Acute fatty liver of pregnancy/es: Difference between revisions
Ostermayer (talk | contribs) (Created page with "==Antecedentes==") |
Ostermayer (talk | contribs) (Created page with "thumb|Vista inferior del hígado con superficie que muestra lóbulos e impresiones. *Complicación rara, potencialmente mortal que se presenta en la segunda mitad del embarazo o (menos comúnmente) a principios del postparto *Etiología exacta poco clara, pero se cree que implica un metabolismo anormal de los ácidos grasos fetales *Vesículas de grasa se acumulan dentro de los hepatocitos, interfiriendo con la función hepática") |
||
| Line 11: | Line 11: | ||
==Características clínicas== | ==Características clínicas== | ||
*Por lo general, se presenta en el 3er trimestre, pero puede ocurrir en cualquier momento de la segunda mitad del embarazo hasta el postparto temprano | |||
*[[Special:MyLanguage/Nausea/vomiting|Nausea/vomiting]] (comúnmente severa) | |||
*[[Special:MyLanguage/Nausea/vomiting|Nausea/vomiting]] ( | |||
*[[Special:MyLanguage/Jaundice|Jaundice]] | *[[Special:MyLanguage/Jaundice|Jaundice]] | ||
* | *Hallazgos consistentes con [[Special:MyLanguage/preeclampsia|preeclampsia]] en algunas mujeres: | ||
**[[Special:MyLanguage/Hypertension|Hypertension]] | **[[Special:MyLanguage/Hypertension|Hypertension]] | ||
**Edema | **Edema | ||
**[[Special:MyLanguage/Proteinuria|Proteinuria]] | **[[Special:MyLanguage/Proteinuria|Proteinuria]] | ||
*[[Special:MyLanguage/Hypoglycemia|Hypoglycemia]] | *[[Special:MyLanguage/Hypoglycemia|Hypoglycemia]] | ||
* | *A menudo, signos/síntomas de [[Special:MyLanguage/DIC|DIC]] | ||
*+/- [[Special:MyLanguage/encephalopathy|encephalopathy]], [[Special:MyLanguage/ascites|ascites]] | *+/- [[Special:MyLanguage/encephalopathy|encephalopathy]], [[Special:MyLanguage/ascites|ascites]] | ||
==Diagnóstico diferencial== | |||
= | |||
{{Postpartum emergencies DDX}} | {{Postpartum emergencies DDX}} | ||
| Line 34: | Line 30: | ||
==Evaluación== | |||
= | |||
===Evaluación=== | |||
=== | |||
<div lang="en" dir="ltr" class="mw-content-ltr"> | <div lang="en" dir="ltr" class="mw-content-ltr"> | ||
Revision as of 17:13, 10 January 2026
Antecedentes
- Complicación rara, potencialmente mortal que se presenta en la segunda mitad del embarazo o (menos comúnmente) a principios del postparto
- Etiología exacta poco clara, pero se cree que implica un metabolismo anormal de los ácidos grasos fetales
- Vesículas de grasa se acumulan dentro de los hepatocitos, interfiriendo con la función hepática
Características clínicas
- Por lo general, se presenta en el 3er trimestre, pero puede ocurrir en cualquier momento de la segunda mitad del embarazo hasta el postparto temprano
- Nausea/vomiting (comúnmente severa)
- Jaundice
- Hallazgos consistentes con preeclampsia en algunas mujeres:
- Hypertension
- Edema
- Proteinuria
- Hypoglycemia
- A menudo, signos/síntomas de DIC
- +/- encephalopathy, ascites
Diagnóstico diferencial
3rd Trimester/Postpartum Emergencies
- Acute fatty liver of pregnancy
- Amniotic fluid embolus
- Chorioamnionitis
- Eclampsia
- HELLP syndrome
- Mastitis
- Peripartum cardiomyopathy
- Postpartum endometritis (postpartum PID)
- Postpartum headache
- Postpartum hemorrhage
- Preeclampsia
- Resuscitative hysterotomy
- Retained products of conception
- Septic abortion
- Uterine rupture
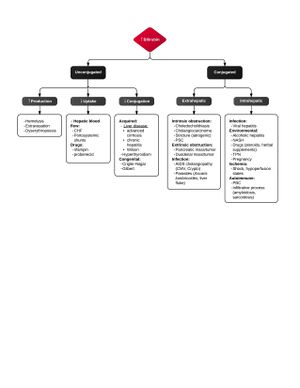
Jaundice
Indirect Hyperbilirubinemia
- Hemolytic
- G6PD
- Drug related
- Autoimmune hemolytic anemia
- Hematoma resorption
- Ineffective erythropoiesis
- Gilbert's
Direct (Conjugated) Hyperbilirubinemia
- Choledocholithiasis
- Cholecystitis
- Ascending cholangitis
- AIDS cholangiopathy
- Stricture
- Neoplasm
- Pancreatic head
- Gallbladder
- Primary liver (e.g. hepatocellular carcinoma)
- Metastatic
- Obstructing AAA
Hepatocellular damage
Patient will have severely elevated AST/ALT with often normal Alkaline Phosphatase
- Viral hepatitis
- Fulminant hepatic failure
- alcoholic hepatitis
- Ischemic hepatitis
- Toxins
- Isoniazid
- Phenytoin
- acetaminophen
- Ritonavir
- Halothane
- Sulfonamide
- Autoimmune hepatitis
- Primary biliary cirrhosis
- HELLP Syndrome
- Congestive Hepatopathy
Pregnancy Related
Transplant Related
Pediatric Related
- Inborn error of metabolism
- Neonatal jaundice (physiologic)
Additional Differential Diagnosis
- Reye syndrome
- TPN
- Heatstroke
- Budd-Chiari (with acute ascites)
- Wilson's disease
- Sarcoidosis
- Amyloidosis
Masqueraders
Only bilirubin stains the sclera
- Carotenemia
- Quinacrine ingestion
- Dinitrophenol, teryl (explosive chemicals)
Evaluación
Evaluación
- LFTs
- ALT/AST usually in 300-500 range, alk phos usually elevated in pregnancy
- Hyperbilirubinemia- more pronounced than in preeclampsia
- BMP
- DIC labs
- Low fibrinogen, coagulopathy
- DIC present in as many as 70% of patients[1]
- CBC
- Often shows leukocytosis
- UA
- RUQ US
- Non-specific; the liver can even be normal in echotexture
- Useful to rule out other causes of obstructive biliary tract pathology.
Diagnosis
- Often initially misdiagnosed as preeclampsia/HELLP
- Hypoglycemia, jaundice, ascites, hypofibrinogenemia all more common in AFLP
Swansea criteria[2]
At least six of the following findings, in the absence of another cause:
- Vomiting
- Abdominal pain
- Polydipsia/polyuria
- Encephalopathy
- Elevated bilirubin
- Hypoglycemia
- Elevated urea
- Leukocytosis
- Ascites or bright liver on ultrasound scan
- Elevated transaminases (AAT or ALT)
- Elevated ammonia
- Renal impairment: elevated creatinine
- Coagulopathy: elevated prothrombin time or PT
- Microvesicular steatosis on liver biopsy
Management
- Emergent Ob/Gyn consult
- Delivery typically results in rapid hepatic recovery
- Dextrose for hypoglycemia
- FFP, cryoprecipitate, and/or platelets for coagulopathy (see DIC)
Disposition
- Admit ICU or transfer to center with Ob
See Also
External Links