Mild traumatic brain injury
Background
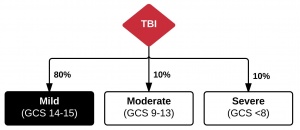
- Definition: GCS 14-15
- Neurologic dysfunction that varies without gross lesions (ie patients have trouble with memory, attention, and executive functioning
- Occurs after a blunt force or acceleration-deceleration head injury
- Likely secondary to metabolic insult ie low oxygen state, ion changes
- Structural imaging on MRI or CT might not indicate any injury
- Often evidence on microscopic level of injury with histology
- Important to not expose the already injured brain to repeated insults which is why there are usually worsening symptoms after a repeat concussion
Epidemiology
- 2.5 million people sustain a TBI in the United States every year
- 75 to 95 percent, are mild
- Most common causes of TBI are motor vehicle accidents (20 to 45 percent), falls (30 to 38 percent), occupational accidents (10 percent), recreational accidents (10 percent), and assaults (5 to 17 percent)
TBI Pathophysiology
Primary injury
- Contusions
- Bruises to brain parenchyma
- Hematomas
- Epidural hematoma
- Subdural hematoma
- Intraparenchymal
- Intraventricular
- Subarachnoid hemorrhage
- Diffuse axonal injury
- Direct cellular damage
- Neurons
- Axons
- Tearing and shearing of tissues
Secondary injury
Brain swelling causes increased ICP which compresses the tissue causing ischemia with direct compression of the vasculature causing brain tissue herniation and brain death
- Leads to expansion of the original injury (predominantly metabolic insult)
- Calcium and sodium shifts
- Mitochondrial damage
- Production of free radicals
- Ultimately leads to damage to axonal integrity and axonal transport
- Enzyme activity leads to apoptosis
- Microscopic structural injury is often unidentifiable on CT or MRI
Cerebral Blood Flow and Autoregulation
- vasoconstriction
- HTN, Hypocarbia, alkalosis
- No good way to measure cerebral blood flow
- Use CPP as surrogate
- CPP is amount of pressure needed to perfuse the brain
- CPP=MAP-ICP
- When ICP elevates, CPP decreases
- Normal ICP
- 15 in adults
- <10 to 15 in children
- 1.5 to 6.0 in infants
- Use CPP as surrogate
- Autoregulation allows the body to control the cerebral blood flow
- Autoregulatory mechanism is damaged in most TBI patients
Clinical Features
- Most consistent abnormality is subtle impairments in cognitive function (concussion symptoms)
- Attention, concentration, amnesia, memory, processing speed, reaction time, calculation, executive function
- Physical signs/symptoms
- Behavioral changes
- Irritability, depression, anxiety, sleep disturbances, problems related to school/work, emotional lability, loss of initiative, loneliness, and helplessness
Differential Diagnosis
Head trauma
- Traumatic brain injury
- Intracranial hemorrhage
- Intra-axial
- Extra-axial
- Moderate-to-severe traumatic brain injury
- Mild traumatic brain injury
- Intracranial hemorrhage
- Orbital trauma
- Maxillofacial trauma
- Scalp laceration
- Skull fracture
- Pediatric head trauma
Evaluation
Workup
- Consider head CT (rule out intracranial hemorrhage)
- Use validated decision rule to determine need
- Avoid CT in patients with minor head injury who are at low risk based on validated decision rules.[1]
- Consider cervical and/or facial CT
Westmead post-traumatic amnesia scale
Any wrong answer to following questions is considered positive for cognitive impairment after head injury
- What is your name?
- What is the name of this place?
- Why are you here?
- What month are we in?
- What year are we in?
- What town/suburb are you in?
- How old are you?
- What is your date of birth?
- What time of day is it? (morning, afternoon, evening)
- Three pictures are presented for subsequent recall
Diagnosis
- Clinically made, no reliable test that can confirm diagnosis of concussion
- Signs and symptoms may occur immediately or be delayed by days-weeks (see also post-concussive syndrome)
Types
- Simple concussion
- Gradual resolution of symptoms within 7-10d
- Complex concussion
- Persisting symptoms or cognitive impairment
- Symptoms with exertion
Management
Simple
- Limitations on playing and training while symptomatic
- Follow up with primary care provider
Complex
- Refer to sports medicine or concussion specialist
Disposition
Admit
Patient requires inpatient observation if GCS <15, seizure activity present, anticoagulation or bleeding diathesis, or no responsible caregiver to discharge to
Discharge
Patient may be discharged for outpatient observation if (all of the following):
- No head CT required per above criteria OR head CT performed and not requiring neurosurgical intervention
- Patient GCS 15 on discharge
- No seizures
- No anticoagulation or bleeding diathesis
- Responsible caregiver at home to discharge to
Discharge instructions
- Given good follow up instructions detailing a graded return-to-activity program and symptoms to anticipate during recovery [2]
- Encourage cognitive rest and avoidance of repetitive head injuries
- Discharge patient to care of responsible individual
- Patients might not understand discharge instructions so repeat them to the individual taking care of the patient
- In one study of adolescents, strict rest immediately after mild TBI offered no benefit. [3]
- Physical activity at any level (light aerobic, moderate, full) within first 7 days compared with no activity associated with lower rates of persistent symptoms at 28 days (29% vs. 40%)[4]
- Multicohort study - 2400 children, aged 5-18, in the emergency department
- Still recommend strict rest for first 24-48 hours
- Follow up for full examination, gait and cognition testing
- Mini-Mental State Exam
- Standardized Assessment for Concussion
- Takes 10-15 mins to administer, often not performed in ED
Modified brain injury guideline (mBIG)
For adults with mild TBI (GCS 13–15) and traumatic intracranial hemorrhage on CT, the Modified brain injury guideline (mBIG) stratifies risk to guide neurosurgical consultation, ICU admission, and safe discharge:
Scope: mBIG applies ONLY to traumatic intracranial hemorrhage in adults with mild traumatic brain injury (GCS 13–15). It is not applicable to spontaneous/aneurysmal subarachnoid hemorrhage, spontaneous intracerebral hemorrhage, or any non-traumatic intracranial hemorrhage.
mBIG 1 (lowest risk)
All of the following must be true:
- GCS 15
- No loss of consciousness (LOC)
- No seizure
- No emesis
- Isolated SDH ≤4 mm, isolated EDH ≤4 mm, isolated tSAH ≤4 mm, cerebral contusion ≤2 cm, or intraventricular hemorrhage ≤2 mm
- No herniation or significant mass effect on CT
- Neurologically intact
Disposition: No neurosurgical consultation required; observation in non-monitored setting acceptable; repeat CT imaging not required if clinically stable; may be appropriate for discharge with reliable follow-up.
mBIG 2 (intermediate risk)
Meets any of the following (but does not meet mBIG 3 criteria):
- GCS 13–14, OR
- LOC, OR
- Isolated seizure, OR
- Emesis, OR
- CT findings larger than mBIG 1 thresholds but without herniation/significant mass effect
Disposition: Neurosurgical consultation warranted; admission to step-down or monitored unit; repeat head CT in 4–6 hours or per neurosurgical guidance.
mBIG 3 (highest risk)
Any of the following:
- GCS <13 (note: if GCS <13, patient may not strictly qualify as "mild TBI" — manage per moderate-to-severe traumatic brain injury pathway)
- Any herniation on CT
- Significant mass effect (midline shift >5 mm, cisternal effacement)
- Bilateral or mixed intracranial hemorrhage pattern with neurologic decline
- Neurovascular injury identified
Disposition: Emergent neurosurgical consultation; ICU admission; operative intervention frequently required.
Prognosis
See also post-concussive syndrome
- At 3 mo after injury 20-40% are symptomatic
- At 1 yr after injury 15% are symptomatic
Calculators
PECARN Pediatric Head Injury
| Age Group | Select One |
|---|---|
| Patient Age | 1 <2 years ≥2 years |
| Criteria | No | Yes |
|---|---|---|
| GCS <15 (altered mental status) | 1 | |
| Palpable skull fracture | 1 | |
| Occipital/parietal/temporal scalp hematoma | 1 | |
| Loss of consciousness ≥5 seconds | 1 | |
| Not acting normally per parent | 1 | |
| Severe mechanism of injury (MVC with ejection/rollover/fatality, pedestrian/cyclist without helmet struck by motorized vehicle, fall >3 feet, head struck by high-impact object) | 1 | |
| Risk Factors (<2y) | / 6 | |
| Criteria | No | Yes |
|---|---|---|
| GCS <15 (altered mental status) | 1 | |
| Signs of basilar skull fracture (hemotympanum, raccoon eyes, Battle sign, CSF otorrhea/rhinorrhea) | 1 | |
| Vomiting | 1 | |
| Loss of consciousness | 1 | |
| Severe headache | 1 | |
| Severe mechanism of injury (MVC with ejection/rollover/fatality, pedestrian/cyclist without helmet struck by motorized vehicle, fall >5 feet, head struck by high-impact object) | 1 | |
| Risk Factors (≥2y) | / 6 | |
| Interpretation (for selected age group) | |
|---|---|
| 0 | Very low risk — ciTBI risk <0.02% (<2y) or <0.05% (≥2y). CT not recommended. |
| 1 (intermediate*) | Low risk — ciTBI risk ~0.9% (<2y) or ~0.8% (≥2y). Observation vs. CT. *Only if GCS=15 and no skull fracture/AMS. Consider observation for 4-6 hours. |
| GCS<15 or skull fx | High risk — ciTBI risk 4.4% (<2y) or 4.3% (≥2y). CT recommended. |
| References |
|---|
|
Canadian CT Head Rule
| High Risk (for neurosurgical intervention) | ||
|---|---|---|
| Criteria | No | Yes |
| GCS <15 at 2 hours after injury | 1 | |
| Suspected open or depressed skull fracture | 1 | |
| Any sign of basal skull fracture (hemotympanum, raccoon eyes, CSF otorrhea/rhinorrhea, Battle sign) | 1 | |
| Vomiting ≥2 episodes | 1 | |
| Age ≥65 years | 1 | |
| Medium Risk (for brain injury on CT) | ||
| Amnesia before impact >30 min | 1 | |
| Dangerous mechanism (pedestrian struck, occupant ejected, fall from ≥3 feet or ≥5 stairs) | 1 | |
| High Risk Criteria | / 5 | |
| Medium Risk Criteria | / 2 | |
| Interpretation | |
|---|---|
| All No | CT NOT required — Low risk for clinically important brain injury. Safe for discharge with head injury instructions. |
| Medium risk ≥1 | CT recommended — Risk of brain injury on CT. Imaging indicated. |
| High risk ≥1 | CT required — High risk for neurosurgical intervention. Urgent CT head. |
| References |
|---|
|
See Also
References
- ↑ Choosing wisely ACEP
- ↑ Ronsford J, et al. Impact of early intervention on outcome after mild traumatic head in adults. 2002
- ↑ Thomas DG, Apps JN, Hoffmann RG, et al. Benefits of strict rest after acute concussion: a randomized controlled trial. Pediatrics. 2015; 2(135):213-223.
- ↑ Grool AM et al. Association Between Early Participation in Physical Activity Following Acute Concussion and Persistent Postconcussive Symptoms in Children and Adolescents. JAMA. 2016;316(23):2504-2514.