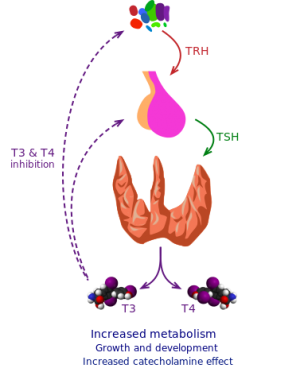
Thyroid storm
Background
- Mortality
- Without treatment: 80-100%
- With treatment: 10-30%[1]
- Difference between severe thyrotoxicosis and thyroid storm is clinical diagnosis[2]
- Must empirically treat before laboratory confirmation
- Death caused by multi-organ dysfunction, congestive heart failure, respiratory failure, dysrhythmias, DIC, hypoxic brain injury, or sepsis [3]
Precipitants
- Long-standing untreated hyperthyroidism
- Infection
- Trauma
- Recent thyroid manipulation (physical or surgical)
- Burns
- Surgery (non-thyroid)
- DKA
- Withdrawal of thyroid medication
- Lithium withdrawal
- Iodine load (contrast media or amiodarone[4])
- MI
- CVA
- PE
- Interferon-α treatment
- Recent parturition
- Molar pregnancy
- Hypoglycemia
- Hyperemesis gravidarum [5]
- Toxemia of pregnancy [6]
Spectrum of Thyroid Disease
- Myxedema coma << hypothyroidism < euthyroid > hyperthyroidism >> thyroid storm
Clinical Features
Classic Triad
- Hyperthermia
- Often marked (40 - 41C)[7]
- Tachycardia
- Often out of proportion to fever [8]
- Altered mental status (agitation, confusion, delirium stupor, coma, seizure)
May also have:
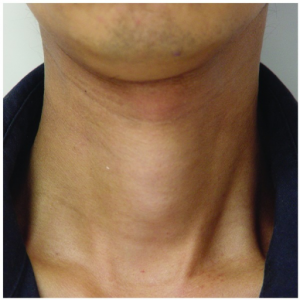
- Goiter
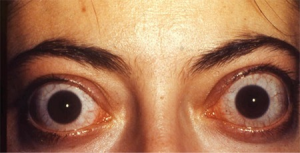
- Thyrotoxic stare, lid retraction
- Hyperhidrosis
- Thermoregulatory dysfunction
- Central nervous system dysfunction
- Gastrointestinal-hepatic dysfunction
- Diarrhea, nausea and vomiting, abdominal pain
- Unexplained jaundice, hepatomegaly
- Cardiovascular dysfunction
- Tachycardia, palpitations
- Congestive heart failure, dyspnea
- Pedal edema
- A. fib
- Widened pulse pressure
Complications
- Cardiovascular collapse[9]
- Hypovolemia, hypotension
- Hepatic failure with cholestatic jaundice [10]
- Rare but carries poor prognosis
Apathetic Hyperthyroidism
- Strikingly different rare form, dominated by depressed mental status, cardiac complications[11]
- Treatment with antithyroid therapy is still mainstay
- More common in elderly patients [12]
Differential Diagnosis
- Sympathomimetic ingestion
- Atherosclerosis
- Aortic regurgitation
- Thyrotoxicosis
- Fever
- Anemia
- Pregnancy
- Anxiety
- Patent ductus arteriosus
- Heart block
- Aortic dissection
- Endocarditis
- Increased ICP
- Vasodilating drugs
- Beriberi
- Pheochromocytoma
Evaluation
Workup
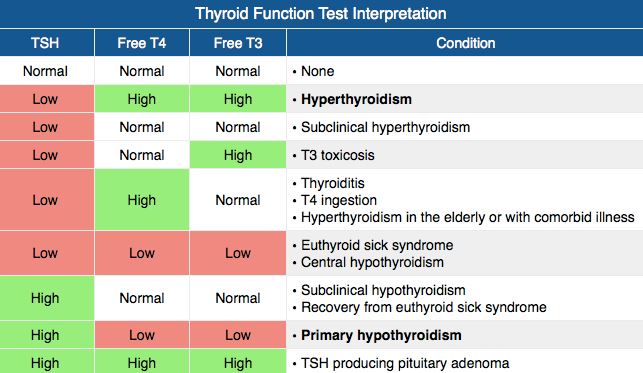
- TSH
- Low or undetectable
- Free T3/T4
- Elevated
- Chemistry
- Calcium may be elevated
- Hyperglycemia often present [13]
- CBC
- May have thrombocytopenia
- Leukocytosis common [14]
- LFTs
- Mild elevation in AST, ALT, LDH, bilirubin, ALP may be seen [15]
- Cortisol level (rule-out concurrent adrenal insufficiency)
- ECG
- Rule out infection:
- CXR
- Blood culture
- UA
- Consider lumbar puncture after CTH
Diagnosis
Burch & Wartofsky Diagnostic Criteria
| Category | Points | ||||
| Thermoregulatory dysfunction (°F) | |||||
|---|---|---|---|---|---|
| Tmax= 99-99.9 | 5 | ||||
| Tmax= 100-100.9 | 10 | ||||
| Tmax= 101-101.9 | 15 | ||||
| Tmax= 102-102.9 | 20 | ||||
| Tmax= 103-103.9 | 25 | ||||
| Tmax= 104 | 30 | ||||
| Central nervous system effects | |||||
| Mild (Agitation) | 10 | ||||
| Moderate (delirium, psychosis, extreme lethargy) | 20 | ||||
| Severe (seizure, coma) | 30 | ||||
| Gastrointestinal-hepatic dysfunction | |||||
| Moderate (diarrhea, nausea and vomiting, abdominal pain) | 10 | ||||
| Severe (unexplained jaundice) | 20 | ||||
| Cardiovascular dysfunction (tachycardia) | |||||
| HR= 99-109 | 5 | ||||
| HR= 110-119 | 10 | ||||
| HR= 120-129 | 15 | ||||
| HR= 130-139 | 20 | ||||
| HR= 140 | 25 | ||||
| Congestive Heart Failure | |||||
| Mild (pedal edema) | 5 | ||||
| Moderate (bibasilar rales) | 10 | ||||
| Severe (pulmonary edema, A. fib) | 15 | ||||
| Precipitant history | |||||
| Negative | 0 | ||||
| Positive | 10 | ||||
Scoring[16]
- >45 = Highly suggestive of thyroid storm
- 25-44 = Suggestive of impending storm
- <25 = Unlikely to represent storm
Management[17]
Identify precipitant (i.e. med noncompliance, DKA, infection). When in doubt of diagnosis, the EP should treat given the high mortality rate, as a few doses of anti-thyroid medication are unlikely to harm euthyroid patient[18]
Supportive care
- Fever
- Do not aggressively cool as this can lead to vasoconstriction[19]
- Careful cooling measures (ice packs & cooling blankets)
- Acetaminophen (avoid aspirin or NSAIDS because they displace thyroid hormone from TBG)
- Dehydration/hypoglycemia
- D5NS (most patients have depleted glycogen stores)
- Crackles in lungs are likely high output heart failure, NOT fluid overload
- Cardiac decompensation (CHF, A-fib)
- Rate control, inotropes, diuretics as needed (short acting always better)
- Agitation
- Benzodiazepines are the preferred agent
Treat Increased Adrenergic Tone
- Propranolol PO 60-80 mg q4hr (if can tolerate PO, no PR form)
- or
- Propranolol IV 1-2mg over 10 min; if tolerates then 1-2mg boluses q15 minutes until HR <100[20]
- Followed by drip at dose required for heart rate control (3-5mg/hr)
- Relative contraindications are same as for other medical conditions (e.g. CHF, Reactive Airway Disease, see alternative therapies)
- In addition to decreasing peripheral conversion, propranolol will improve tremor, hyperpyrexia, and agitation
- Unlike other beta-blockers, propranolol also partially blocks conversion of T4 to T3
- or
- Esmolol 250-500mcg/kg loading dose, then 50-100mcg/kg/min[21]
- B1 selective so can be used with active CHF, asthma, etc
- Does not have T4 to T3 blocking properties of propranolol
- or
- Reserpine 2.5 - 5 mg IM q4h
- Option for patients in whom beta-blockers are contraindicated [22]
Block New Hormone Synthesis[23]
Thionamides are the main class of medications which prevent new hormone synthesis by inhibiting the iodination of tyrosine residues by thyroid peroxidase (TPO) enzymes. Propylthiouracil (PTU) is prefered over methimazole because it will also bock T4→T3 conversion
- PTU 500-1000mg PO or NG followed by 250mg q4hr
- May provide PR, but PO or NG are preferred routes (IV formulations not available in US)
- PTU recommended in the first trimester of pregnancy with transition to methimazole afterwards[24]
- Note black box warning of hepatotoxicity so check LFTs prior
- Avoid in patients with significant liver disease; use methimazole instead
- Theoretically first line and offers advantage over methimazole
- PTU has earlier onset of action and capacity to inhibit peripheral conversion of T4 to T3
- However, no significant difference in mortality between PTU and methimazole[25]
- Methimazole 20-25mg q4hr (80 - 100 mg daily in divided doses)
- Potassium iodide (SSKI)
- Give 1hr after PTU or methimazole to prevent increased hormone production (Jod-Basedow effect)[28]
- Block hormone release: (Wolff-Chaikoff effect) only after hormone synthesis is inhibited. Iodine concentration leads to transient decrease of T3/T4
- 5 drops (0.25 mL or 250mg) orally every 6 hours
- Avoid potassium iodide if patient is on amiodarone
- Can substitute radiocontrast dyes (Iopanoic acid, ipodate and iopanoate), PO Lugol solution, OR IV sodium iodide [29]
- Lithium carbonate[30]
- Consider if iodine allergic
- Lithium carbonate 300mg PO q8hr
- Lithium inhibits thyroid hormone release from the gland and reduces iodination of tyrosine residues, but its use is complicated by the toxicity that can ensue
- Treatment of choice for iodine-induced hyperthyroidism as the result of contrast load or amiodarone
- Lugol’s Solution 8 drops PO q 6 (alternative iodine source)
- Sodium Iodide 0.5mg IV Q 12 hours (alternative iodine source)
- Cholestyramine 1-4g BID PO
- Inhibits enterohepatic circulation of thyroid hormone by binding to conjugated products and promote excretion
Adrenal Insufficiency Treatment
Often there may be associated adrenal insufficiency (also blocks T4>T3)
- Hydrocortisone 300mg IV bolus, followed by 100mg TID for several days OR
- Dexamethasone 4mg IV q6hr
- Note that corticosteroids also inhibit conversion of T4 to T3 and block release of hormone from thyroid gland
Plasmapheresis[31]
- For recalcitrant thyroid storm, with remaining cardiac and neurologic symptoms
- Especially in the case of fulminant liver failure, in which anti-thyroid drugs are contraindicated[32]
- Repeat sessions until TFTs normalize
- Removes cytokines, auto-antibodies, thyroid hormones, thyroid hormone bound proteins
Antibiotics
- Second most common etiology of thyroid storm (after medication noncompliance) is infection [33]
- Low threshold to start broad spectrum antibiotics
Additional Interventions
- Consider L-Carnitine (1 g PO q 12h) - blocks T3 & T4 entry into cell nuclei peripherally [34]
- Consider Cholestyramine (4g PO q 6h) - decreases GI hormone recycling
Disposition
- Admission to ICU
See Also
External Links
References
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders in Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders.
- ↑ Nayak B1, Burman K. Thyrotoxicosis and thyroid storm. Endocrinol Metab Clin North Am. 2006 Dec;35(4):663-86, vii.
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders in Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders.
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders in Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders.
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders in Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders.
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders in Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders.
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders in Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders.
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders in Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders.
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders in Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders.
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders in Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders.
- ↑ Parker KI et al. A case of apathetic thyroid storm with resultant hyperthyroidism-induced hypercalcemia. Am J Med Sci. 2013 Oct;346(4):338-40.
- ↑ Poudel RR et al. Apathetic thyrotoxicosis presenting with diabetes mellitus. J Community Hosp Intern Med Perspect. 2014 4(5).
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders in Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders.
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders in Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders.
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders in Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders.
- ↑ Burch HB, Wartofsky L. Life-threatening thyrotoxicosis. Thyroid storm. Endocrinol Metab Clin North Am. 1993 Jun;22(2):263-77
- ↑ Bahn chair RS, Burch HB, Cooper DS, et al. Hyperthyroidism and other causes of thyrotoxicosis: management guidelines of the American Thyroid Association and American Association of Clinical Endocrinologists. Thyroid. 2011;21(6):593-646.
- ↑ LoPresti J. A New Look at Thyroid Emergencies Part II: Handling Thyroid Storm. http://epmonthly.com/article/a-new-look-at-thyroid-emergencies-part-ii-handling-thyroid-storm/.
- ↑ Chiha, Maguy, Shanika Samarasinghe, and Adam S Kabaker. 2013. Thyroid storm: an updated review. Journal of intensive care medicine, no. 3. http://www.ncbi.nlm.nih.gov/pubmed/23920160.
- ↑ http://emcrit.org/podcasts/thyroid-storm/ EMCrit - Thryoid Storm (149)
- ↑ Brunette DD, Rothong C. Emergency department management of thyrotoxic crisis with esmolol. Am J Emerg Med. 1991;9(3):232-4.
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders in Rosen's Emergency Medicine (9th ed.). Philadelphia, PA: Elsevier/Saunders.
- ↑ Doses based on American Association of Clinical Endocrinologists recommendations
- ↑ Kobaly K, Mandel SJ. Hyperthyroidism and Pregnancy. Endocrinol Metab Clin North Am. 2019 Sep;48(3):533-545. doi: 10.1016/j.ecl.2019.05.002. Epub 2019 Jun 17. PMID: 31345521.
- ↑ Isozaki O et al. Treatment and management of thyroid storm: analysis of the nationwide surveys: The taskforce committee of the Japan Thyroid Association and Japan Endocrine Society for the establishment of diagnostic criteria and nationwide surveys for thyroid storm. Clin Endocrinol (Oxf). 2016; 84(6):912-8 (ISSN: 1365-2265).
- ↑ Kobaly K, Mandel SJ. Hyperthyroidism and Pregnancy. Endocrinol Metab Clin North Am. 2019 Sep;48(3):533-545. doi: 10.1016/j.ecl.2019.05.002. Epub 2019 Jun 17. PMID: 31345521.
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders. Rosen's Emergency Medicine (9th ed). Philadelphia, PA: Elsevier/Saunders.
- ↑ Chiha M. et al Thyroid storm: an updated review. J Intensive Care Med. 2015 Mar;30(3):131-40.
- ↑ Weingart, Scott. EMCRIT Thyroid Storm Show Notes. http://emcrit.org/podcasts/thyroid-storm/
- ↑ Carroll R, Matfin G. Endocrine and metabolic emergencies: thyroid storm. Ther Adv Endocrinol Metab. 2010 Jun; 1(3): 139–145. Full Text
- ↑ Muller C et al. Role of plasma exchange in the thyroid storm. Ther Apher Dial. 2011 Dec;15(6):522-31.
- ↑ Garg N et al. CALMING THE STORM - ROLE OF PLASMAPHERESIS IN THYROTOXIC CRISES. The Endocrine Society's 95th Annual Meeting and Expo, June 15–18, 2013 - San Francisco.
- ↑ Akamizu T, et al. Diagnostic criteria, clinical features, and incidence of thyroid storm based on nationwide surveys. Thyroid 2012; 22:661.
- ↑ Salvatore Benvenga, et al. Effects of carnitine on thyroid hormone action PMID: 15591013 DOI: 10.1196/annals.1320.015