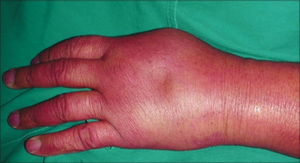
Purple glove syndrome
Background
- Uncommon skin complication of phenytoin
- Typically associated with IV infiltration of phenytoin, but poorly understood pathophysiology
- Proposed mechanisms include:[1]
- Chemical irritation from added propylene glycol and sodium hydroxide
- Vasoconstriction
- Vasculitis
- Microthrombus formation
- Phenytoin leakage into soft tissue with subsequent edema
- Generally develops within first 24 hours after infusion, resolves within days to weeks [2]
Clinical Features
- Peripheral edema, blistering, pain, and discoloration of the extremity receiving intravenous phenytoin
- Pulses and sensation may be diminished
- Skin necrosis may develop
Differential Diagnosis
- Simple IV fluid extravasation
- Arterial thrombosis
- Compartment syndrome
Skin and Soft Tissue Infection
- Cellulitis
- Erysipelas
- Lymphangitis
- Folliculitis
- Hidradenitis suppurativa
- Skin abscess
- Necrotizing soft tissue infections
- Mycobacterium marinum
Look-A-Likes
- Sporotrichosis
- Osteomyelitis
- Deep venous thrombosis
- Pyomyositis
- Purple glove syndrome
- Tuberculosis (tuberculous inflammation of the skin)
Evaluation
- Clinical diagnosis based on history and exam
Management
- Optimal management remains unclear
- Some case reports found improvement with
- topical nitroglycerin
- brachial plexus nerve block
- elevation, heat application, soft tissue massage
- Consider vascular or hand consult if digital or skin necrosis suspected
- Anticoagulation is occasionally started (no clear evidence that it is effective) [3]
Disposition
- Given possibility of severe outcomes, recommend 24 hours of observation in asymptomatic patients
See Also
External Links
References
- ↑ Bhattacharjee P.. Early histopathologic changes in purple glove syndrome. J Cutan Pathol. 2004;31(7):513-5.
- ↑ Santoshi JA. Purple glove syndrome: a case report. Hand surgeons and physicians be aware. J Plast Reconstr Aesthet Surg. 2010;63(3):e340-2.
- ↑ Scumpia AJ. Purple glove syndrome after intravenous phenytoin administration presenting in the emergency department. J Emerg Med. 2013;44(2):e281-3.