Celiac disease
Background[1][2][3]
- Also known as “Celiac Sprue”
- Affects 0.6 to 1.0% of worldwide population
- Occurs in industrialized countries and developing countries among all ethnicities and races
- Occurs in children and adults
- 1.5 to 2 times more prevalent in females than in males
- Gluten is found in wheat, rye, and barley
- Associated with strong family history, Type 1 DM, autoimmune thyroid disorders along with other autoimmune disorders, Turner’s syndrome, and Down syndrome
- Rotavirus infection in children increases risk of developing disease
- Breastfeeding reported to reduce risk by 50%
- MHC class II proteins HLA-DQ2 (90%) and HLA-DQ8 are expressed in almost all of patients affected by Celiac disease
Pathophysiology[1][2]
- Gluten triggers an immune mediated systemic disorder
- Can be weeks to years between gluten exposure and onset of symptoms
- Gluten is mainly composed of prolamine and glutanin
- Prolamines (such as Gliadin found in wheat) interact with intestinal cells to cause breakdown of the inter-enterocyte tight junctions
- Proposed that HLA-DQ2 and HLA-DQ8 present prolamines to antigen-specific CD4+ T lymphocytes in lamina propria of the small bowel
- Once activated, CD4+ T cells release pro-inflammatory cytokines and activate T-helper cells
- Proinflammatory cytokines such as IL-15 stimulate CD8+ T-lymphocytes
- T-helper type 1 cells release IFN-gamma
- T-helper type 2 cells promote conversion of B cells to plasma cells that produce anti-gliadin and anti-tissue-transglutaminase antibodies that are used in serologic testing
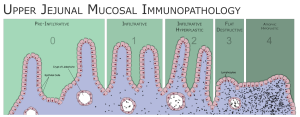
- This process leads to celiac enteropathy with histological features such as decreased enterocyte height, crypt hyperplasia, villous atrophy, and increased intraepithelial T lymphocytes
Clinical Features
Classic Features
- Classically presents around 6 to 18 months of age when foods containing gluten are introduced but can occur anytime
- Chronic diarrhea
- Weight loss
- Abdominal distension
- Iron deficiency with or without anemia
- Aphthous stomatitis
- Short stature
- High aminotransferase levels
- Chronic fatigue
- Reduced bone mineral density
- Vitamin D deficiency
Atypical Features
- Few or no gastrointestinal symptoms
- Older children or adults
- Dermatitis herpetiformis
- Gluten Ataxia
Silent or Asymptomatic From
- Patients have no symptoms
- Diagnosed based on serology of histology
- Found in patients with strong family history of disease, autoimmune disorders, chromosomal disorders (Down syndrome)
Refractory Form
- Persistent or recurrent symptoms or villous atrophy despite gluten free diet for 12 months
Celiac Crisis[4]
- Life threatening
- Often observed after a general immune stimulus such as surgery or infection
- Mostly observed in children
- Severe diarrhea
- Hypoproteinemia
- Metabolic and electrolyte disturbances
Complications from untreated disease[1][2][3]
- Osteoporosis
- Impaired splenic function
- Infertility
- Recurrent abortion
- Ulcerative jejunoileitis
- Enteropathy-associated intestinal T-cell lymphoma
- Adenocarcinoma of the jejunum
- Non-Hodgkin lymphoma
- Vitamin deficiencies
Differential Diagnosis
- Acute diarrhea
- Chronic diarrhea
- Irritable bowel syndrome
- Small intestinal bacterial overgrowth
- Lactose intolerance
- Chronic pancreatitis
- Microscopic colitis
- Inflammatory bowel disease
- Non-celiac gluten sensitivity (NCGS)
- Wheat allergy
- Vitamin or mineral deficiency
Evaluation[1]
- Rule out emergent causes of abdominal pain such as appendicitis, small bowel obstruction, bowel perforation, etc.
- Depending on presentation, chemistry panel and/or abdominal imaging may be appropriate in the emergency department setting
| Test | Sensitivity | Specificity | Comments |
| IgA anti-tTG antibodies | >95 | >95 | Screening test |
| IgG anti-tTG antibodies | Variable | Variable | Screening test in patients with IgA deficiency |
| IgA antendomysial antibodies | >90 | 98.2 | Useful if diagnosis unclear |
| IgG DGP | >90 | >90 | IgA deficiency and young patients |
| HLA DQ2 or HLA-DQ8 | 91 | 45 | High NPV |
Celiac Crisis[4]
- History and physical
- Assessment of volume status
- CBC to look for evidence of iron deficiency anemia
- CMP
- VBG
- Lactic acid
| Signs of severe dehydration including: hemodynamic instability and/or orthostatic changes |
| Neurologic dysfunction |
| Renal dysfunction: creatinine >2.0 g/dL |
| Metabolic acidosis: pH <7.35 |
| Hypoproteinemia (Albumin < 3.0 g/dL) |
| Abnormal electrolytes including: hyper/hyponatremia, hypocalcemia, hypokalemia or hypomagnesemia |
| Weight loss > 10 lbs |
Management
Uncomplicated Celiac disease
- Avoid wheat, rye, barley which all contain gluten
- Possible benefit to avoiding large amounts of Oats
- IV fluids if necessary
Celiac Crisis[4]
- Fluid resuscitation
- Oral or IV steroids
- Supplemental nutrition
- Electrolyte repletion
- Gluten free diet
Disposition
Uncomplicated Celiac disease
- Primary care follow up:
- Serology, histology, and likely EGD
- consultation with dietitian
- treatment of nutritional deficiencies
- referral to specialists
- serologic monitoring for recurrence
Celiac Crisis
- Hospital admission
See Also
References
- ↑ 1.0 1.1 1.2 1.3 Fasano A, Catassi C. Celiac Disease. New England Journal of Medicine. 2012;367(25):2419-2426. doi:10.1056/nejmcp1113994.
- ↑ 2.0 2.1 2.2 Parzanese I. Celiac disease: From pathophysiology to treatment. World Journal of Gastrointestinal Pathophysiology. 2017;8(2):27-38. doi:10.4291/wjgp.v8.i2.27.
- ↑ 3.0 3.1 Freeman HJ. Adult Celiac Disease and Its Malignant Complications. Gut and Liver. 2009;3(4):237-246. doi:10.5009/gnl.2009.3.4.237.
- ↑ 4.0 4.1 4.2 Jamma S, Rubio–Tapia A, Kelly CP, et al. Celiac Crisis Is a Rare but Serious Complication of Celiac Disease in Adults. Clinical Gastroenterology and Hepatology. 2010;8(7):587-590. doi:10.1016/j.cgh.2010.04.009.