Crohn's disease
Background
- Can involve any part of the GI tract from the mouth to the anus
- Bimodal distribution: 15-22yr, 55-60yr
- Pathology
- All layers of the bowel are involved
- Reason why fistulas and abscesses are common complications
- "Skip lesions" are common
- All layers of the bowel are involved
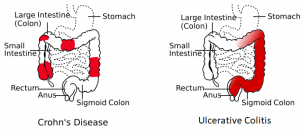
Crohn's disease vs. ulcerative colitis
| Finding | Crohn's disease | Ulcerative colitis |
| Depth of inflammation | May be transmural, deep into tissues | Shallow, mucosal |
| Distribution of disease | Patchy areas of inflammation (skip lesions) | Continuous area of inflammation |
| Terminal ileum involvement | Commonly | Seldom |
| Colon involvement | Usually | Always |
| Rectum involvement | Seldom | Usually (95%) |
| Involvement around anus | Common | Seldom |
| Stenosis | Common | Seldom |
Clinical Features
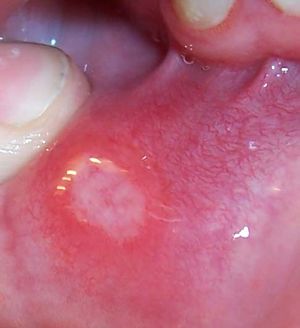
An aphthous mouth ulcer (aphthous stomatitis) on seen with Crohn's disease.
GI Symptoms
- Abdominal pain
- Diarrhea
- Weight loss
- Perianal fissures or fistulas
Extraintestinal Symptoms (50%)
- Arthritis
- Peripheral arthritis
- Migratory monoarticular or polyarticular
- Ankylosing spondylitis
- Pain/stiffness of spine, hips, neck, rib cage
- Sacroiliitis
- Low back pain with morning stiffness
- Peripheral arthritis
- Ocular
- Uveitis
- Acute blurring of vision, photophobia, pain, perilimbic scleral injection
- Episcleritis
- Eye burning or itching with out visual changes or pain; scleral and conj hyperemia
- Uveitis
- Dermatologic
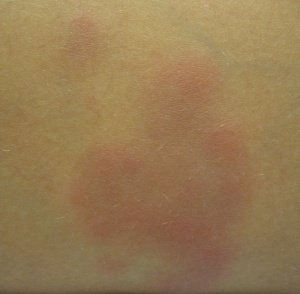
- Erythema nodosum
- Painful, red, raised nodules on extensor surfaces of arms/legs
- Pyoderma gangrenosum
- Violaceous, ulcerative lesions with necrotic center found in pretibial region or trunk
- Erythema nodosum
- Hepatobiliary
- Cholelithiasis (33%)
- Fatty liver
- Autoimmune hepatitis
- Primary sclerosing cholangitis
- Cholangiocarcinoma
- Renal
- Increased risk for calcium oxalate stones due to hyperoxaluria
- Vascular
Differential Diagnosis
Colitis
- Viral gastroenteritis
- Bacterial gastroenteritis
- Campylobacter infections
- Clostridium difficile colitis
- Colon cancer
- Crohn disease
- Cryptosporidiosis
- Mycobacterium Avium-Intracellulare
- Toxic megacolon
- Ulcerative colitis
- Ischemic bowel disease (e.g. mesenteric ischemia, strangulated hernia)
- Pseudomembranous enterocolitis
- Lymphoma
- Ileocecal amebiasis
- Sarcoidosis
- Yersinia
- Campylobacter
Other
Evaluation
Work-Up
- Rule out alternate etiologies for symptoms
- Evaluate for complications (e.g. fistulae, abscess, obstruction)
- Labs
- Consider imaging:
- CT A/P if concern for small bowel obstruction, perforation, or toxic megacolon
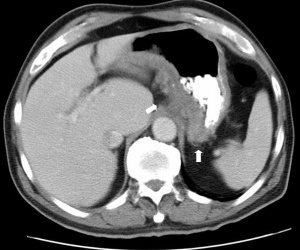
- Most useful diagnostic test in patients with acute symptoms who have known or suspected Crohn
- Findings: bowel wall thickening, mesenteric edema, local abscess, fistulas
- CT A/P if concern for small bowel obstruction, perforation, or toxic megacolon
Diagnosis
Management
Acute Flare Management
- IVF
- Bowel rest
- Analgesia
- Electrolyte correction
- Consider steroid burst
- Methylprednisolone (e.g., 30mg IV bid) or prednisone (e.g., 60 mg day 1, then 40 mg daily x 4 days), OR
- Budesonide for mild to moderate disease due to fewer systemic side effects
- Antidiarrheals are contraindicated
Chronic Treatment
Alterations should be discussed with GI
- Aminosalicylates (5-ASA) - Mild-to-moderate Crohn's disease. Give with probiotics.
- Sulfasalazine 3-5gm/day PO (sulfa drug)
- Caution: Can cause folate deficiency so give with folic acid, and can cause hemolytic anemia in G6PD patients
- Mesalamine 4gm/day PO
- Active moiety of sulfasalazine, and formed from prodrug balsalazide
- Balsalazide or Olsalazine - Bypasses small intestine to deliver drug into large intestine (better for UC)
- Sulfasalazine 3-5gm/day PO (sulfa drug)
- Anti-diarrheal - Use caution in patients with active inflammation as can precipitate toxic megacolon
- Loperamide 4-16mg/day
- Diphenoxylate 5-20mg/day
- Cholestyramine 4g once to six times daily
- Glucocorticoids - Symptomatic relief (course not altered)
- Prednisone - 40-60mg/day with taper once remission induced
- Methylprednisolone 20mg IV q6hr
- Hydrocortisone 100mg q8hr
- Do not start if any suspicion of infection (ie C. diff colitis)
- Double edge sword: Reduction of bone density in addition to underlying disease process(decreased Ca absorption)
- Antibiotics - Induce remission
- Ciprofloxacin 500mg q8-12hr OR
- Metronidazole 500mg q6hr OR
- Rifaximin 800mg BID
- Immunomodulators - Steroid-sparing agents used in fistulas and patients with surgical contraindication. Slower onset.
- 6-Mercaptopurine 1-1.5mg/kg/day → Start at 50mg daily
- Azathioprine 2-2.5mg/kg/day → Start at 50mg daily
- Methotrexate IM
- Anti-TNF - Medically resistant moderate-to-severe Crohn's disease
- Infliximab (Remicade) 5mg/kg IV
- Adalimumab (Humira), Natalizumab or certolizumab pegol can also be used
Medication Dosing
Methylprednisolone 20mg IV q6hr IV Prednisone 40-60mg daily with taper once remission induced PO
Disposition
Inpatient Admission
- Significant metabolic derangements (i.e. electrolyte imbalance or severe dehydration)
- Fulminate colitis
- Obstruction
- Peritonitis
- Significant hemorrhage
Surgical Intervention
Consult EARLY if any of the following suspicions
- Perforation
- Abscess/fistula formation
- Toxic megacolon
- Significant hemorrhage
- Perianal disease
- Failed medical management
Complications
- Bowel obstruction
- Due to stricture or bowel wall edema
- Abscess
- Fistula
- Occurs due to extension of intestinal fissure into adjacent structures
- Suspect if changes in patient's symptoms (e.g. BM frequency, amt of pain, wt loss)
- Perianal disease
- Hemorrhage
- Erosion into a bowel wall vesel
- Toxic megacolon
- Can be associated with massive GI bleeding
Therapy complications
See Also
References
- ↑ van Rheenen PF, Van de Vijver E, Fidler V. Faecal calprotectin for screening of patients with suspected inflammatory bowel disease: diagnostic meta-analysis. BMJ. 2010;15(341):c3369.
1. Thomas N, Wu AW. Large intestine. In: Walls RM, Hockberger RS, Gausche-Hill M, et al., eds. Rosen’s Emergency Medicine: Concepts and Clinical Practice. 10th ed. Elsevier; 2023.