaining B-hCG
- US
- Do not use hCG to determine whether ultrasound should be obtained
Abortion Types
| Classification | Characteristics | OS | Fetal Tissue Passage | Misc |
|---|---|---|---|---|
| Threatened | Abdominal pain or bleeding; < 20 weeks gestation | Closed | No | If < 11 weeks (with fetal cardiac activity) 90% progress to term. If between 11 and 20 weeks 50% progress to term |
| Inevitable | Abdominal pain or bleeding; < 20 weeks gestation | Open | No | |
| Incomplete | Abdominal pain or bleeding; < 20 weeks gestation | Open | Yes, some | |
| Complete | Abdominal pain or bleeding; < 20 weeks gestation | Closed | Yes, complete expulsion of products | Distinguish from ectopic based on decreasing hCG and/or decreased bleeding |
| Missed | Fetal death at <20 weeks without passage of any fetal tissue for 4 weeks after fetal death | Closed | No | |
| Septic | Infection of the uterus during a miscarriage. Most commonly caused by retained products of conception | Open | No, or may be incomplete | Uterine tenderness and purulent discharge from the OS may be present |
Clinical Features
History
- Previous spontaneous abortion
- Extent of bleeding, clots, tissue
- Often quantified by pads per hour, greater than 1 per hour is concerning
- Presence of cramping
- Light-headedness? Chest pain? Shortness of breath? Palpitations?
Physical
- Uterus able to palpated in abdomen ~ 12 weeks
- Uterus able to visualzed by abdominal ultrasound ~ 10 weeks
- Open os decreases, but does not rule-out, ectopic
- If products of conception obtained send to pathology to rule-out trophoblastic disease
- Can quantify amount of bleeding by number of scopettes of blood on pelvic exam
- Large subchorionic hemorrhage increases chances of a miscarriage
Normal Vitals in Pregnancy[1]
| Vital | Nonpregnant | 1st Trimester | 2nd Trimester | 3rd Trimester |
| HR | 70 | 78 | 82 | 85 |
| SBP | 115 | 112 | 112 | 114 |
| DBP | 70 | 60 | 63 | 70 |
| Hcrt | 40 | 36 | 33 | 34 |
| WBC | 7.2k | 9.1k | 9.7k | 9.8k |
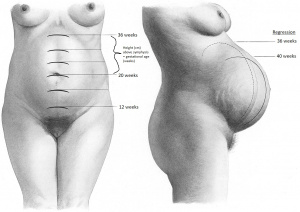
Estimated Gestational Age by Fundal Height[2]
| Weeks | Fundal Height / Finding |
| 12 | Pubic symphysis |
| 20 | Umbilicus |
| 20-32 | Height (cm) above symphysis = gestational age (weeks) |
| 36 | Xiphoid process |
| >37 | Regression |
| Post delivery | Umbilicus |
Differential Diagnosis
Vaginal Bleeding in Pregnancy (<20wks)
- Ectopic pregnancy
- Subchorionic hematoma
- First Trimester Abortion
- Complete Abortion
- Incomplete Abortion
- Inevitable Abortion
- Missed Abortion
- Septic abortion
- Threatened Abortion
- Gestational trophoblastic disease
- Consider when pregnancy-induced hypertension is seen before 24 wks of gestation
- Heterotopic pregnancy
- Implantation bleeding
- Molar pregnancy
- Non-pregnancy related bleeding
- Cervicitis
- Fibroids
- Implantation bleeding
Evaluation
See also maternal vitals and labs in pregnancy
Work-Up
- B-hCG (quantitative)
- CBC and BMP
- Coags
- T&S (Rh) vs. T&C
- Urinalysis
- Pelvic ultrasound
Diagnosis
Diagnostic Algorithm
- By ultrasound finding:
- +IUP = threatened abortion
- Ectopic ruled-out unless on fertility drugs
- Empty uterus + free fluid/adnexal mass = Ectopic
- Empty uterus + no free fluid / no mass
- +IUP = threatened abortion
Discrimatory Zone[3]
Values are for IUP visualization, not ectopic visualization
- Pelvic Ultrasound: hCG >1500
- Abd Ultrasound: hCG >3000[4]
Management
- RhoGAM if Rh Negative
- ACOG Clinical practice guideline recommends forgoing routine Rh testing and RhIg administration at <12 weeks of gestation[5]
- Assess need for transfusion (severe anemia or hypotension)
- Treat specific process:
- Ectopic
- Threatened abortion
- Indeterminate
Disposition
- Admit for:
- Ectopic
- Life threatening bleeding
- Surgical abdomen
See Also
Vaginal bleeding (main)
External Links
- https://bridgetotreatment.org/resource/ectopic-pregnancy-in-the-ed-unrestricted/
- https://bridgetotreatment.org/resource/ed-management-of-early-pregnancy-loss-misoprostol-protocol/
References
- ↑ Kuklina EV, Ayala C, Callaghan WM. Hypertensive disorders and severe obstetric morbidity in the United States. Obstet Gynecol 2009; 113:1299-1306.
- ↑ Vasquez V, Desai S. Labor and delivery and their complications. In: Walls RM, Hockberger RS, Gausche-Hill M, et al., eds. Rosen’s Emergency Medicine: Concepts and Clinical Practice. 9th ed. Philadelphia, PA: Elsevier Saunders; 2018:2296–2312.
- ↑ Ankum WM, Van der Veen F, Hamerlynck JV, Lammes FB. Suspected ectopic pregnancy. What to do when human chorionic gonadotropin levels are below the discriminatory zone. J Reprod Med. 1995;40:525–8
- ↑ Wag, R. et al. Use of a !-hCG Discriminatory Zone With Bedside Pelvic Ultrasonography. Annals of Emergency Medicine. 58(1)12-20. PDF
- ↑ (2024). ACOG Clinical Practice Update: Rh D Immune Globulin Administration After Abortion or Pregnancy Loss at Less Than 12 Weeks of Gestation. Obstetrics & Gynecology, 144 (6), e140-e143. doi: 10.1097/AOG.0000000000005733.