Multiple sclerosis
(Redirected from MS)
Background
- CNS myelin destruction causes variable motor, sensory, visual and cerebellar dysfunction[1]
- Peak onset age 20-40 years, F:M ratio ~3:1
- More common in populations of Northern European descent and at higher latitudes
Types
- Clinically isolated syndrome (CIS)
- Single first episode of neurologic symptoms lasting ≥24 hours, caused by CNS demyelination
- May or may not progress to MS
- Radiologically isolated syndrome (RIS)
- Incidental MRI findings suggestive of MS in asymptomatic patients
- Relapsing/remitting (most common)
- Relapse (days-months) followed by remission
- Secondary progressive
- Relapses and partial recoveries occur, but disability does not fade away between cycles
- Primary progressive
- Symptoms progress slowly and steadily without remission
- Progressive relapsing
- Similar to primary progressive but with superimposed flares
Clinical Features
- Classic patient has multiple presentations for neuro symptoms of different areas of pathology
- Patient often has resolution of the earlier symptoms
- Symptoms worsen with increases in body temperature, classically after hot showers (Uhthoff's phenomenon[2])
- Muscle/sensory signs:
- Lower extremity weakness usually worse than upper extremity
- Upper motor neuron signs:
- Hyperreflexia
- Positive Babinski
- Decrease in proprioception/pain/temperature sensation
- Lhermitte sign
- Electric shock sensation radiating down back into arms/legs from neck flexion
- If the discomfort is severe, carbamazepine or gabapentin may be beneficial for some patients.
- Partial transverse myelitis
- Asymmetric motor/sensory deficits at a spinal cord level
- One of the most common acute presenting syndromes
- Trigeminal neuralgia
- Bilateral trigeminal neuralgia in a young patient should raise suspicion for MS
- Optic neuritis
- Initial sign in 30% of patients
- Vision loss (usually unilateral) often preceded by retrobulbar pain
- Blurred vision
- Afferent pupillary defect is suggestive of optic neuritis
- Nystagmus
- Diplopia
- Internuclear ophthalmoplegia
- Impaired adduction of the adducting eye with nystagmus of the abducting eye
- Bilateral INO is classic for MS
- Convergence (both eyes center medially) is preserved
- Dysautonomia
- Urinary retention (increased risk of UTI/pyelo)
- Constipation or incontinence
- Sexual dysfunction (males)
- Other common symptoms
- Fatigue — most common symptom overall; frequent reason for ED presentation
- Cognitive dysfunction (up to 50% of patients)
Differential Diagnosis
Weakness
- Neuromuscular weakness
- Upper motor neuron:
- CVA
- Hemorrhagic stroke
- Multiple sclerosis
- Amyotrophic Lateral Sclerosis (ALS) (upper and lower motor neuron)
- Lower motor neuron:
- Spinal and bulbar muscular atrophy (Kennedy's syndrome)
- Spinal cord disease:
- Infection (Epidural abscess)
- Infarction/ischemia
- Trauma (Spinal Cord Syndromes)
- Inflammation (Transverse Myelitis)
- Degenerative (Spinal muscular atrophy)
- Tumor
- Peripheral nerve disease:
- Neuromuscular junction disease:
- Muscle disease:
- Rhabdomyolysis
- Dermatomyositis
- Polymyositis
- Alcoholic myopathy
- Upper motor neuron:
- Non-neuromuscular weakness
- Can't miss diagnoses:
- ACS
- Arrhythmia/Syncope
- Severe infection/Sepsis
- Hypoglycemia
- Periodic paralysis (electrolyte disturbance, K, Mg, Ca)
- Respiratory failure
- Emergent Diagnoses:
- Symptomatic Anemia
- Severe dehydration
- Hypothyroidism
- Polypharmacy
- Malignancy
- Aortic disease - occlusion, stenosis, dissection
- Other causes of weakness and paralysis
- Acute intermittent porphyria (ascending weakness)
- Can't miss diagnoses:
Evaluation
Known MS Patient with Exacerbation
- Urinalysis — rule out occult UTI as pseudorelapse trigger (very common in MS)
- CBC, Chemistry
- Consider CXR or other infectious workup based on presentation
- Temperature — fever suggests pseudorelapse or infection
- MRI with GAD generally not needed emergently unless diagnostic uncertainty or concern for PML
- LP is generally not needed for exacerbation of known MS — defer to neurology
Suspected New Diagnosis
- MRI with GAD of brain (+/- spine) and orbits (if optic neuritis suspected)
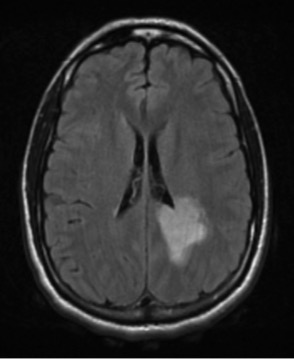
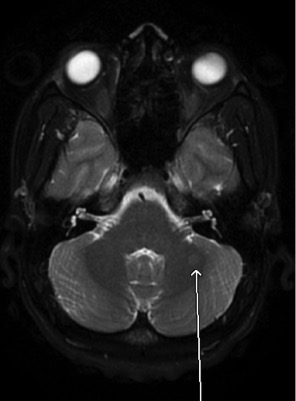
- Multiple lesions in supratentorial white matter, paraventricular area, spinal cord
- CSF
- Elevated protein and gamma-globulin (increased oligoclonal bands)
- Generally can be deferred to neurology
- CBC, Chemistry
- Urinalysis
- TSH, B12, RPR/VDRL — rule out MS mimics
- Consider NMO/aquaporin-4 antibody testing (especially if longitudinally extensive transverse myelitis or bilateral optic neuritis)[3]
Management
Pseudorelapse vs True Relapse
| True Relapse | Pseudorelapse | |
|---|---|---|
| Definition | New inflammatory demyelinating event | Temporary worsening of old symptoms from an external trigger |
| Duration | >24 hours, evolves over hours to days, persists days to weeks | Typically <24 hours; resolves when trigger is removed |
| Triggers | None (not explained by fever or infection) | Infection (especially UTI), fever, heat, stress, dehydration, medication changes |
| Symptoms | New neurologic symptoms OR worsening in a new distribution | Recurrence of prior/known deficits; symptoms may fluctuate |
| MRI | Often shows new gadolinium-enhancing lesion | No new lesion |
| Treatment | High-dose corticosteroids | Treat the underlying trigger; steroids are not indicated |
- Always check UA and infectious workup before initiating steroids — occult UTI is a very common pseudorelapse trigger in MS patients
- If symptoms are identical to a prior relapse, pseudorelapse is more likely (MS rarely causes repeated inflammation in the same CNS location)
- Symptoms that fluctuate or resolve completely and then return favor pseudorelapse[6]
Fever and Infection
- Fever must be reduced to minimize weakness associated with elevated temperature
- Antibiotics or surgical control of any infectious sources
Steroids
- High-dose steroid therapy for true relapses in the form of oral or intravenous methylprednisolone (1000 mg daily x 3-5 days)[7]
- Oral methylprednisolone at equivalent doses is non-inferior to IV and allows for outpatient treatment
- Do not initiate steroids until infection has been ruled out as the cause of symptom worsening
Plasma Exchange (PLEX)
- Second-line treatment for severe relapses refractory to high-dose corticosteroids[8]
- ~20-35% of patients may not fully respond to steroids alone
- Typically 5-7 sessions over 10-14 days
- Consult neurology early if relapse is severe or not responding to steroids
Disease-Modifying Therapies (DMTs)
- Suppression therapies (IFN-β, Glatiramer, etc.) — initiation is generally not in ED
- However, ED physicians should be aware of complications of DMTs in patients already on treatment:
| DMT | ED-Relevant Complications |
|---|---|
| Natalizumab (Tysabri) | Risk of PML (progressive multifocal leukoencephalopathy) — any new neurologic worsening warrants urgent MRI and JC virus testing |
| Fingolimod / Siponimod | Bradycardia, cardiac conduction abnormalities, macular edema |
| Ocrelizumab, Rituximab (anti-CD20) | Increased infection risk, infusion reactions, reactivation of hepatitis B |
| Interferons (Avonex, Rebif) | Flu-like symptoms (may mimic infection), hepatotoxicity, cytopenias |
| Dimethyl fumarate (Tecfidera) | Lymphopenia (increased infection risk); rare PML risk |
Disposition
Discharge
- Mild relapse in a patient who can ambulate safely
- Able to tolerate oral medications (oral methylprednisolone non-inferior to IV)
- Has reliable follow-up with neurology (ideally within 1-3 days)
- No untreated infection
- Adequate social support
Admission
- Any disease exacerbation associated with significant morbidity or functional impairment
- IV antibiotics or steroid therapy required
- Inability to ambulate safely or care for self
- Urinary retention requiring catheterization
- Concern for PML or other serious DMT complication
- Depression and significant risk of suicide
- Need for plasma exchange
Neurology Consultation
- New suspected MS diagnosis
- Severe relapse with significant functional impairment
- Steroid-refractory symptoms (discuss PLEX)
- Concern for PML or other DMT-related complication
- Diagnostic uncertainty
Return Precautions
- Worsening weakness or new weakness
- New or worsening visual symptoms
- Inability to urinate or new incontinence
- Difficulty breathing or swallowing
- Fever
See Also
References
- ↑ Multiple sclerosis: a practical overview for clinicians. British Medical Bulletin, Volume 95, Issue 1, September 2010, Pages 79–104. https://doi.org/10.1093/bmb/ldq017
- ↑ Flensner G, et al. "Sensitivity to heat in MS patients: a factor strongly influencing symptomology-an explorative survey". BMC Neurol. 2011. 11:27.
- ↑ Pelletier J, et al. "Multiple Sclerosis: An Emergency Medicine-Focused Narrative Review." J Emerg Med. 2024;66(4):e441-e456.
- ↑ Mellen Center Approaches: Management of MS Relapses. Cleveland Clinic Mellen Center for Multiple Sclerosis Treatment and Research. https://my.clevelandclinic.org/departments/neurological/depts/multiple-sclerosis/ms-approaches/relapse-management-ms
- ↑ Defined by Thompson AJ, et al. "Diagnosis of multiple sclerosis: 2017 revisions of the McDonald Criteria." Lancet Neurol. 2018;17(2):162-173.
- ↑ Amin A, et al. "Triaging Patients with Multiple Sclerosis in the Emergency Department: Room for Improvement." Proc Bayl Univ Med Cent. 2022;36(2):186-189.
- ↑ Le Page et al. Oral versus intravenous high-dose methylprednisolone for treatment of relapses in patients with multiple sclerosis (COPOUSEP): a randomised, controlled, double-blind, non-inferiority trial. Lancet. 2016 Jan 23;387(10016):340. https://core.ac.uk/download/pdf/52993687.pdf
- ↑ Ehler J, et al. "Therapeutic Plasma Exchange in Multiple Sclerosis and Autoimmune Encephalitis." J Clin Med. 2019;8(10):1793.
- ↑ Pelletier J, et al. "Multiple Sclerosis: An Emergency Medicine-Focused Narrative Review." J Emerg Med. 2024;66(4):e441-e456.