Anorectal abscess
(Redirected from Perianal abscess)
Background
- Usually begin via blocked anal gland (leads to infection/abscess formation)
- Can progress to involve any of the potential spaces.
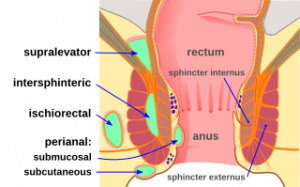
| Perianal | Ischiorectal | Intersphincteric, deep postanal, pelvirectal | |
| Epidemiology | Most common | Second most common | Least common |
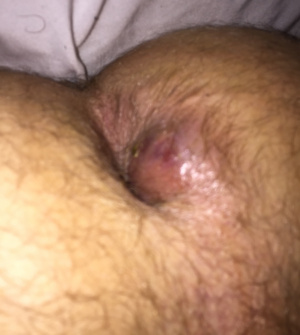
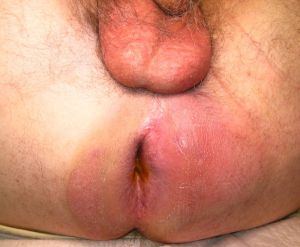
| Symptoms | Located close to anal verge, posterior midline, superficial tender mass | Larger, indurated, well-circumscribed, located laterally on medial aspect of buttocks | Rectal pain, skin signs may not be present |
| Comments | High incidence of fistula formation even with drainage | Constitutional symptoms often present |
Risk Factors
- Crohn's disease
- Chronic constipation
- Diabetes mellitus
- Chronic corticosteroid use
Clinical Features
- Worsening pain around bowel movement, with decreased pain post rectal evacuation
- Perirectal abscesses often accompanied by fever, leukocytosis
- May only be palpable via digital rectal exam
- Perianal abscesses typically do not cause fever in immunocompetent individuals
- Tender inguinal lymphadenopathy may be only clue to deeper abscesses
Differential Diagnosis
Anorectal Disorders
- Anal fissure
- Anal fistula
- Anal malignancy
- Anal tags
- Anorectal abscess
- Coccydynia
- Colorectal malignancy
- Condyloma acuminata
- Constipation
- Crohn's disease
- Cryptitis
- GC/Chlamydia
- Fecal impaction
- Hemorrhoids
- Levator ani syndrome
- Pedunculated polyp
- Pilonidal cyst
- Proctalgia fugax
- Proctitis
- Pruritus ani
- Enterobius (pinworms)
- Rectal foreign body
- Rectal prolapse
- Syphilitic fissure
Non-GI Look-a-Likes
Skin and Soft Tissue Infection
- Cellulitis
- Erysipelas
- Lymphangitis
- Folliculitis
- Hidradenitis suppurativa
- Skin abscess
- Necrotizing soft tissue infections
- Mycobacterium marinum
Look-A-Likes
- Sporotrichosis
- Osteomyelitis
- Deep venous thrombosis
- Pyomyositis
- Purple glove syndrome
- Tuberculosis (tuberculous inflammation of the skin)
Evaluation
- CT with IV contrast can be useful to define deep abscesses (especially with pain out of proportion to exam)
- May consider ultrasound or MRI as alternatives
Management
- Isolated perianal abscess is only type of anorectal abscess that should be treated in ED
- Consider either linear incision with packing, elliptical incision, or cruciate incision without packing
- Frequent sitz baths
- All perirectal abscesses (ischiorectal, intersphincteric, supralevator) should be drained in the OR
- All anorectal abscesses require surgical referral and follow up
Antibiotics
Causative organisms: Mixed infection with fecal flora for anaerobes and Gram Negatives (Bacteroides fragilis and Escherichia coli)
Use is controversial
- Only recommended in high risk patients:[1][2]
- Elderly
- Diabetics
- Systemic signs (fever, leukocytosis)
- Valvular heart disease
- Cellulitis
- Immunosuppression
- Possibly prevent fistula formation in otherwise healthy patients[3]
Treatment options:
- Augmentin
- Ciprofloxacin 500mg PO BID and Metronidazole 500mg PO TID
Disposition
Discharge
- Perianal abscess
See Also
External Links
References
- ↑ BMJ Best Practice Anorectal abscess http://bestpractice.bmj.com/best-practice/monograph/644/treatment/step-by-step.html
- ↑ Guidelines.gov - Practice parameters for the management of perianal abscess and fistula-in-ano.http://www.guideline.gov/content.aspx?id=36077
- ↑ Mocanu V, Dang JT, Ladak F, et al. Antibiotic use in prevention of anal fistulas following incision and drainage of anorectal abscesses: A systematic review and meta-analysis. Am J Surg. 2019;217(5):910-917.