Acute hepatic failure/es: Difference between revisions
Ostermayer (talk | contribs) (Created page with "Insuficiencia hepática aguda") |
Ostermayer (talk | contribs) (Created page with "===Encefalopatía (cambio en el estado mental)===") |
||
| Line 7: | Line 7: | ||
===Definiciones=== | ===Definiciones=== | ||
*Insuficiencia hepática hiperaguda: la encefalopatía ocurre dentro de los 7 días del inicio de la ictericia; este subgrupo es probable que sobreviva con manejo médico a pesar de la alta incidencia de edema cerebral<ref>O’Grady, JG, Schalm SW, Williams R. Acute liver failure: redefining the syndromes. Lancet. July 1993, Volume 342, Issue 8866, Page 273-275</ref> | |||
* | *Insuficiencia hepática aguda: intervalo de 8-28 días desde la ictericia hasta la encefalopatía; este subgrupo tiene una alta incidencia de edema cerebral y un peor pronóstico sin trasplante de hígado<ref>O’Grady, JG, Schalm SW, Williams R. Acute liver failure: redefining the syndromes. Lancet. July 1993, Volume 342, Issue 8866, Page 273-275</ref> | ||
* | *Insuficiencia hepática subaguda: intervalo de 5-12 semanas desde el inicio de la ictericia hasta el inicio de la encefalopatía; este subgrupo tiene una menor incidencia de edema cerebral, pero un mal pronóstico<ref>O’Grady, JG, Schalm SW, Williams R. Acute liver failure: redefining the syndromes. Lancet. July 1993, Volume 342, Issue 8866, Page 273-275</ref> | ||
* | |||
{{Acute hepatitis causes}} | {{Acute hepatitis causes}} | ||
| Line 18: | Line 16: | ||
===Otras Causas Raras de Insuficiencia Hepática Aguda=== | |||
=== | |||
*'''[[Special:MyLanguage/Wilson's disease|Wilson's disease]]''': elevaciones inexplicadas en las pruebas de función hepática, síntomas neuropsiquiátricos, anillos de Kayser-Fleischer en el examen ocular | |||
*'''[[Special:MyLanguage/Wilson's disease|Wilson's disease]]''': | *'''[[Special:MyLanguage/Autoimmune hepatitis|Autoimmune hepatitis]]''': más común en mujeres, enfermedad hepática sin explicación, puede tener antecedentes familiares de otros trastornos autoinmunes | ||
*'''[[Special:MyLanguage/Autoimmune hepatitis|Autoimmune hepatitis]]''': | *'''[[Special:MyLanguage/Hemochromatosis|Hemochromatosis]]''': antecedentes familiares de enfermedad hepática y enfermedad cardíaca | ||
*'''[[Special:MyLanguage/Hemochromatosis|Hemochromatosis]]''': | *'''[[Special:MyLanguage/Budd-Chiari|Budd-Chiari]]''': historia de trastorno hipercoagulable, dolor abdominal y ascitis | ||
*'''[[Special:MyLanguage/Budd-Chiari|Budd-Chiari]]''': | |||
==Características clínicas== | |||
= | |||
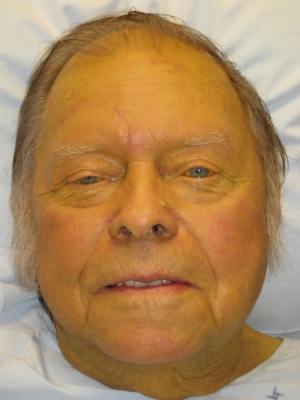
[[File:Jaundice08.jpg|thumb|Ictericia de la piel]] | |||
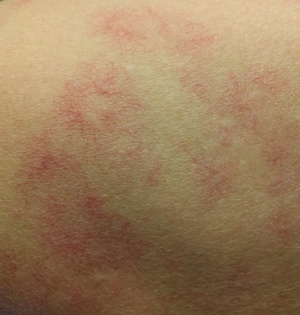
[[File:Jaundice08.jpg|thumb| | [[File:SpiderAngioma.jpg|thumb|Angioma en araña]] | ||
[[File:SpiderAngioma.jpg|thumb| | [[File:Hepaticfailure.jpg|thumb||Ascitis secundaria a [[Special:MyLanguage/cirrhosis|cirrosis]].]] | ||
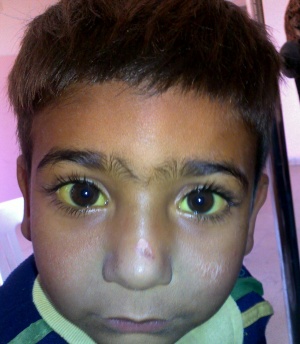
[[File:Hepaticfailure.jpg|thumb|| | [[File:Jaundice.jpg|thumb|Ictericia pediátrica con ictericia de la esclera.]] | ||
[[File:Jaundice.jpg|thumb| | *Hallazgos comunes en la insuficiencia hepática aguda | ||
* | **[[Special:MyLanguage/hepatomegaly|Hepatomegalia]] dolorosa | ||
** | **[[Special:MyLanguage/Jaundice|Ictericia]] | ||
**[[Special:MyLanguage/Jaundice| | **[[Special:MyLanguage/Hepatic encephalopathy|Encefalopatía hepática]] | ||
**[[Special:MyLanguage/Hepatic encephalopathy| | |||
**Asterixis | **Asterixis | ||
* | *Hallazgos comunes en la insuficiencia hepática crónica | ||
**[[Special:MyLanguage/Ascites| | **[[Special:MyLanguage/Ascites|Ascitis]] | ||
**Caput medusae | **Caput medusae | ||
** | **Eritema palmar | ||
** | **Angiomas en araña | ||
** | **Ginecomastia | ||
** | **Atrofia testicular | ||
** | **Enlargement de la glándula parótida | ||
** | **Atrofia muscular | ||
** | **También puede tener [[Special:MyLanguage/jaundice|ictericia]], [[Special:MyLanguage/hepatic encephalopathy|encefalopatía]], y asterixis como en la insuficiencia hepática aguda | ||
==Diagnóstico diferencial== | |||
= | |||
===[[Special:MyLanguage/Encephalopathy|Encefalopatía]] (cambio en el estado mental)=== | |||
===[[Special:MyLanguage/Encephalopathy| | |||
*[[Special:MyLanguage/Hypoglycemia|Hipoglicemia]] | |||
*[[Special:MyLanguage/Hypoglycemia| | *[[Special:MyLanguage/Hypoxia|Hipoxia]] | ||
*[[Special:MyLanguage/Hypoxia| | *[[Special:MyLanguage/Intracerebral hemorrhage|Hemorragia intracerebral]] o masa | ||
*[[Special:MyLanguage/Intracerebral hemorrhage| | *[[Special:MyLanguage/Meningitis|Meningitis]]/[[Special:MyLanguage/encephalitis|encefalitis]] | ||
*[[Special:MyLanguage/Meningitis|Meningitis]]/[[Special:MyLanguage/encephalitis| | *[[Special:MyLanguage/CVA|Accidente cerebrovascular]] | ||
*[[Special:MyLanguage/CVA| | *[[Special:MyLanguage/Alcohol intoxication|Intoxicación alcohólica]] | ||
*[[Special:MyLanguage/Alcohol intoxication| | *[[Special:MyLanguage/Myxedema coma|Coma mixédemico]] | ||
*[[Special:MyLanguage/Myxedema coma| | *[[Special:MyLanguage/Wernicke encephalopathy|Encefalopatía de Wernicke]] | ||
*[[Special:MyLanguage/Wernicke encephalopathy|Wernicke | |||
*[[Special:MyLanguage/Sepsis|Sepsis]] | *[[Special:MyLanguage/Sepsis|Sepsis]] | ||
*[[Special:MyLanguage/Seizure| | *[[Special:MyLanguage/Seizure|Convulsión]]/estado post-ictal | ||
*[[Special:MyLanguage/Uremia|Uremia]] | *[[Special:MyLanguage/Uremia|Uremia]] | ||
*[[Special:MyLanguage/Electrolyte abnormality| | *[[Special:MyLanguage/Electrolyte abnormality|Anomalía electrolítica]] | ||
*[[Special:MyLanguage/Acute hepatic failure| | *[[Special:MyLanguage/Acute hepatic failure|Insuficiencia hepática aguda]] | ||
Revision as of 21:55, 12 January 2026
Antecedentes
Definiciones
- Insuficiencia hepática hiperaguda: la encefalopatía ocurre dentro de los 7 días del inicio de la ictericia; este subgrupo es probable que sobreviva con manejo médico a pesar de la alta incidencia de edema cerebral[1]
- Insuficiencia hepática aguda: intervalo de 8-28 días desde la ictericia hasta la encefalopatía; este subgrupo tiene una alta incidencia de edema cerebral y un peor pronóstico sin trasplante de hígado[2]
- Insuficiencia hepática subaguda: intervalo de 5-12 semanas desde el inicio de la ictericia hasta el inicio de la encefalopatía; este subgrupo tiene una menor incidencia de edema cerebral, pero un mal pronóstico[3]
Causas de hepatitis aguda
- Toxicidad por paracetamol (causa más común de insuficiencia hepática aguda en EE.UU.[4])
- Hepatitis viral
- Toxoplasmosis
- Hepatitis alcohólica aguda
- Tóxicos
- Hepatitis isquémica
- Hepatitis autoinmune
- Enfermedad de Wilson
Drug or Toxin Related Liver Disease
- Liver damage from drugs or toxins may be cytotoxic from the primary drug or its metabolites, or may be caused by veno-occlusive disease or hypersensitivity disease[5]
- Common Drugs and Toxins
- Acetaminophen
- Amiodarone
- Amphotericin
- Anabolic steroids
- Azathioprine
- Carbamazepine
- Chlorpromazine
- Cisplatin
- Contraceptives
- Cyclophosphamide
- Erythromycin
- Gold salts
- Haloperidol
- Isoniazid
- Ketoconazole
- Lovastatin
- Methotrexate
- Methoxyflurane
- Methyldopa
- Phenobarbital
- Phenytoin
- Quinidine
- Salicylates
- Tetracycline
- Valproic acid
- Verapamil
Otras Causas Raras de Insuficiencia Hepática Aguda
- Wilson's disease: elevaciones inexplicadas en las pruebas de función hepática, síntomas neuropsiquiátricos, anillos de Kayser-Fleischer en el examen ocular
- Autoimmune hepatitis: más común en mujeres, enfermedad hepática sin explicación, puede tener antecedentes familiares de otros trastornos autoinmunes
- Hemochromatosis: antecedentes familiares de enfermedad hepática y enfermedad cardíaca
- Budd-Chiari: historia de trastorno hipercoagulable, dolor abdominal y ascitis
Características clínicas
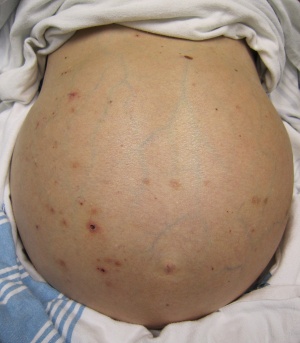
Ascitis secundaria a cirrosis.
- Hallazgos comunes en la insuficiencia hepática aguda
- Hepatomegalia dolorosa
- Ictericia
- Encefalopatía hepática
- Asterixis
- Hallazgos comunes en la insuficiencia hepática crónica
- Ascitis
- Caput medusae
- Eritema palmar
- Angiomas en araña
- Ginecomastia
- Atrofia testicular
- Enlargement de la glándula parótida
- Atrofia muscular
- También puede tener ictericia, encefalopatía, y asterixis como en la insuficiencia hepática aguda
Diagnóstico diferencial
Encefalopatía (cambio en el estado mental)
- Hipoglicemia
- Hipoxia
- Hemorragia intracerebral o masa
- Meningitis/encefalitis
- Accidente cerebrovascular
- Intoxicación alcohólica
- Coma mixédemico
- Encefalopatía de Wernicke
- Sepsis
- Convulsión/estado post-ictal
- Uremia
- Anomalía electrolítica
- Insuficiencia hepática aguda
- Hepatic dysfunction
- Biliary disease (e.g. CBD obstruction)
- Hemolysis
- Pregnancy
- Congenital diseases (e.g. inborn errors of metabolism; (more likely to present in early childhood)
Hepatic Dysfunction
Infectious
- Hepatitis
- Malaria
- HIV (present in 50% of AIDS patients)[6]
- EBV
- Babesiosis, leptospirosis
- Typhoid
- Hepatic abscess, amebiasis
Neoplastic
Metabolic
Biliary
- Biliary cirrhosis
Drugs
- Alcoholic cirrhosis
- Alcoholic hepatitis
- Hepatotoxic drugs
Miscellaneous
- Other causes of cirrhosis
- Autoimmune hepatitis
- Veno-occlusive disease
- CHF (right heart failure)
Evaluation
Labs
- LFTs
- AST and ALT
- Enzymes found mainly in hepatic cells, though ALT is more specific to the liver than AST
- Extreme elevation in AST (>3000U/L, or >40x upper limit of normal) is consistent with acetaminophen toxicity or ischemic injury
- Moderate elevations (10-40x upper limit of normal) is consistent with viral hepatitis
- Mild elevations (<10x upper limit of normal) is consistent with alcoholic hepatitis
- Alkaline Phosphatase
- Found in bile canaliculi (but also in placenta, ileal mucosa, bone, and kidney)
- Elevated in diseases of cholestasis
- Rare for levels to be >3x normal limit in acute liver failure
- Bilirubin
- Elevated in diseases of cholestasis
- In obstructive diseases, the direct bilirubin will usually be about 50% of the total bilirubin; if indirect bilirubin is higher, more suggestive of hemolysis or problem with conjugation
- AST and ALT
- Coagulation Studies
- Reflects the liver’s ability to synthesize clotting factors
- INR >6.5 or PT >20 seconds indicates patients at high risk for death
- Albumin
- Reflects synthetic function of the liver
- Has a long half-life (20 days) and may not be decreased early in disease
- Ammonia
- Elevated as a result of impaired clearance
- Poor correlation between degree of elevation and severity of encephalopathy symptoms
- Chemistry Panel
- Electrolyte abnormalities may indicate malnutrition or dehydration
- Creatinine is used as a prognostic indicator
- Need to check a glucose because patients with liver failure are prone to hypoglycemia
- CBC
- Not useful in diagnosing the cause of liver failure, but helpful in determining coexisting infection, anemia, thrombocytopenia
- Viral hepatitis Serologies
- Consider for all patients with undifferentiated liver failure
- IgM anti-HBc may be the only positive marker in acute Hepatitis B infection
- Anti-HCV and HCV RNA are present in both chronic and acute Hepatitis C infections, so it is difficult to differentiate based on serologies, but presence of HCV RNA in the absence of anti-HCV is more suggestive of acute infection[7]
- Only need to test for IgM anti-HEV in patients who are symptomatic and have just travelled from areas where Hepatitis E is endemic
Imaging
- Consider RUQ US or CT in patients with jaundice to evaluate for a mechanical obstruction
- Otherwise, tailor imaging towards specific complaints
Diagnóstico del ascitis
El diagnóstico diferencial del ascitis frecuentemente se aclara mediante el cálculo del gradiente de albúmina sérica al ascítico (SAAG).^
- SAAG alto > 1.1 g/dL – Indicativo de hipertensión portal[8]
- Cirrosis
- Insuficiencia cardíaca
- Ascitis con proteína total > 2.5 g/dL sugiere ascitis cardíaca[9]
- Hepatitis alcohólica
- Síndrome de Budd-Chiari
- Trombosis de vena portal
- SAAG bajo < 1.1 g/dL
- Malignidad / carcinomatosis peritoneal
- Síndrome nefrótico
- Pancreatitis
- Tuberculosis peritoneal
- Serositis
- Infarto intestinal
- Quiloso
- ^SAAG = (albúmina sérica en g/dL) − (albúmina ascítica en g/dL)
Management
- Treatment is mostly supportive and tailored towards the specific etiology
- Early consideration regarding transporting patient to a transplant center given potential for rapid deterioration
- Symptom specific supportive treatment options
- Encephalopathy: consider lactulose of neomycin
- Seizures: consider phenytoin over benzodiazepines (prevent benzodiazepine oversedation secondary to decreased hepatic clearance)
- Intracranial Hypertension: elevated head of bed, mannitol, short-term hyperventilation; hypothermia may be a bridge to transplant; no benefit from steroids
- Coagulopathy
- Prophylactic normalization of the INR is not necessary unless procedure (such as paracentesis) is planned; then can give Vitamin K
- Recommend platelet transfusion to 10K for asymptomatic patients, and to 50-70K for patients undergoing invasive procedures
- See Acetaminophen toxicity for specifics regarding treatment of acetaminophen toxicity
- See Spontaneous Bacterial Peritonitis for specifics regarding diagnosis and treatment of SBP
Disposition
- Admission to ICU with early consideration for transportation to transplant center
See Also
References
- ↑ O’Grady, JG, Schalm SW, Williams R. Acute liver failure: redefining the syndromes. Lancet. July 1993, Volume 342, Issue 8866, Page 273-275
- ↑ O’Grady, JG, Schalm SW, Williams R. Acute liver failure: redefining the syndromes. Lancet. July 1993, Volume 342, Issue 8866, Page 273-275
- ↑ O’Grady, JG, Schalm SW, Williams R. Acute liver failure: redefining the syndromes. Lancet. July 1993, Volume 342, Issue 8866, Page 273-275
- ↑ Ostapowicz G, Fontana RJ, Schiodt FV, et al. Results of a prospective study of acute liver failure at 17 tertiary care centers in the United States. Ann Intern Med. 2002 Dec 17; 137(12): 947-54.
- ↑ Oyama, LC: Disorders of the Liver and Biliary Tractin Marx JA, Hockberger RS, Walls RM, et al (eds): Rosen’s Emergency Medicine: Concepts and Clinical Practice, ed 8. St. Louis, Mosby, Inc., 2014, (Ch) 107: p 1186-1204
- ↑ Tintanelli's
- ↑ Bailey, C, Hern HG. Hepatic Failure: An Evidence-Based Approach In The Emergency Department. Emergency Medicine Practice. Vol. 12, No. 4, 2014.
- ↑ Runyon BA. Management of adult patients with ascites due to cirrhosis: update 2012. Amer Assoc Study Liv Dis. 2012; 1-96.
- ↑ Runyon BA. Cardiac ascites: a characterization. J Clin Gastro. 1998; 10(4): 410-412.