Acute asthma exacerbation
This page is for adult patients. For pediatric patients, see: asthma (peds)
Background
- Establish severity of current presentation based of vital signs, clinical presentation, and history of prior severe exacerbations (e.g. need for hospitalization, ICU admission, intubation, etc.)
- Identify any treatable precipitant (e.g. pneumonia, URI, GERD, exposure to irritants, aspirin/NSAIDs)
- Status asthmaticus is a life-threatening form of asthma in which progressively worsening reactive airways are unresponsive to usual appropriate therapy leading to pulmonary insufficiency.
Clinical Features
- Dyspnea, wheezing, and cough (+/- sputum production)
- Prolonged expiration
- Accessory muscle use
- Sign of impending ventilatory failure:
- Paradoxical respiration (chest deflation and abdominal protrusion during inspiration)
- Altered mental status
- "Silent chest"
- Low peak flows
- Cyanosis is uncommon (respiratory alkalosis -> left shift of the oxyhemoglobin dissociation curve)
Differential Diagnosis
Wheeze
Common (the "Big 3")
- Asthma
- COPD
- Bronchiolitis (peds)
- CHF ("cardiac asthma")
Airway — Intrathoracic Lower
- Aspirated foreign body
- Bronchiectasis
- Bronchiolitis
- Bronchiolitis obliterans
- Pneumonia (focal wheeze)
- Pulmonary embolism
- Carcinoid tumor
- Endobronchial tuberculosis
- Parasitic infection (eosinophilic pneumonia; in endemic areas)
- Hypersensitivity pneumonitis (e.g., farmer's lung)
Airway — Intrathoracic Central
- Aspirated foreign body
- Tracheal stenosis / tumor
- Tracheomalacia
- Mucus plugging
- Vascular ring / aortic aneurysm
- Mediastinal mass / lymphoma
Airway — Extrathoracic (typically stridor ± wheeze)
- Foreign body
- Anaphylaxis
- Angioedema (including ACE inhibitor-induced)
- Croup
- Epiglottitis
- Vocal cord dysfunction / paradoxical vocal fold motion
- Vocal cord edema / paralysis
- Laryngeal stenosis / tumor
- Retropharyngeal abscess
- Peritonsillar abscess
- Tonsillar / adenoid hypertrophy
- Goiter / thyroid mass
- Postnasal drip
Allergic / Inflammatory
- Anaphylaxis
- Allergic bronchopulmonary aspergillosis (ABPA)
- Eosinophilic granulomatosis with polyangiitis (Churg-Strauss)
- Sarcoidosis
Drug-Induced Bronchospasm
- Beta-blocker (including ophthalmic)
- Aspirin / NSAIDs (aspirin-exacerbated respiratory disease)
- ACE inhibitor (cough / bronchospasm)
- Cholinergic agents (e.g., neostigmine)
- Inhaled irritants / smoke inhalation
Other
- GERD / aspiration
- Pneumothorax (decreased breath sounds ± focal wheeze)
- Pulmonary embolism (may present with wheeze in up to 25%)
- Vocal cord dysfunction (often misdiagnosed as refractory asthma)
- Obesity hypoventilation
Acute dyspnea
Emergent
- Pulmonary
- Airway obstruction
- Anaphylaxis
- Angioedema
- Aspiration
- Acute respiratory distress syndrome (ARDS)
- Asthma
- Cor pulmonale
- Epiglottitis
- Inhalation exposure
- Noncardiogenic pulmonary edema
- Pneumonia
- Pneumocystis Pneumonia (PCP)
- Pulmonary embolism
- Pulmonary hypertension
- Tension pneumothorax
- Idiopathic pulmonary fibrosis acute exacerbation
- Cystic fibrosis exacerbation
- Cardiac
- Other Associated with Normal/↑ Respiratory Effort
- Other Associated with ↓ Respiratory Effort
Non-Emergent
- ALS
- Ascites
- Uncorrected ASD
- Congenital heart disease
- COPD exacerbation
- Deconditioning
- Fever
- Hyperventilation
- Interstitial lung disease
- Neoplasm
- Obesity
- Obstructive sleep apnea
- Panic attack
- Pleural effusion
- Polymyositis
- Porphyria
- Pregnancy
- Rib fracture
- Spontaneous pneumothorax
- Thyroid Disease
- URI
- Vocal cord dysfunction
Evaluation
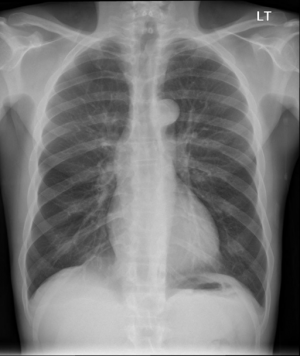
Workup
- For uncomplicated exacerbations in patients with known asthma, CXR is not routinely indicated.[1][2]
- Consider CXR if:
- Asymmetric lung auscultation findings, after treatment with albuterol
- Poor response to medications/treatment, if history and exam are not consistent with asthma
- Worsening symptoms
- Unexplained fever
- Chest pain
Diagnosis
- Normally a clinical diagnosis
- ABG unlikely to add to clinical decision making unless pulse oximetry unavailable
- However, a blood gas with a normal or elevated CO2 suggest impending respiratory failure (asthmatics typically hypocapneic during exacerbation)
Classification
| Severity | Symptom frequency | Night-time symptoms | %FEV1 of predicted | FEV1 variability | SABA use |
|---|---|---|---|---|---|
| Intermittent | ≤2/week | ≤2/month | ≥80% | <20% | ≤2 days/week |
| Mild persistent | >2/week | 3–4/month | ≥80% | 20–30% | >2 days/week |
| Moderate persistent | Daily | >1/week | 60–80% | >30% | daily |
| Severe persistent | Continuously | Frequent (7/week) | <60% | >30% | ≥twice/day |
Management
Oxygen PRN
- Titrate to an arterial oxygen saturation >90% (>95% in pregnant women and with coexistent heart disease)
Albuterol
Favor continuous nebulization to decrease the chance of admission when compared to intermittent dosing[4]
- Nebulizer
- Intermittent: 2.5-5mg q20min x3, then 2.5-10mg q1-4hr as needed OR
- Continuous: 0.5mg/kg/hr (max 15mg/hr)[5]
- If using intermitent nebs at home PTA, start on continuous
- MDI
- 6-12 puffs q20min up to 4h, then q1-4hr as needed
- Levalbuterol is pure R-enantiomer, whereas racemic albuterol as above is 50:50 mix of R and S albuterol
- Levalbuterol at 5x the cost, may not warrant the small benefits seen in some studies
- In severe asthma exacerbation, be aware of lactic acidosis that develops due to pathology and the added lactic acidosis from albuterol,
- Manifests as worsening respiratory distress, tachypnea, compensatory increase in ventilation
- Ensure adequate intravascular volume, but carefully volume expand as acute asthma may increase ADH secretion[8]
- Rarely, clinically important hypokalemia, alongside hyperglycemia and leukocytosis, may result from repeated beta agonists and sympathomimetics[9]
Ipratropium[10][11]
- 0.25-0.5mg q20min x2-3 doses
- Only shown to be effective in the acute setting to reduce hospitalization rates and improve lung function
- No benefit of adding to inpatient, hospitalized regimens
Steroids
Should be given in the first hour with effects to reduce admission and rate of relapses[12] Options include:
- Dexamethasone
- As effective as prednisone especially in children [13]
- Single dose dexamethasone may be equally effective to 5 days of prednisone in adults[14]
- 0.6mg/kg IV or PO (max 16mg); 2nd dose 24hr later may be an equally good option as single dose therapy [15]
- Prednisone
- 40-60mg /day x5d
- Methylprednisolone
- 1mg/kg IV q 4–6hr
- Only use IV if cannot tolerate PO since equal effectiveness between dosing routes[16]
- Oral and IV steroids are safe during pregnancy (though technically Category C)
- Inhaled corticosteroids may be considered as a rescue effort for severe asthma, given over a 90 min period[17][18]
- Nebulized fluticasone 500 µg q15 min
- Nebulized budesonide 800 µg q30 min
Magnesium
- 25-75 mg/kg over 30 min (2-3 g IV in most adults)
- Duration of action approximately 20 min, beware of hypotension in rapid administration due to smooth muscle relaxation mechanism
- In patients with moderate to severe asthma there is a decreased rate of admission with an NNT of 2[12]
- High-dose, prolonged magnesium may expedite discharge from the ED in non-infectious asthma in pediatric study[19]
- 50 mg/kg/hr for 4 hours
- MAX 8,000 mg for 4 hours, monitor for cardiopulmonary complications
- No interventions or discontinuations of magnesium sulfate due to adverse events in the study
- NNT of 2-3, for hospital discharge before 24 hours
Other Beta-Agonists
- Inhalation is preferred route of administration, but adequate drug delivery to small airways may be hampered in severe attacks
- Terbutaline and epinephrine can be administered IM/IV/SubQ
- Need to monitor for arrhythmias, tachycardia, hypertension, cardiac ischemia[20]
Epinephrine
- 1:1000 0.01 mg/kg (max 0.5mg) subQ or IM Q20min x3
- Nebulized racemic epinephrine 0.03 mL/kg (2.25% solution) diluted in 3-5 mL NS via jet nebulizer q3-4hr PRN shown to be as safe as nebulized albuterol[21]
- In severe, life-threatening asthma, IV epinephrine may be safe to consider, substantiated only by a case series of adults in 2003, however[22]
- Epinephrine infusion for adults at 5mcg/min (0.05mcg/kg/min for pediatrics) after requiring multiple epinephrine doses.
Terbutaline
- Longer-acting beta2-agonist promoting bronchodilation
- Caution in elderly/CHF with greater potential for cardiotoxicity
- 0.25mg subQ/IM q20min x 3
- Then followed by infusion at 1 µg/kg/min, titrated up by increments of 1 to max of 10 1 µg/kg/min
- Elevated troponins q4hrs during infusion, more common in cTnI vs. cTnT, with EKG changes of ischemia should prompt re-evaluation for stopping infusion[23]
- Some experts have nebulized IV form[24][25]
- Terbutaline 5 mg IV
- More expensive than albuterol
Non-invasive ventilation
- Consider as alternative to intubation or pre-oxygenation prior to intubation
- Alleviates muscle fatigue which leads to larger tidal volumes
- May drive nebulized treatments deeper into airways
- Maximize inspiratory support
- Inspiratory pressure 8
- PEEP 0-3, only enough to match patient's auto-PEEP
Intubation and Invasive Ventilation
- Relative indications include worsening hypercapnea, exhaustion, altered mental status, CO2 narcosis without any specific number endpoint on blood gases, refractory hypoxemia, status asthmaticus
- Consider induction with Ketamine
- Provides bronchodilation and sedation however it does promote secretions
- Ketamine is the preferred induction agent for intubation in an asthmatic.
- Dosing 1-2mg/kg
- Ventilation of asthmatic patients requires deep sedation
- Initial ventilation settings - severe asthma
- Assist-control ventilation
- Resp rate
- Start slow to avoid air-trapping
- RR ~ 8-10 in adults
- Goal: obtaining a pH above 7.2 and plateau pressure below 30 cmH2O[27]
- If Pplat >30 must lower respiratory rate
- If Pplat under 30 cannot be maintained, other causes of decreased respiratory system compliance must be considered (i.e. pneumothorax, misplaced endotracheal tube, pulmonary edema, etc.)
- May require "permissive hypoventilation"
- Sacrifice MV for full exhalation
- Lower I:E ratio
- Low peak pressure/avoidance of breath stacking more important than correcting CO2 [28]
- Tidal volume 6-8mL/kg ideal wt
- PEEP 0-5 cmH2O
- Flow rate 80-100L/min
- Keep FiO2 minimum to achieve SpO2 > 90%
- Use bronchodilators even when intubated
- Monitor for breath stacking (inspiratory holds, plateau pressures)
- Most common cause of post-intubation hypotension[29]
- Check ventilator tracing
Asthma Arrest
- Disconnect ventilator
- Decompress chest
- Consider empiric bilateral chest tubes or rapid ultrasound to identify pneumothorax
- IVF bolus
Antibiotics
- Administration of antibiotics only when physical exam or ancillary testing supportive of bacterial infection
- Antibiotics may be considered for select patients and may improve symptoms and peak expiratory flow, further understanding needed to identify which patients may be most likely to benefit [30]
Heliox
- 60 to 80% helium is blended with 20 to 40% oxygen
- Heliox improves laminar flow and may increase the diffusion of carbon dioxide by improving ventilation[31]
Leukotriene Modifiers
- Not indicated for acute treatment
- Zafirlukast (20 mg bid) and montelukast (10 mg/day)
Outpatient Treatment
New guidelines by Global Initiative for Asthma (GINA) 2019 endorse the use of an ICS-LABA combined product as both rescue and maintenance inhaler based off of a 2018 meta analysis [32]
- GINA recommends budesonide or beclomethasone as the inhaled corticosteroid, and formoterol as the long acting beta agonist. The only U.S. formulation meeting this recommendation is Symbicort (budesonide-formoterol).
| Severity | Day Sx | Night Sx | Treatment (WHO 2008 Formulary)[33] |
| Mild intermittent, > 80% peak flow | < 2/wk | < 2/mo | Albuterol MDI 100-200 mcg PRN QID |
| Mild persistent, > 80% peak flow | >2/wk | >2/mo | Albuterol MDI 100-200 mcg PRN QID AND
Beclometasone 100-250 mcg bid |
| Moderate persistent, 60-80% peak flow | Daily with exacerbations weekly | > 1/wk | Albuterol MDI 100-200 mcg PRN QID AND
Beclometasone 100-500 mcg BID AND Salmeterol inhaled 50 mcg bid |
| Severe persistent, < 60% peak flow | Continuous daily | Frequent | Albuterol MDI 100-200 mcg PRN QID AND
Beclometasone 1mg BID (high dose) AND Salmeterol inhaled 50 mcg BID AND (if needed) theophylline, leukotriene antagonist, or PO prednisolone with taper |
Disposition
Discharge
- If symptoms resolve
- Often, patients will still have mild wheezing, but should have complete resolution of tachypnea, hypoxia, and work of breathing if being discharged
- A short course of glucocorticoids decreases chance of relapse[34] - prednisone in adults (40-60 mg/day for 5-10 days without tapering) or dexamethasone (0.6mg/kg) in children
Admit
- If symptoms persist or are severe
- Classically disposition is based on peak flow measurements - however, these measurements are often not available in the ED
- Predicted = (30 x age (yrs)) + 30
- PEF >70% predicted → high likelihood of successful discharge
- PEF <40% predicted → should be admitted
See Also
- Asthma (peds)
- Modified pulmonary index score
- Ventilation settings
- Deterioration after intubation
- COPD exacerbation
External Links
References
- ↑ Sakr M, et al. A Quality Improvement Initiative to Minimize Unnecessary Chest X-Ray Utilization in Pediatric Asthma Exacerbations. Pediatr Qual Saf. 2024 Apr 3;9(2):e721. doi: 10.1097/pq9.0000000000000721.
- ↑ Sher et al. Int J Crit Care Emerg Med 2022, 8:142
- ↑ Yawn BP (September 2008). "Factors accounting for asthma variability: achieving optimal symptom control for individual patients" (PDF). Primary Care Respiratory Journal. 17 (3): 138–47. doi:10.3132/pcrj.2008.00004. PMC 6619889. PMID 18264646.
- ↑ Camargo CA et al. Continuous versus intermittent beta- agonists for acute asthma. Cochrane Database Syst Rev. 2003;(4):CD001115. PMID: 14583926.
- ↑ National Asthma Education and Prevention Program (NAEPP), “Expert Panel Report 3 (EPR-3): Guidelines for the Diagnosis and Management of Asthma,” Clinical Practice Guidelines, National Institutes of Health, National Heart, Lung, and Blood Institute, NIH Publication No. 08-4051, prepublication 2007; available at http://www.nhlbi.nih.gov/guidelines/asthma/asthgdln.htm.
- ↑ Ralston ME, Euwema MS, Knecht KR, Ziolkowski TJ, Coakley TA, Cline SM. Comparison of levalbuterol and racemic albuterol combined with ipratropium bromide in acute pediatric asthma: a randomized controlled trial. J Emerg Med. 2005;29(1):29-35.
- ↑ Qureshi F, Zaritsky A, Welch C, Meadows T, Burke BL.Clinical efficacy of racemic albuterol versus levalbuterol for the treatment of acute pediatric asthma. Ann Emerg Med. 2005;46(1):29-36.
- ↑ Qureshi F. Management of children with acute asthma in the emergency department. Pediatr Emerg Care. 1999;15(3):206-214.
- ↑ Leikin JB et al. Hypokalemia after pediatric albuterol overdose: a case series. Am J Emerg Med. 1994 Jan;12(1):64-6.
- ↑ Goggin N, Macarthur C, Parkin PC. Randomized trial of the addition of ipratropium bromide to albuterol and corticosteroid therapy in children hospitalized because of an acute asthma exacerbation. Arch Pediatr Adolesc Med. 2001;155(12):1329-1334.
- ↑ Rodrigo GJ, Rodrigo C. The role of anticholinergics in acute asthma treatment: an evidence-based evaluation. Chest. 2002;121(6):1977-1987.
- ↑ 12.0 12.1 Rowe BH et al. Magnesium sulfate for treating exac- erbations of acute asthma in the emergency depart- ment. Cochrane Database Syst Rev. 2000;(2):CD001490. PMID: 10796650.
- ↑ Keeney, et al. Dexamethasone for Acute Asthma Exacerbations in Children: A Meta-analysis. Pediatrics. 2013-2273
- ↑ Rehrer MW et al. A randomized controlled noninferiority trial of single dose of oral dexamethasone versus 5 days of oral prednisone in acute adult asthma. Ann Emerg Med 2016 Apr 22.
- ↑ Kratitz J et al. Two Days of Dexamethasone Versus 5 Days of Prednisone in the Treatment of Acute Asthma: A Randomized Controlled Trial. Ann Emerg Med. 2011 Aug;58(2):200-4. PMID: 2133409
- ↑ Rowe BH, Keller JL, Oxman AD. Effectiveness of steroid therapy in acute exacerbations of asthma: a meta-analysis. Am J Emerg Med. Jul 1992;10(4):301-10
- ↑ Rodrigo GJ. Inhaled Corticosteroids as Rescue Medication in Acute Severe Asthma. Expert Rev Clin Immunol. 2008;4(6):723-729.
- ↑ Volovitz B. Inhaled budesonide in the management of acute worsenings and exacerbations of asthma: a review of the evidence. Respir Med. 2007 Apr;101(4):685-95.
- ↑ Irazuzta J et al. High-Dose Magnesium Sulfate Infusion for Severe Asthma in the Emergency Department: Efficacy Study. Pediatric Critical Care Medicine. 17(2):e29–e33, FEBRUARY 2016.
- ↑ Scarfone RJ, Friedlaender EY.beta2-Agonists in acute asthma: the evolving state of the art. Pediatr Emerg Care. 2002;18(6):442-427.
- ↑ Plint AC, Osmond MH, Klassen TP. The efficacy of nebulized racemic epinephrine in children with acute asthma: a randomized, double-blind trial. Acad Emerg Med. 2000;7(10):1097-1103.
- ↑ Smith D et al. Intravenous epinephrine in life-threatening asthma. Annals of Emerg Med. May 2003. Volume 41, Issue 5, Pages 706–711.
- ↑ Kalyanaraman M et al. Serial cardiac troponin concentrations as marker of cardiac toxicity in children with status asthmaticus treated with intravenous terbutaline. Pediatr Emerg Care. 2011 Oct;27(10):933-6.
- ↑ Lin YZ, Hsieh KH, Chang LF, Chu CY.Terbutaline nebulization and epinephrine injection in treating acute asthmatic children. Pediatr Allergy Immunol. 1996;7(2):95-99.
- ↑ Rodrigo GJ, Nannini LJ. Comparison between nebulized adrenaline and beta2 agonists for the treatment of acute asthma. A meta-analysis of randomized trials. Am J Emerg Med. 2006;24(2):217-222.
- ↑ Adnet F, Dhissi G, Borron SW, et al. Complication profiles of adult asthmatics requiring paralysis during mechanical ventilation. Intensive Care Med. 2001;27(11):1729-1736.
- ↑ Stather DR, Stewart TE. Clinical review: Mechanical ventilation in severe asthma. Crit Care. 2005;9(6):581-587.
- ↑ Darioli, et al. Mechanical Controlled hypoventilation in status asthmaticus. Am Rev Respir Dis. 1984; 129 (3) 385-7
- ↑ Williams TJ, Tuxen DV, Scheinkestel CD, et al. Risk factors for morbidity in mechanically ventilated patients with acute severe asthma. Am Rev Respir Dis. 1992;146(3):607-615.
- ↑ Ganti L, Rosario J, Do Antibiotics Improve Outcomes in Patients With Acute Asthma Exacerbations? An of Emrg Med. 2019; 74(5) : 711–712.
- ↑ Kass JE: Heliox redux. Chest 2003; 123:673.
- ↑ Sobieraj, Diana M., et al. “Association of Inhaled Corticosteroids and Long-Acting β-Agonists as Controller and Quick Relief Therapy With Exacerbations and Symptom Control in Persistent Asthma.” Jama, vol. 319, no. 14, Oct. 2018, p. 1485., doi:10.1001/jama.2018.2769.
- ↑ Stuart MC et al. WHO Model Formulary 2008. http://www.who.int/selection_medicines/list/WMF2008.pdf.
- ↑ Chapman K. Effect of a short course of prednisone in the prevention of early relapse after the emergency room treatment of acute asthma. NEJM. 1991;324(12):788