Peptic ulcer disease
(Redirected from PUD)
Background
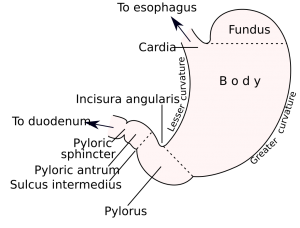
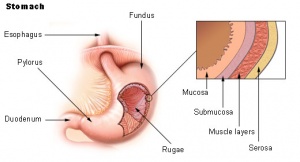
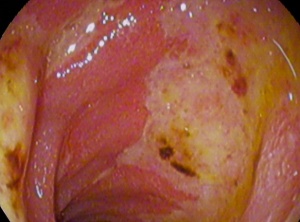
- Recurrent ulcerations in the stomach and proximal duodenum
- Defect in the gastric or duodenal wall that extends through the muscularis mucosa into the deeper layers of the wall[1]
- Majority of cases related to H. pylori or NSAID use
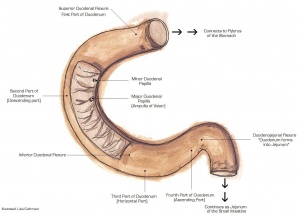
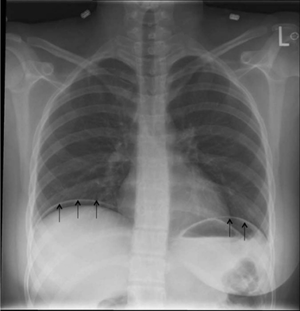
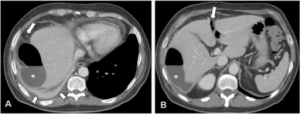
- Perforation most commonly occurs in anterior wall of duodenum.
Clinical Features
Non-Perforated
- Burning epigastric pain
- May awaken patient at night (gastric contents empty)
- Abrupt onset of severe pain may indicate perforation
- Abrupt onset of back pain may indicate penetration into the pancreas
- The following symptoms are NOT associated with PUD:
- Postprandial pain, food intolerance, nausea, retrosternal pain, belching
Perforated
- Abrupt onset of severe epigastric pain
- Patients may not have history of ulcer-like symptoms
Differential Diagnosis
Epigastric Pain
- Gastroesophageal reflux disease (GERD)
- Peptic ulcer disease with or without perforation
- Gastritis
- Pancreatitis
- Gallbladder disease
- Myocardial Ischemia
- Splenic Infarctionenlargement/rupture/aneurysm
- Pericarditis/Myocarditis
- Aortic dissection
- Hepatitis
- Pyelonephritis
- Pneumonia
- Pyogenic liver abscess
- Fitz-Hugh-Curtis Syndrome
- Hepatomegaly due to CHF
- Bowel obstruction
- SMA syndrome
- Pulmonary embolism
- Bezoar
- Ingested foreign body
Upper gastrointestinal bleeding
- Peptic ulcer disease (most common cause)
- Gastritis/esophagitis
- Gastric/esophageal varices
- Mallory-Weiss tear
- Malignancy
- Aortoenteric fisulta
- Boerhaave
- Dieulafoy's lesion
- Angiodysplasia
- Hemobilia
- Hemorrhagic gastritis, EtOH
- Celiac disease
- Dengue
- Other intrabdominal bleeds
- Lower GI bleeding
- Hemorrhagic pancreatitis
- Splenic rupture
- Subcapsular cavernous hemangiomas
- Peliosis hepatis
Mimics of GI Bleeding
- Hemoptysis
- Vaginal/Urethra bleeding
- ENT bleeding
- Dietary (Iron, bismuth, beets)
- Swallowed maternal blood (in neonate)
Evaluation
Work-Up
- CBC (rule out anemia)
- LFTs
- Lipase
- Consider acute abdominal series if concern for perforation (>50 years old; concerning abdominal exam)
- Consider RUQ US
- Consider ECG
- Consider troponin
Evaluation
- Diagnosis not typically definitively made in ED (requires endoscopy or H. pylori test)
- Depending on clinical certainty can consider initial empiric treatment
Management
Perforated
Surgical emergency
- Consult surgery
- Antibiotics to cover abdominal flora
- IVF
Non-Perforated
- Stop NSAIDs and ETOH
- PPI
- Generally heal ulcers faster than H2 blockers[2]
- Omeprazole 20-40mg QD
- H2 blocker
- Famotidine 20-40mg QD
- Ranitidine 75-150mg BID
- Eradicate H. pylori if identified in symptomatic patient
- Triple Therapy: PPI + clarithromycin 500mg BID + (amoxicillin 1g or metronidazole 500mg) BID x 10-14d
- Quadruple Therapy: PPI + bismuth subsalicylate 524mg QID + metronidazole 250mg QID and tetracycline 500mg QID x 10-14d
Disposition
- Normally outpatient management, unless complication (see below)
Red Flags
Any of the following suggest need for endoscopy referral:
- Age >55yr
- Unexplained weight loss
- Early satiety
- Persistent vomiting
- Dysphagia
- Anemia or GI bleeding
- Abdominal mass
- Persistent anorexia
- Jaundice
Complications
- Perforation (see above)
- Hemorrhage
- Obstruction, due to:
- Scarring of gastric outlet
- Edema due to active ulcer
See Also
References
- ↑ Vakil N. Peptic ulcer disease: Management. UpToDate. https://www.uptodate.com/contents/peptic-ulcer-disease-management?search=ulcer treatment&source=search_result&selectedTitle=1~150&usage_type=default&display_rank=1#H1. Published September 16, 2019. Accessed November 5, 2019.
- ↑ Walan A, Bader JP, Classen M, Lamers CB, Piper DW, Rutgersson K, Eriksson S. Effect of omeprazole and ranitidine on ulcer healing and relapse rates in patients with benign gastric ulcer. N Engl J Med. 1989 Jan 12;320(2):69-75. doi: 10.1056/NEJM198901123200201. PMID: 2643037.