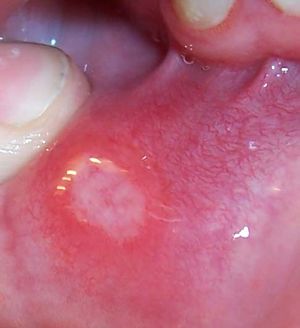
Aphthous stomatitis
Background
- Common oral ulcers (canker sores) affecting ~20% of the population
- Recurrent episodes; etiology unclear
- Triggers: stress, hormonal changes, local trauma, certain foods (citrus, chocolate, coffee), nutritional deficiencies (B12, folate, iron)
- Self-limited; resolve in 10-14 days without scarring (minor type)
Clinical Features
- Well-circumscribed, painful ulcers on nonkeratinized mucosa (labial, buccal mucosa, floor of mouth, ventral tongue)
- Central yellow-white fibrinous base with erythematous halo
- Key distinction from herpes: Aphthous ulcers are on non-keratinized mucosa and do NOT involve attached gingiva or hard palate (herpes involves keratinized mucosa)
- Types:
- Minor (<1 cm, most common, heals in 10-14 days)
- Major (>1 cm, deeper, may take weeks to heal, can scar)
- Herpetiform (clusters of tiny ulcers, mimics herpes but on non-keratinized mucosa)
Differential Diagnosis
Oral rashes and lesions
- Angioedema
- Aphthous stomatitis
- Herpes gingivostomatitis
- Herpes labialis
- Measles (Koplik's spots)
- Perioral dermatitis
- Oral thrush
- Steven Johnson syndrome
- Streptococcal pharyngitis
- Tongue diagnoses
- Vincent's angina
- Consider systemic disease if: Recurrent severe episodes, genital ulcers (Behcet's disease), GI symptoms (Crohn's), or systemic symptoms
Evaluation
- Clinical diagnosis
- Consider labs (CBC, iron, B12, folate) for recurrent or severe cases
- Biopsy if lesion does not respond to treatment or concern for malignancy
Management
- Pain control: Viscous lidocaine 2%, benzocaine gel, or magic mouthwash (equal parts viscous lidocaine, diphenhydramine, and antacid)
- Topical corticosteroids:
- Dexamethasone 0.01% elixir as mouth rinse
- Fluocinonide 0.05% gel applied to isolated lesions
- Betamethasone syrup
- Avoid irritating foods (acidic, spicy)
Disposition
- Discharge with symptomatic treatment
- Refer to oral medicine or ENT if recurrent severe episodes or non-healing ulcers